![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
79 Cards in this Set
- Front
- Back
|
what are the stages and guidelines for excisions of tumors?
|
Guidelines of Excision
Stage 1 (Benign, latent) Intracapsular Excision Marginal Local Excision Diagnosis must be certain Guidelines of Excision Stage 2 (Benign, Active) Marginal Local Excision Careful Dissection 30% recurrence with intracapsular excision Guidelines of Excision Stage 3 (Benign, Aggressive) Wide local Excision Extracapsular satellite lesions 50% recurrence with marginal excision Guidelines of Excision Stage 1A (Malignant, Low-Grade, Intracompartmental) Wide Marginal Resection Low recurrence rate Stage 1B (Malignant, Low-Grade, Extracompartmental) Recurrence increased Guidelines of Excision Stage IIA & IIB (Malignant, high-grade, Intra/Extracompartmental) Radical Margin Excision |
|
|
Benign lesion
Younger individuals Well circumscribed Thin walled, amber fluid filled Freely movable May impinge on anatomic neighbors Excision, high recurrence rate |
Ganglion cyst
(Attachment: Extensor Tendon Joint Capsule) |
|
|
Most common plantar foot lesion
|
Plantar fibroma
|
|
|
20 – 40 y/o
10 – 15% Bilateral Plantar Zig-Zag incision High recurrence Pain with compression and weight bearing |
Plantar fibroma
|
|
|
Most common soft tissue tumor
|
Lipoma
|
|
|
Active, benign Stage 2 lesions
Peripheral nerve spindle cell origin |
Neurofibroma
|
|
|
Benign
Arising from peripheral nerve sheath Fusiform, well-encapsulated nodule |
Neurolemoma
(Discrete, often tender nodule Neurogenic pain and paresthesias Slow growth Seldom >2cm in diameter Stage 2, Active : Stage 1, latent Marginal local excision) |
|
|
Benign tumors of blood vessels
Childhood or early adolescence Skin and subcutaneous tissues More common Painless mass Bluish color Soft, easily compressable Deep fascia and muscle Rare Intermittent pain *Blanchable w compression PAINLESS |
Capillary Hemangioma (most common form)
(vs Cavernous hemangioma) |
|
|
Large, dilated, tourtuous endothelial cavities
Appear bluish PAINFUL *Do not blanch with compression |
Cavernous Hemangioma
(vs capillary hemangioma) |
|
|
Benign
Aggressive, proliferative lesion of synoval membranes Microscopical eval Fibroblast Giant cells |
Pigmented Villonodular Synovitis
(3 types: Extraarticular tenosynovial giant cell tumor Solitary intraarticular nodules Diffuse, villous, pigmented involving synovial membrane of joint) |
|
|
Painful
Swelling and limitation of joint motion Joint aspirate Serosanguinous brownish fluid Underlying osseous changes on x-ray |
Pigmented Villonodular Synovitis
|
|
|
Benign
Smooth muscle layer of blood cell origin Female:male, 2:1 Solitary, encapsulated Freely moveable Recurrence is low |
Angioleiomyoma
"Angio is low (recurrence)" |
|
|
Which tumor?
Common on plantar foot keratin is produced Forms mass **“cheesy material” Sinus tract may develop Painful |
Epidermal inclusion cyst
(caused from traumatic introduction of epidermal cells into the subepidermal layer) |
|
|
Most common malignant ST tumor?
|
Malignant Fibrous Histiocytoma
(Most common malignant ST tumor 5 subtypes: Pleomorphic Myxoid Giant cell Inflammatory Angiomatoid) "FIbrous has FIve subtypes: i AM PIG" |
|
|
50-70 y/o
Angiomatoid – adolescence Males > females Pain, fever,chills, and myalgia Located below the deep fascia 5 year survival 73% when lesion located distal to the knee (28% proximal) |
Malignant Fibrous Histiocytoma
|
|
|
70% in the lower extremity
< 50% occur close to a joint Fewer in direct continuity with joint synovium Slow growing High-rage lesion Minimal exposure biopsy Radical resection or amputation is required |
Synovial sarcoma
|
|
|
Malignant tumor
Rare in foot and ankle Arises from deep fascia Men > 40y/o Symes amputation with distal small lesions Otherwise BKA is reccommended |
Fibrosarcoma
|
|
|
Malignant
40 to 60 y/o Male > females Nonencapsulated, invasive growth *Metastasis is common Staged differentiation Radical excision or amputation |
Liposarcoma
|
|
|
Which implant is put in by cutting a window in the tibia?
|
Buechel pappas
|
|
|
Which implant has a dual fin talar fixation?
|
Buechel pappas
|
|
|
What is the only implant you can do with AVN?
|
Buechel pappas
|
|
|
Which implant fuses the tibia and fibular and has a definitive amputation rate?
|
Alvin agility
|
|
|
your choices are Alvin agility and STAR implant:
which is mobile bearing and which is rigid/fixed? |
Alvin agility is rigid/fixed.
