![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
19 Cards in this Set
- Front
- Back
|
Methemoglobinemia
|
Hemoglobin oxidized to methemoglobin (ferrous iron -> ferric iron); ferric hemes are UNABLE to bind oxygen
Oxidation of one of the hemes in the Hb tetramer INCREASES the affinity for the remaining hemes in the tetramer |
|
|
Effects of methemoglobinemia on the oxygen dissociation curve
|
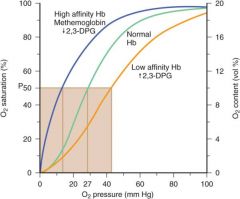
|
|
|
Cytochrome B5 Redutcase Deficiency (NADH-Methemoglobin Reductase Deficiency)
|
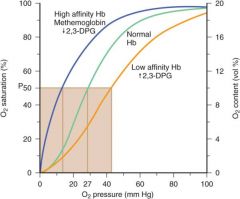
Functional deficiency of RBCs only
MetHb concentrations 10-35%; cyanotic but asymptomatic Heterozygotes at increased risk for acquired methemoglobinemia |
|
|
When do levels of MetHb become life threatening?
|
>50%
|
|
|
Main drugs that can cause acquired methemoglobinemia
|
Dapsone
Benzocaine and related topical anesthetics |
|
|
How to tx acquired methemoglobinemia?
|

|
|
|
Bright red molecule
|
Carboxhemoglobin; shifts ODC left
|
|
|
Brown molecule
|
Methemoglobin; shifts ODC left
|
|
|
Blue molecule
|
Deoxyhemoglobin; shifts ODC right
|
|
|
Methylene Blue
|
Used to tx increased MetHb levels; decreases the levels and shifts ODC to the right
|
|
|
Sulfhemoglobinemia
|
Sulfur binds to the B-prrole ring of the moiety; can't bind oxygen and has a green color; does not respond to methylene blue tx
|
|
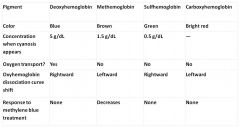

|
Summary Slide
|
|
|
How does MetHb vs SulfHb affect the oxygen dissociation curve?
|
Sulfhemoglobinemia considered w a cyanotic/gray pt who has normal oxygen tension, and has failed to respond to methylene blue therapy; usually asymptomatic unless other globinemias presnt
pts have a GRAY appearance |
|
|
How does MetHb vs SulfHb affect the oxygen dissociation curve?
|
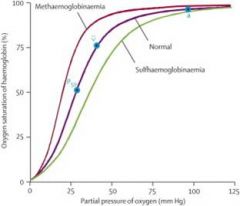
Sulfhemoglobinemia considered w a cyanotic/gray pt who has normal oxygen tension, and has failed to respond to methylene blue therapy; usually asymptomatic unless other globinemias presnt
pts have a GRAY appearance |
|
|
How does methylene blue work as a tx for methemoglobinemia?
|
Methylene blue functions as an artificial electron acceptor for NADPH methemoglobin reductase; NADPH generated via hexose monophosphate shunt
|
|
|
What is the problem in HbM disease?
|
the HbM is not amenable to reduction to ferrous states despite intact enzyme systems; acquired congenital methemoglobinemia
|
|
|
How can G6PD deficiency cause methemoglobinemia?
|
There is impaired production of the cofactor NADPH, required for the reduction of methemoglobinemia
|
|
|
Why might pyruvate kinase deficiency cause methoglobinemia?
|
Impaired production of NADH, essential cofactor for diaphorase I
|
|
|
cytochrome-b5 reductase
|
Same as NADH methemoglobin reductase; reduces via electron donation the spontaneous formation of methemoglobin; disruption of this enzyme may lead to methemoglobineima
|

