![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
226 Cards in this Set
- Front
- Back
|
What are the important genes of embryogenesis? |
- Sonic hedgehog (Shh)
- Wnt-7 gene - FGF gene - Homeobox (Hox) genes |
|
|
Where is the Sonic hedgehog gene produced? Function?
|
- Produced at base of limbs in zone of polarizing activity
- Involved in patterning along anterior-posterior axis - Involved in CNS development |
|
|
What can a mutation in Sonic hedgehog gene cause?
|
Holoprosencephaly
|
|
|
Where is the Wnt-7 gene produced? Function?
|
- Produced at apical ectodermal ridge (thickened ectoderm at distal end of each developing limb)
- Involved in proper organization along dorsal-ventral axis |
|
|
Where is the FGF gene produced? Function?
|
- Produced at apical ectodermal ridge (thickened ectoderm at distal end of each developing limb)
- Stimulates mitosis of underlying mesoderm, providing for lengthening of limbs |
|
|
What is the function of the Homeobox (Hox) genes?
|
Involved in segmental organization of embryo in a craniocaudal direction
|
|
|
What can a mutation in Homeobox (Hox) gene cause?
|
Appendages in wrong locations
|
|
|
What gene is necessary for patterning along the anterior-posterior axis?
|
Sonic hedgehog gene
|
|
|
What gene is necessary for organization along the dorsal-ventral axis?
|
Wnt-7 gene
|
|
|
What gene stimulates mitosis of the underlying mesoderm, allowing for the lengthening of limbs?
|
FGF gene
|
|
|
What gene is involved in the segmental organization of embryo in a craniocaudal direction?
|
Homeobox (Hox) gene
|
|
|
A mutation in what gene can cause holoprosencephaly?
|
Sonic hedgehog gene
|
|
|
A mutation in what gene can cause appendages in wrong locations?
|
Homeobox (Hox) genes
|
|
|
What happens on day 0 of fetal development?
|
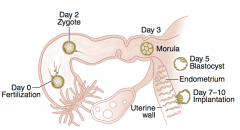
Fertilization of egg by sperm (in fallopian tube)
|
|
|
What happens during the first week of fetal development?
|
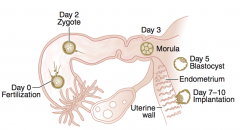
Formation of:
- Zygote (day 2) - Morula (day 3) - Blastocyst (day 5) Implantation of Blastocyst |
|
|
What happens during the second week of fetal development?
|
- Formation of Bilaminar disc: Epiblast and Hypoblast
- 2 weeks = 2 layers |
|
|
What happens during the third week of fetal development?
|
Formation of Trilaminar disc
- 3 weeks = 3 layers Gastrulation - Formation of primitive streak, notochord, mesoderm and its organization, and neural plate |
|
|
What happens during the "embryonic period"? When does this occur?
|
- Neural tube formed by neuroectoderm and closes by week 4
- Organogenesis (weeks 3-8) |
|
|
During what period is the fetus extremely susceptible to teratogens?
|
Weeks 3-8 (embryonic period) - this is when organogenesis takes place
|
|
|
What forms the neural tube? When does it close?
|
- Formed by neuroectoderm
- Closes by week 4 |
|
|
When does the heart begin to beat?
|
Week 4
|
|
|
When do the limb buds start to form?
|
Week 4
(4 weeks = 4 limbs) |
|
|
When is fetal cardiac activity visible by transvaginal ultrasound?
|
Week 6
|
|
|
When do the genitalia begin to display distinctive male/female characteristics?
|
Week 10
|
|
|
What is the process that forms the trilaminar embryonic disc?
|
Gastrulation
|
|
|
What occurs during gastrulation?
|
Formation of trilaminar embryonic disc (3 germ layers):
- Ectoderm - Mesoderm - Endoderm |
|
|
How does gastrulation begin?
|
Starts with the epiblast invaginating to form the primitive streak
|
|
|
What are the embryologic derivatives of the ectoderm?
|
- Surface ectoderm
- Neuroectoderm - Neural crest |
|
|
What are the embryologic derivatives of the surface ectoderm?
|
- Adenohypophysis (from Rathke pouch)
- Lens of eye - Epithelial lining of oral cavity - Sensory organs of ear - Olfactory epithelium - Epidermis - Anal canal below pectinate line - Parotid, sweat, and mammary glands |
|
|
What is the embryologic origin of the adenohypophysis (anterior pituitary)?
|
Rathke pouch - from surface ectoderm
|
|
|
What kind of tumor forms from a remnant of the Rathke pouch? Characteristics?
|
Craniopharyngioma
- Benign Rathke pouch tumor - With cholesterol crystals and calcifications |
|
|
What types of glands originate from surface ectoderm?
|
- Parotid glands
- Sweat glands - Mammary glands |
|
|
What types of epithelium originate from surface ectoderm?