STAR is mobile bearing |
|
|
Which implant has a rounded talor component so that it moves 360 degrees?
|
Ramses
"Ramses is Round" |
|
|
Only implant that goes into lateral side?
|
ESKA implant
"Esculate---->ESKA-LATe" |
|
|
Which 2 popular implants can NOT be used for talar necrosis?
|
STAR and ALvin
“AVasculAR necrosis---can’t use AlVin and stAR” |
|
|
Which implant:
Cobalt-Chromium Alloy double stem tibial component Ultra-High Molecular Weight Polyethylene meniscus Hydroxyapatite tibial-talar coating |
STAR
|
|
|
Which implant:
Titanium alloy single stem tibial prosthesis Ultracoat Titanium Nitride beaded coating Dual fin talar fixation Meniscus of Ultra-High Molecular Weight Polyethylene |
Buechel-Pappas
|
|
|
Which implant uses a sulcus burr for the talar sulcus step?
|
Buechel-pappas
|
|
|
How many current total ankle joint prostheses are in use around the world?
|
11
(from Feldman article) Agility (DuPuy, Warsaw, IN) Scandinavian Total Ankle Replacement (Waldmar Link, Hamburg, Germany) Buechel-Pappas (Endotec, Orange, NJ) Salto (Tornier SA, Lyon, France) Alpha OSG (Alphanorm, Quiershied, Germany) Ankle Evolutive System (AES) (Biomet Merck France Sarl (French Corporation), Valence, France) ESKA (ESKA, Lubeck, Germany) Albatros, (Groupe Lepine, Lyon, France) Hintegra (Newdeal SA, Lyon, France) Ramses (Fournitures Hospitalie`res Industrie, Quimper, France) TNK ceramic ankle prosthesis (Dr. Yoshino Takakura, Nara, Japan). |
|
|
Which implant is the only total titanium and titanium nitride implant?
|
Buechel Pappas
|
|
|
Which implant:
"It is the only one that requires excision of 40% to 50% of the width of both malleoli, excision and fusion of the tibio-fibular syndesmosis, and fixation of the fibula/ tibia with transcortical screws. It requires the excision of more dome of the talus than any other prosthesis. It is the most difficult of the seven ankles the author has experience with to implant and is the only one requiring that an external ankle joint distractor be used for the procedure." |
Agility
|
|
|
Which implant?
"The implant is classified by the FDA as a class II prosthesis, thus allowing it to be the only FDA-approved ankle implant in the United States at this time." |
Agility
|
|
|
Which implant?
"...is the only design with a separate specific talar avascular necrosis (AVN) component, called the THICK talus." |
Buechel Pappas
|
|
|
According to Feldman article: "Who are the patients for whom TAA offers an advantage
over fusion?" |
"The brief answer is the middle aged or elderly
patient with an anatomically aligned ankle and heel, whose ankle has a well-preserved range of movement that includes at least 5 degrees of dorsiflexion." |
|
|
True of false:
Mitchell introduced term “phantom limb” & he describes what we call CRPS today Dekatas first used the term “reflex sympathetic dystrophy” |
True
(from handout) |
|
|
Best diagnostic test for CRPS?
|
Bone scan
(Bone scan uptake in areas beyond initial trauma) |
|
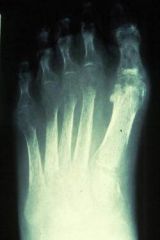
Whats going on here and what is it indicative of?
|
The bone appears mottled “ = describing punched out lesions due to periarticular remodeling seen in CRPS---->SUDECKS ATROPHY!
|
|
|
Describe the clinical phases of CRPS (one word description for each phase)
|
Phase IA=Vasoconstriction (2-6 WEEKS)
Phase IB=Vasodilatation (2-6 MONTHS) Phase II=Osteoporosis (6-12 MONTHS) Phase III=Vasoconstriction |
|
|
Which phase of CRPS do you see sudeck's atrophy as the hallmark sign?
|
Phase II
"SUe is TWO" |
|
|
Which phase of CRPS do you see cyanotic nail beds?
|
Phase IA
|
|
|
Which phase of CRPS do you see "doughy edema"?
|
Phase IB
|
|
|
Which phase of CRPS do you see morbid, constricted muscle atrophy?
|
Phase III
|
|
|
Dose of oral steroids for CRPS at:
week 1? week 2? week 3? week 4? week 5? |
week 1=40-60mg/day
2=30-50mg 3=20-40mg 4=10-30mg 5=0-10mg |
|
|
what is the technique called that uses an epidermal block for CRPS?
|
Raj technique
|
|
|
why would one use a "sham block" in CRPS?
|
it is an injection of normal saline to rule out malingering
|
|
|
what is the average number of sympathetic blocks used in treatment of CRPS? what is the success rate?
|
3-4
80% |
|
|
which 2 treatments for CRPS are vasodilators and used for HTN as well?
|
Reserpine and guanethidine monosulfate (Ismelin)
|
|
|
which treatment for CRPS is used for ventricular fibrillations as well?
