![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
22 Cards in this Set
- Front
- Back
|
describe development of the foetal testis
|
germ cells differentiate into spermatogonial stem cells peritubular myoid cells form (flattened smooth msucle like cells) around the tubules Leydig cells form in interstitium between tubules - this also contains blood vessles and lymph |
|
|
describe the mechanism of development of the foetal testis by SRY
|
2. sertoli cells form sex cords and then tubules 3. sertoli cells secrete DHH and PDGF-A to induce Leydig cell formation |
|
|
describe the Leydig cells
|
in mammals there are two different populations of Leydig cells - one foetal and one adult |
|

what does this shwo
|
1st image = foetal Leydig cells 2nd image = adult Leydig cells |
|
|
what additional function other than testosterone production do Leydig cells have
|
a combination of this and testosterone is essential for testis descent |
|
|
how does the Leydig cell mak testosterone |
LH binds to Leydig cell and causes ATP to form cAMP which induces fromaton of StAR protein StAR protein causes cholesterol to move into mitochondria cholesterl forms pregenelone which moves out into mitochondria and induces testosterone formation testosterone moves out into smooth ER and then leaves the Leydig cell |
|
|
what controls the action of Sertoli cells
|
|
|
|
what are the functions of Sertoli cells
|
- SRY acts to form SC - SC regulates development of other cell types 2. forms the blood testis barrier - tight junctions between SC 'seal off' the lumen of the tubule 3. secrete AMH - prevents paramesonephric duct development 4, in adult maintains the Leydig cells - mechanism unknown |
|
|
describe features of the peritubular myoid cell
|
androgen-dependant essential for normal spermatogenesis |
|
|
how is testis function controlled
|
also some input from ACTH, GH and thyroid hormones paracrine control also essential |
|
|
describe testes descent
|
2. INSL3 acts to complete shortening of the gubernaculum and movement of the testes into the scrotum |
|
|
summarise male devlopment
|
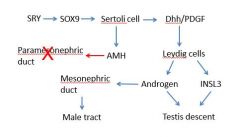
|
|
|
describe spermatogenesis
|
1. proliferation 2. meiosis 3. spermiogenesis - differentiation process |
|
|
describe the proliferation/spermatogonia stage of spermatogenesis
|
|
|
|
describe the meiosis stage of spermatogenesis
|
1. DNA replication starts 2. chromosomes line up 3. 1st meiotic division 4. 2nd meiotic division end up with a haploid round spermatid which goes on to enter spermiogenesis |
|
|
describe the spermiogenesis stage of spermatogenesis
|
begins with round spermatid 1. nuclear condensation 2. acrosome forms from golgi 3. tail develops from centriole 4. cytoplasm re-distributes - residual body lost 5. mitochondria re-arrange in middle piece final result is an elongated spermatid called a spermatozoa |
|
|
what is spermatogenesis controlled by
|
space and time |
|
|
describe hormonal control of spermatogenesis
|
Sertoli cells secrete FSH and testosterone which stimulates spermatogonial differentiation testosterone accts through the Sertoli cells and PTMC to ensure the passage through meiosis Testosterone stimulates spermiogenesis |
|
|
what is the function of the epididymis
|
to induce sperm maturation non-motile, non-fertile sperm enter at the head and then become fertile and motile as they travel down the epididymis tail acts as sperm storage area |
|
|
describe the histological structure of the epididymis
|
epithelium gets smaller towards tail androgen sensitive structure |
|
|
what is the function of the accessory glands
|
4 accessory glands: seminal vesicles prostate bulbourethral glands preputial glands all are exocrine glands may be essential for embryo development |
|
|
describe features of the seminal vesicles
|
lined with tall columnar secretory epithelium surrounded by fibro-muscular capsule |