|
- Epithelium of oral cavity
- Olfactory epithelium |
|
|
What are the embryological derivatives of the neuroectoderm?
|
Think CNS:
- Brain (including neurohypophysis, CNS neurons, oligodendrocytes, astrocytes, ependymal cells, pineal gland) - Retina - Optic nerve - Spinal cord |
|
|
What are the embryological derivatives of the neural crest?
|
Think PNS and non-neural structures nearby:
- PNS (including dorsal root ganglia, cranial nerves, celiac ganglion, Schwann cells, ANS) - Melanocytes - Chromaffin cells of adrenal medulla - Parafollicular (C) cells of thyroid - Pia and arachnoid mater - Bones of skull - Odontoblasts - Aorticopulmonary septum |
|
|
Which non-PNS structures originate from the neural crest?
|
- Melanocytes
- Chromaffin cells of adrenal medulla - Parafollicular (C) cells of thyroid - Pia and arachnoid mater - Bones of skull - Odontoblasts - Aorticopulmonary septum |
|
|
What components of the PNS originate from the neural crest?
|
- Dorsal root ganglia
- Cranial nerves - Celiac ganglion - Schwann cells - ANS |
|
|
What are the embryologic derivatives of the mesoderm?
|
- Muscle, bone, CT
- Serous linings of body cavities (eg, peritoneum) - Spleen (from foregut mesentery) - Cardiovascular structures - Lymphatics - Blood - Wall of gut tube - Vagina - Kidneys - Adrenal cortex - Dermis - Testes and ovaries |
|
|
What signal tells the ectoderm to form the neuroectoderm?
|
Notochord induces ectoderm to form neuroectoderm
|
|
|
What is the postnatal derivative of the notochord?
|
Nucleus pulposus of the intervertebral disc
|
|
|
What are the possible defects caused by problems with the development of the mesodermal derivatives?
|
VACTERL:
- Vertebral defects - Anal atresia - Cardiac defects - Trachio-Esophageal fistula - Renal defects - Limb defects (bone and muscle) |
|
|
What are the derivatives of the endoderm?
|
- Gut tube epithelium (up to anal canal above pectinate line)
- Most of urethra (from urogenital sinus) - Luminal epithelial derivatives (eg, lungs, liver, gallbladder, pancreas, eustachian tube, thymus, parathyroid, thyroid follicular cells) |
|
|
What are the luminal epithelial derivatives of the endoderm?
|
- Lungs
- Liver - Gallbladder - Pancreas - Eustachian tube - Thymus - Parathyroid - Thyroid follicular cells |
|
|
What are the cells of the thyroid derived from?
|
- Parafollicular (C) cells of thyroid: neural crest (ectoderm)
- Thyroid follicular cells: endoderm |
|
|
What are the types of errors in organ morphogenesis?
|
- Agenesis
- Aplasia - Hypoplasia - Deformation - Disruption - Malformation - Sequence |
|
|
What is the term for the absence of an organ due to absent primordial tissue?
|
Agenesis
|
|
|
What is the term for absent organ despite presence of primordial tissue?
|
Aplasia
|
|
|
What is the term for incomplete organ development with primordial tissue present?
|
Hypoplasia
|
|
|
What is the term for an extrinsic disruption, that occurs after the embryonic period?
|
Deformation
|
|
|
What is the term for the secondary breakdown of a previously normal tissue or structure (eg, amniotic band syndrome)?
|
Disruption
|
|
|
What is the term for the intrinsic disruption of an organ that occurs during the embryonic period (weeks 3-8)?
|
Malformation
|
|
|
What is the term for abnormalities that result from a single primary embryological event (eg, oligohydramnios → )?
|
Sequence
(eg, Potter sequence) |
|
|
What is the difference between a deformation and a malformation?
|
- Deformation: extrinsic disruption, occurs after embryonic period
- Malformation: intrinsic disruption, occurs during embryonic period (weeks 3-8) |
|
|
When are fetuses most susceptible to teratogens?
|
3rd-8th weeks (embryonic period - organogenesis)
|
|
|
What happens if a fetus is exposed to a teratogen before week 3?
|
All or none effects
|
|
|
What happens if a fetus is exposed to a teratogen after week 8?
|
Growth and function affected
|
|
|
What is the effect on the fetus, of a mother taking ACE inhibitors during her pregnancy?
|
Renal damage
|
|
|
What is the effect on the fetus, of a mother taking alkylating agents during her pregnancy?
|
- Absence of digits
- Multiple anomalies |
|
|
What is the effect on the fetus, of a mother taking aminoglycosides during her pregnancy?
|
CN VIII toxicity ("a mean guy hit the baby in the ear")
|
|
|
What is the effect on the fetus, of a mother taking carbamazepine during her pregnancy?
|
- Neural tube defects
- Craniofacial defects - Fingernail hypoplasia - Developmental delay - IUGR |
|
|
What is the effect on the fetus, of a mother taking Diethylstilbestrol (DES) during her pregnancy?
|
- Vaginal clear cell adenocarcinoma
- Congenital Müllerian anomalies |
|
|
What is the effect on the fetus, of a mother taking folate antagonists during her pregnancy?
|
Neural tube defects
|
|
|
What is the effect on the fetus, of a mother taking Lithium during her pregnancy?
|
Ebstein Anomaly (atrialized RV)
|
|
|
What is the effect on the fetus, of a mother taking Methimazole during her pregnancy?
|
Aplasia cutis congenita
|
|
|
What is the effect on the fetus, of a mother taking Phenytoin during her pregnancy?
|
Fetal Hydantoin Syndrome:
- Microcephaly - Dysmorphic craniofacial features - Hypoplastic nails and distal phalanges - Cardiac defects - IUGR - Intellectual disability |
|
|
What is the effect on the fetus, of a mother taking Tetracycline antibiotics during her pregnancy?
|
Discolored teeth
|
|
|
What is the effect on the fetus, of a mother taking Thalidomide during her pregnancy?
|
Limb defects:
- Phocomelia - Micromelia - "Flipper" limbs |
|
|
What is the effect on the fetus, of a mother taking Valproate during her pregnancy?
|
Inhibition of maternal folate absorption → neural tube defects
|
|
|
What is the effect on the fetus, of a mother taking Warfarin during her pregnancy?
|
- Bone deformities
- Fetal hemorrhage - Abortion - Ophthalmologic abnormalities "Do not wage WARFARe on the baby, keep it HEPpy with HEParin (does not close the placenta) |
|
|
Which medication taken during pregnancy can cause renal damage?
|
ACE-Inhibitors
|
|
|
Which medication taken during pregnancy can cause absence of digits?
|
Alkylating agents
|
|
|
Which medication taken during pregnancy can cause CN VIII toxicity?
|
Aminoglycosides
|
|
|
Which medication taken during pregnancy can cause neural tube defects?
|
- Carbamazepine
- Folate antagonists - Valproate |
|
|
Which medication taken during pregnancy can cause fingernail hypoplasia?
|
- Carbamazepine
- Phenytoin |
|
|
Which medication taken during pregnancy can cause Intrauterine Growth Restriction?
|
- Carbamazepine
- Phenytoin |
|
|
Which medication taken during pregnancy can cause vaginal clear cell adenocarcinoma?
|
Diethylstilbestrol (DES)
|
|
|
Which medication taken during pregnancy can cause congenital Müllerian anomalies?
|
Diethylstilbestrol (DES)
|
|
|
Which medication taken during pregnancy can cause Ebstein anomaly?
|
Lithium (atrialized RV)
|
|
|
Which medication taken during pregnancy can cause aplasia cutis congenita?
|
Methimazole
|
|
|
Which medication taken during pregnancy can cause fetal hydantoin syndrome?
|
Phenytoin
- Microcephaly - Dysmrophic craniofacial features - Hypoplastic nails and distal phalanges - Cardiac defects - IUGR - Intellectual disability |
|
|
Which medication taken during pregnancy can cause discolored teeth?
|
Tetracycline
|
|
|
Which medication taken during pregnancy can cause limb defects?
|
Thalidomide
|
|
|
Which medication taken during pregnancy can cause bone deformities?
|
Warfarin
|
|
|
Which medication taken during pregnancy can cause fetal hemorrhage?
|
Warfarin
|
|
|
Which medication taken during pregnancy can cause ophthalmologic abnormalities?
|
Warfarin
|
|
|
What is a common cause of birth defects and intellectual disability?
|
Alcohol (Fetal Alcohol Syndrome)
|
|
|
What are the effects of a mother taking cocaine while pregnant?
|
- Abnormal fetal growth
- Fetal addiction - Placental abruption |
|
|
What is a leading cause of low birth weight in developed countries?
|
Smoking (nicotine, CO)
|
|
|
What is smoking during pregnancy associated with?
|
- Low birth weight
- Preterm labor - Placental problems - IUGR - ADHD |
|
|
How does the amount of iodine in the diet of the mother affect a fetus?
|
Iodine (lack or excess) → congenital goiter or hypothyroidism (cretinism)
|
|
|
What are the possible consequences to the fetus of having a mother with maternal diabetes?
|
- Caudal regression syndrome (anal atresia to sirenomelia)
- Congenital heart defects - Neural tube defects |
|
|
What are the possible consequences of having excess Vitamin A on the fetus?
|
Extremely high risk for spontaneous abortions and birth defects:
- Cleft palate - Cardiac abnormalities |
|
|
What are the possible consequences of a mother receiving x-rays while she is pregnant?
|
- Microcephaly
- Intellectual disability |
|
|
What is one of the leading causes of congenital malformations in US?
|
Fetal Alcohol Syndrome
|
|
|
What abnormalities are associated with Fetal Alcohol Syndrome?
|
- Intellectual disability
- Pre- and post-natal developmental retardation - Microcephaly - Holoprosencephaly - Facial abnormalities (smooth philtrum, tin upper lip, small palpebral fissures, hypertelorism) - Limb dislocation - Heart defects |
|
|
What do dizygotic twins arise from?
|
2 eggs, separately fertilized by 2 different sperm → two zygotes
|
|
|
How many amniotic sacs and placentas (chorions) can dizygotic twins have?
|
- 2 separate amniotic sacs
- 2 separate placentas (chorions) |
|
|
What do monozygotic twins arise from?
|
- 1 fertilized egg + 1 sperm
- Splits into 2 zygotes in early pregnancy |
|
|
What determines the degree of separation between monozygotic twins?
|
Depends on when the fertilized egg splits into 2 zygotes: determines the number of chorions and the number of amnions
|
|
|
What are the results of cleavage of a zygote during days 0-4?
|
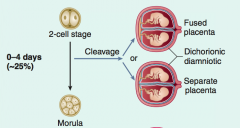
Dichorionic and Diamniotic
|
|
|
What are the results of cleavage of a zygote during days 4-8?
|
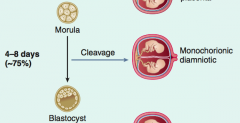
Monochorionic and Diamniotic
|
|
|
What are the results of cleavage of a zygote during days 8-12?
|
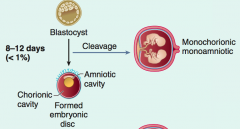
Monochorionic and Monoamniotic
|
|
|
What are the results of cleavage of a zygote after day 13?
|
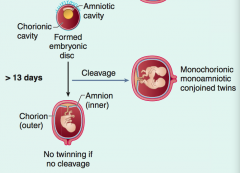
Monochorionic and Monoamniotic; conjoined twins
|
|
|
Which is more common: monozygotic or dizygotic twins?
|
- Monozygotic (20%)
- Dizygotic (80%) |
|
|
What is the primary site of nutrient and gas exchange between the mother and fetus?
|
Placenta
|
|
|
What are the fetal components of the placenta?
|
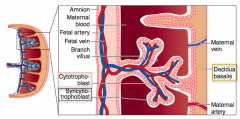
- Cytotrophoblast
- Syncytiotrophoblast |
|
|
What is the maternal component of the placenta?
|
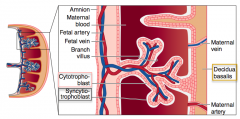
Decidua basalis
|
|
|
What are the layers of the chorionic villi? Which is inner/outer?
|
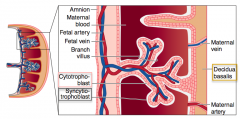
- Inner: cytotrophoblast
- Outer: syncytiotrophoblast |
|
|
What is the function of the cytotrophoblast?
|
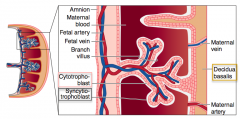
Inner layer of chorionic villi (fetal component of placenta)
- Cytotrophoblast makes Cells |
|
|
What is the function of the syncytiotrophoblast?
|
Outer layer of chorionic villi (fetal component of placenta)
- Secretes hCG → stimulates corpus luteum to secrete progesterone during first trimester |
|
|
What is hormone is hCG similar to structurally? Source in placenta?
|
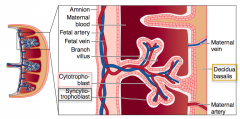
- Structurally similar to LH
- Secreted from syncytiotrophoblast (outer layer of chorionic villi) - Stimulates corpus luteum to secrete progesterone during first trimester |
|
|
What is the origin of the decidua basalis? What is in it?
|
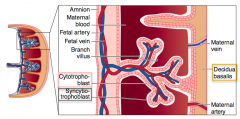
Maternal component of placenta
- Derived from endometrium - Maternal blood is found in lacunae |
|
|
What are the contents of the umbilical cord?
|
- 2 umbilical arteries
- 1 umbilical vein |
|
|
What structure returns deoxygenated blood from the fetal internal iliac arteries to the placenta?
|
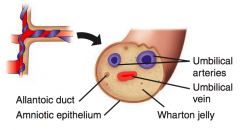
Umbilical arteries
|
|
|
What structure supplies oxygenated blood from the placenta to the fetus?
|
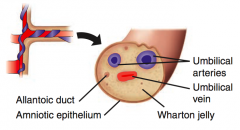
Umbilical vein
|
|
|
What does the umbilical vein flow into?
|
Drains into the IVC via the liver or via the ductus venosus
|
|
|
What is a single umbilical artery associated with?
|
Associated with congenital and chromosomal anomalies
|
|
|
What are the umbilical arteries (2) and vein (1) derived from?
|
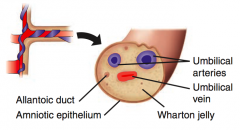
Allantois
|
|
|
What is the origin of the allantois?
|
In the third week, the yolk sac forms the allantois
|
|
|
What does the allantois extend into?
|
Urogenital sinus
|
|
|
What does the allantois become?
|
Becomes the urachus: a duct between the fetal bladder and yolk sac
|
|
|
What does the urachus connect?
|
Duct between the fetal bladder and yolk sac
|
|
|
What are the potential complications if the urachus fails to obliterate?
|
- Patent urachus
- Urachal cyst - Vesicourachal diverticulum |
|
|
What causes urine discharge from the umbilicus?
|
Patent urachus (failure of urachus to obliterate)
|
|
|
What can cause formation of a fluid-filled cavity lined with uroepithelium between the umbilicus and bladder? What is this called?
|
Urachal Cyst
- Partial failure of urachus to obliterate |
|
|
What is a urachal cyst? Cause? What can it lead to?
|
- Fluid-filled cavity lined with uroepithelium
- Caused by a partial failure of the urachus to obliterate - Can lead to infection or adenocarcinoma |
|
|
What is the name for an outpouching of the bladder caused by the failure of the urachus to obliterate?
|
Vesicourachal diverticulum
|
|
|
What is the function of the vitelline duct?
|
Connects yolk sac to midgut lumen
(aka Omphalo-Mesenteric Duct) |
|
|
What can a failure of the vitelline duct to close result in?
|
- Vitelline fistula
- Meckel diverticulum |
|
|
What causes meconium discharge from the umbilicus?
|
Vitelline Fistula (due to failure of the vitelline duct to close)
|
|
|
What causes melena, periumbilical pain, and ulcers?
|
Meckel Diverticulum (due to partial closure of the vitelline duct)
|
|
|
What are the characteristics / cause of a Vitelline Fistula?
|
- Failure of vitelline duct to close
- Meconium discharges from umbilicus |
|
|
What are the characteristics / cause of a Meckel Diverticulum?
|
- Partial closure of Vitelline duct with patent portion attached to ileum (true diverticulum)
- May have ectopic gastric mucosa and/or pancreatic tissue → melena, periumbilical pain, and ulcers |
|
|
What do the aortic arch derivatives develop into?
|
Arterial system
|
|
|
What is the derivative of the 1st aortic arch?
|
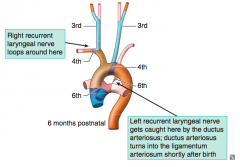
Part of maxillary artery (branch of external carotid)
*1st arch is MAXimal* |
|
|
What is the derivative of the 2nd aortic arch?
|
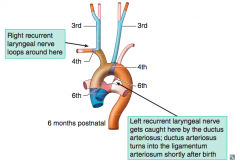
Stapedial artery and hyoid artery
*Second arch = Stapedial* |
|
|
What is the derivative of the 3rd aortic arch?
|
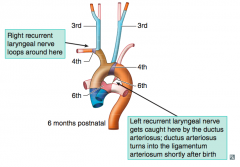
- Common Carotid artery
- Proximal part of internal Carotid artery *C = 3rd letter of alphabet* |
|
|
What is the derivative of the 4th aortic arch?
|
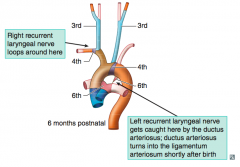
- On left: aortic arch
- On right: proximal part of R subclavian artery *4th arch (4 limbs) = systemic* |
|
|
What is the derivative of the 5th aortic arch?
|
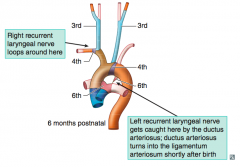
No 5th aortic arch!
|
|
|
What is the derivative of the 6th aortic arch?
|
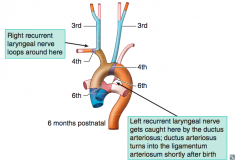
- Proximal part of pulmonary arteries
- On left: ductus arteriosus *6th arch = pulmonary and the pulmonary-to-systemic shunt (ductus arteriosus)* |
|
|
What is the maxillary artery derived from?
|
1st aortic arch
|
|
|
What is the stapedial artery derived from?
|
2nd aortic arch
|
|
|
What is the hyoid artery derived from?
|
2nd aortic arch
|
|
|
What is the common carotid artery derived from?
|
3rd aortic arch
|
|
|
What is the proximal part of the internal carotid artery derived from?
|
3rd aortic arch
|
|
|
What is the aortic arch derived from?
|
Left 4th aortic arch
|
|
|
What is the proximal part of the right subclavian artery derived from?
|
Right 4th aortic arch
|
|
|
What is the proximal part of the pulmonary arteries derived from?
|
6th aortic arch
|
|
|
What is the ductus arteriosus derived from?
|
Left 6th aortic arch
|
|
|
What are the components of the branchial / pharyngeal apparatus?
|
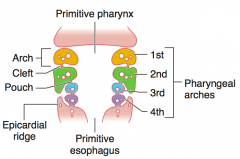
From outside to inside:
- Branchial clefts - Branchial arches - Branchial pouches |
|
|
What are the branchial clefts derived from?
|
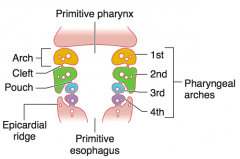
Derived from ectoderm
|
|
|
What are the branchial arches derived from?
|
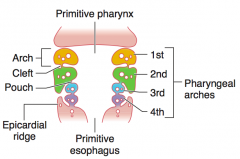
Derived from mesoderm (muscles arteries) and neural crest (bones, cartilage)
|
|
|
What are the branchial pouches derived from?
|
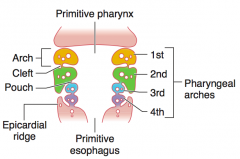
Derived from endoderm
|
|
|
How many pharyngeal arches are there?
|
Four
|
|
|
What is the derivative of the 1st branchial cleft?
|
External auditory meatus
|
|
|
What is the derivative of the 2nd-4th branchial clefts?
|
Temporary cervical sinuses (obliterated by proliferation of 2nd arch mesenchyme)
|
|
|
What happens if there is a persistent cervical sinus?
|
Formation of branchial cleft cyst within lateral neck
|
|
|
What are the cartilaginous derivatives of the 1st branchial arch?
|
Meckel Cartilage:
- Mandible - Malleus - Incus - Spheno-manidbular ligament |
|
|
What are the muscular derivatives of the 1st branchial arch?
|
- Muscles of mastication (temporalis, masseter, lateral and medial pterygoids)
- Mylohyoid - Anterior belly of digastric - Tensor tympani - Tensor veli palatini |
|
|
What are the nervous derivatives of the 1st branchial arch?
|
CN V2 and V3 (for chewing)
|
|
|
What are the implications of abnormalities of the derivatives of the 1st branchial arch?
|
Treacher Collins Syndrome:
- 1st-arch neural crest fails to migrate → mandibular hypoplasia, facial abnormalities |
|
|
What are the cartilaginous derivatives of the 2nd branchial arch?
|
Reichert Cartilage:
- Stapes - Styloid process - Lesser horn of hyoid - Stylohyoid ligament |
|
|
What are the muscular derivatives of the 2nd branchial arch?
|
- Muscles of facial expression
- Stapedius - Stylohyoid - Platysma - Belly of digastric |
|
|
What are the nervous derivatives of the 2nd branchial arch?
|
CN VII (facial expression)
|
|
|
What are the implications of abnormalities of the derivatives of the 2nd branchial arch?
|
Congenital Pharyngocutaneous Fistula:
- Persistence of cleft and pouch → fistula between tonsillar area and lateral neck |
|
|
What are the cartilaginous derivatives of the 3rd branchial arch?
|
Cartilage: greater horn of hyoid
|
|
|
What are the muscular derivatives of the 3rd branchial arch?
|
Stylopharyngeus
|
|
|
What are the nervous derivatives of the 3rd branchial arch?
|
CN IX (stylopharyngeus) swallow stylishly
|
|
|
What are the cartilaginous derivatives of the 4th-6th branchial arches?
|
Cartilage: thyroid, cricoid, arytenoids, corniculate, and cuneiform
|
|
|
What are the muscular derivatives of the 4th branchial arch?
|
- Most pharyngeal constrictors
- Cricothyroid - Levator veli palatini |
|
|
What are the muscular derivatives of the 6th branchial arch?
|
All intrinsic muscles of larynx except cricothyroid
|
|
|
What are the nervous derivatives of the 4th branchial arch?
|
CN X (superior laryngeal branch) = simply swallow
|
|
|
What are the nervous derivatives of the 6th branchial arch?
|
CN X (recurrent laryngeal branch) = speak
|
|
|
What are the implications of abnormalities of the derivatives of the 4th-6th branchial arch?
|
- Arches 3 and 4 form posterior 1/3 of tongue
- Arch 5 makes no major developmental contributions |
|
|
How do you remember the functions of the branchial arches?
|
When at the restaurant of the golden ARCHES, children tend to first CHEW (1), then SMILE (2), then SWALLOW STYLishly (3) or SIMPLY SWALLOW (4), and then SPEAK (6)
|
|
|
Which precursor structure provides cartilage, muscles, and nerves primarily aimed at chewing? What structures?
|
1st branchial arch
- Meckel cartilage (mandible, malleus, incus, spheno-mandibular ligament) - Muscles of mastication: temporalis, masseter, lateral and medial pterygoids), Mylohyoid, anterior belly of digastric, tensor tympani, tensor veli palatini - CN V2 and V3 |
|
|
Which precursor structure provides cartilage, muscles, and nerves primarily aimed at facial expression? What structures?
|
2nd Branchial Arch
- Reichert cartilage (stapes, styloid process, lesser horn of hyoid, stylohyoid ligament) - Muscles: stapedius, stylohyoid, platysma, belly of digastric - CN VII (facial nerve) |
|
|
Which precursor structure provides cartilage, muscles, and nerves primarily aimed at swallowing? What structures?
|
3rd Branchial Arch
- Cartilage: greater horn of hyoid - Stylopharyngeus (think of stylopharyngeus, innervated by glossopharyngeal nerve) - CN IX 4th Branchial Arch - Most pharyngeal constrictors, cricothyroid, levator veli palatini - CN X (superior laryngeal branch) |
|
|
Which precursor structure provides cartilage, muscles, and nerves primarily aimed at speaking? What structures?
|
6th Branchial Arch
- All intrinsic muscles of larynx except cricothyroid - CN X (recurrent laryngeal branch) |
|
|
Which precursor structure forms the posterior 1/3 of the tongue?
|
Branchial arches 3 and 4
|
|
|
What are the derivatives of the 1st branchial pouch?
|
- Develops into middle ear cavity, eustachian tube, mastoid air cells
- Contributes to endoderm-lined structures of ear |
|
|
What are the derivatives of the 2nd branchial pouch?
|
Develops into epithelial lining of palatine tonsil
|
|
|
What are the derivatives of the 3rd branchial pouch?
|
- Dorsal wings: develops into inferior parathyroids
- Ventral wings: develops into thymus Contributes to 3 structures: thymus, left and right inferior parathyroids *These structures end up below 4th pouch structures* |
|
|
What are the derivatives of the 4th branchial pouch?
|
- Dorsal wings: develops into superior parathyroids
*These structures end up above 3rd pouch structures* |
|
|
How do you remember the branchial pouch derivatives?
|
Ear, Tonsils, Bottom-to-Top
1 - ear 2 - tonsils 3 - dorsal (bottom = inferior parathyroids) 3- ventral (to = thymus) 4 - top = superior parathyroids |
|
|
What developmental precursor is abnormal in DiGeorge syndrome?
|
3rd and 4th pouches
|
|
|
What are the implications of DiGeorge Syndrome?
|
- Aberrant development of 3rd and 4th pouches
- T-cell deficiency (thymic aplasia) and hypocalcemia (failure of parathyroid development) - Associated with cardiac defects (conotruncal anomalies) |
|
|
What genetic abnormality is present in MEN 2A syndrome?
|
Mutation of germline RET (in neural crest cells)
|
|
|
What can MEN 2A syndrome lead to?
|
- Pheochromocytoma (adrenal medulla)
- Parathyroid tumor (3rd/4th pharyngeal pouch) - Medullary Thyroid Cancer (parafollicular cells) - derived from neural crest cells, associated with 4th/5th pharyngeal pouches |
|
|
Medullary thyroid cancer (parafollicular cells) are associated with what branchial precursor?
|
4th/5th pharyngeal pouches
|
|
|
Parathyroid tumors are associated with what branchial precursor?
|
3rd/4th pharyngeal pouch
|
|
|
What causes a cleft lip?
|

Failure of fusion of the maxillary and medial nasal processes (formation of 1° palate)
|
|
|
What causes a cleft palate?
|
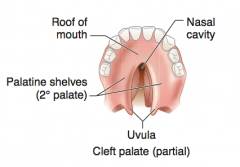
- Failure of fusion of the two lateral palatine processes
OR - Failure of fusion of lateral palatine processes with the nasal septum and/or median palatine process (formation of 2° palate) |
|
|
What is the result of a failure of fusion of the maxillary and medial nasal processes?
|

Cleft lip
|
|
|
What is the result of a failure of fusion of the two lateral palatine processes or failure of fusion of lateral palatine processes with the nasal septum and/or median palatine process?
|
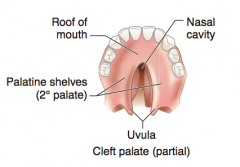
Cleft palate
|
|
|
What is the default genital development? What develops and when degenerates?
|
Female Genitals are Default:
- Mesonephric duct degenerates - Paramesonephric duct develops |
|
|
What is necessary for the default genital development to switch to male genital development?
|
SRY gene on Y chromosome: produces testis-determining factor (testes development)
|
|
|
What prevents development of the paramesonephric ducts in males?
|
Sertoli cells secrete Müllerian Inhibitory Factor (MIF)
|
|
|
What stimulates development of the mesonephric ducts in males?
|
Leydig cells secrete Androgens
|
|
|
What is the source of Müllerian Inhibiting Factor? Function?
|
- Secreted from Sertoli cells in males
- Suppresses development of paramesonephric ducts (female genitalia) |
|
|
What is the source of androgens during fetal development? Function?
|
- Secreted from Leydig cells in males
- Stimulates development of mesonephric ducts (male genitalia) |
|
|
What forms the female internal structures? What are these structures?
|
Paramesonephric (Müllerian) Duct
- Fallopian tubes - Uterus - Upper portion of vagina (lower portion from urogenital sinus) |
|
|
What can abnormalities of the Müllerian duct lead to?
|
Anatomical defects that may present as 1° amenorhea in females with fully developed 2° sexual characteristics (indicator of functional ovaries)
|
|
|
What forms the male internal structures? What are these structures?
|
Mesonephric (Wolffian) duct
- Seminal vesicles - Epididymis - Ejaculatory duct - Ductus deferens (SEED) |
|
|
What results from incomplete fusion of the paramesonephric ducts?
|
Bicornuate Uterus
|
|
|
What results from complete failure of fusion of the paramesonephric ducts?
|
Double uterus and vagina
|
|
|
What causes a Bicornuate uterus? Consequences?
|
Incomplete fusion of the paramesonephric ducts
- May lead to recurrent miscarriages |
|
|
What causes a double uterus and vagina?
|
Complete failure of fusion of the paramesonephric ducts
|
|
|
What are the implications of a patient with no sertoli cells or no Müllerian Inhibitory Factor?
|
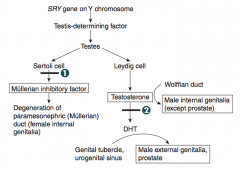
- Develops both male and female internal genitalia (because no MIF to prevent female internal organs from developing)
- Develops male external genitalia (due to Testosterone) |
|
|
What are the implications of a patient with a 5α-reductase deficiency?
|
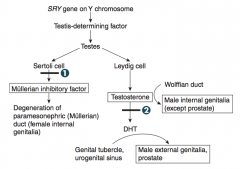
Inability to convert T → DHT
- Formation of male internal genitalia with ambiguous external genitalia until puberty - At puberty, testosterone levels increase causing masculinization |
|
|
What does the undifferentiated genital tubercle become when exposed to estrogen vs dihydrotestosterone?
|
- Estrogen → Glans Clitoris & Vestibular Bulbs
- DHT → Glans Penis & Corpus Cavernosum and Spongiosum |
|
|
What does the undifferentiated urogenital sinus become when exposed to estrogen vs dihydrotestosterone?
|
- Estrogen → Greater Vestibular Glands (of Bartholin) & Urethral and Paraurethral Glands (of Skene)
- DHT → Bulbourethral Glands (of Cowper) & Prostate Gland |
|
|
What does the undifferentiated urogenital folds become when exposed to estrogen vs dihydrotestosterone?
|
- Estrogen → Labia Minora
- DHT → Ventral shaft of Penis (Penile Urethra) |
|
|
What does the undifferentiated Labioscrotal Swelling become when exposed to estrogen vs dihydrotestosterone?
|
- Estrogen → Labia Majora
- DHT → Scrotum |
|
|
What are the types of congenital penile abnormalities? Which is more common?
|
- Hypospadias = more common
- Epispadias |
|
|
Which congenital penile abnormality on the underside of the penis?
|
Hypospadias (ventral side)
*Hypo is below* |
|
|
Which congenital penile abnormality on the superior of the penis?
|
Epispadias (dorsal side)
*When you have Epispadias, you hit your Eye when you pEE* |
|
|
What causes an abnormal opening of the penile urethra on the inferior (ventral) side of the penis?
|
Hypospadis = failure of the urethral folds to close
|
|
|
What causes an abnormal opening of the penile urethra on the superior (dorsal) side of the penis?
|
Epispadias = faulty positioning of the genital tubercle
|
|
|
Why do you need to fix hypospadias (abnormal opening of penile urethra on inferior side of penis)?
|
Prevent UTIs
|
|
|
What is associated with Epispadias?
|
Exstrophy of the bladder is associated with Epispadias
|
|
|
What anchors the testes within the scrotum?
|
Gubernaculum (band of fibrous tissue)
|
|
|
What forms the tunica vaginalis in males?
|
Processus vaginalis (evagination of peritoneum)
|
|
|
What forms the ovarian ligament and round ligament of the uterus?
|
Gubernaculum (band of fibrous tissue)
|
|
|
What is the remnant of the gubernaculum in males and females?
|
- Males: anchors testes within scrotum
- Females: ovarian ligament and round ligament of uterus |
|
|
What is the remnant of the processus vaginalis in males and females?
|
- Males: forms tunica vaginalis
- Females: obliterated |