|
bretylium tosylate (Bretylol, Darenthin)
|
|
|
which treatment for CRPS is a tricyclic antidepressant?
|
Elavil (amitriptyline)
(50-75mg hs or divided, max daily dose 150mg) "Elavates your mood" |
|
|
Which treatment for CRPS is used for pheochromocytoma to control episodes of HTN and sweating?
|
Phenoxybenzamine HCL (Dibenzyline)
"PHENO for PHEO" |
|
|
Which treatment for CRPS is used for persistant pulmonary HTN of the newborn
|
Tolazoline HCL (Priscoline)
|
|
|
True of false:
Methodone and Nyquil are good for pain control for CRPS |
True
|
|
|
In terms of external fixation and bone marrow lesion prognosis, if the two shafts of bone overlap competely, how many days prognosis?
|
21-30 days
|
|
|
In terms of external fixation and bone marrow lesion prognosis, if the center of the midshaft are seperated by more than half but still some medullary canal closer to next, how many days prognosis?
|
41-50 days
|
|
|
In terms of external fixation and bone marrow lesion prognosis, if the center of the midshaft is seperated by less than half but not completely overlapping, how many days prognosis?
|
31-40 days
|
|
|
In terms of external fixation and bone marrow lesion prognosis, if the two shafts of bone are completely seperated and not touching, how many days prognosis?
|
51-70 days
|
|
|
In terms of the mechanism of injury requiring an external fixator, if you have direct trauma, a 5cm or less open lesion, or a large smash /degloving injury.......then you add an additional __?__ weeks per mechanism to the marrow prognosis.
|
2
|
|
|
External fixation:
With distal traction joints and the ligamentous attachments are stretched. Safe time is ______ hours with _____kg traction. Joints affected if stretched longer. Most efficient to distract immediately adjacent to the fracture site. This may be adjacent bone if spanning joint. |
With distal traction joints and the ligamentous attachments are stretched. Safe time is <2-3 hours with ~6 kg traction. Joints affected if stretched longer. Most efficient to distract immediately adjacent to the fracture site. This may be adjacent bone if spanning joint.
|
|
|
When external fixation is placed, when does patient start PT with partial weightbaring?
When do they start FWB or with a cane? |
the next day
one month (walking is impt because the muscles pull fracture into compression) |
|
|
External fixation:
When you get purulent drainage, on day one treat infection with ABX and cleaning!! Daily with antiseptic. In _______ days if still pus, pull the wire and I&D sight with lavage and IM ABX best, PO ok. If this occurs later in treatment you may not need to reapply wires, but if you need to reapply then reinsert in 4-5days. |
When you get purulent drainage, on day one treat infection with ABX and cleaning!! Daily with antiseptic. In 2-3 days if still pus, pull the wire and I&D sight with lavage and IM ABX best, PO ok.
If this occurs later in treatment you may not need to reapply wires, but if you need to reapply then reinsert in 4-5days. If wire is painful for several days post op, reposition on the ring. Possible nerve irritation. |
|
|
True/False?
External fixation: If wire is painful for several days post op, the wire needs to be taken out. |
FALSE
If wire is painful for several days post op, reposition on the ring. Possible nerve irritation. |
|
|
There are 4 types of pseudoarthrosis described, which one describes the following:
the fragment ends are atrophic, sharpen end, periosteal layers are absent, and marrow canal is dysfunctional (poor vascular supply). 20 deg motion. Unable to lengthen through closed technique due to poor regenerate potential. |
hypoplastic
|
|
|
There are 4 types of pseudoarthrosis described, which one describes the following:
ends are more congruent, mild-mod osteoporosis, sclerotic ends, good vascular status.10-15 deg mobility |
Normoplastic
|
|
|
There are 4 types of pseudoarthrosis described, which one describes the following:
fragment ends are thickened (bamboo-like), marked collateral circulation. 5-7 deg mobility |
Hyperplastic
|
|
|
There are 4 types of pseudoarthrosis described, which one describes the following:
fragment ends are smooth, ball and socket like, capsule, canal is closed with bone (with large defect), hypervascular soft tissue. |
Nearthrosis
|
|
|
External fixation powerpoint:
1) How many mm per day can lengthen bone? 2) What dye is used in resecting bone for osteomyelitis? |
1) 0.75mm/day
2) Methyl blue (i think he meant to say methylene blue) |
|
|
According to the student presentation, which implant was the first to be approved by the FDA?
The ankle joint is classified as what kind of joint? |
Agility
Hinge joint (-from treu dang and fadi presentation) |
|
|
According to the student presentation for external fixation, what was the only pre req listed in the study?
How long was the cast left on? how long was frame left on? |
Adequate blood supply
Cast left on for 3 months, frame for 4 months 8% bka, 8% had chronic vascular I dont know what any of this really means but its what i have for Azukes presentation. |
|
|
according to student presentation, for the stable tibial component how many rods, how many rings, and how many wires are used?
|
2 rings, 2 rods, 4-6 wires: stable tibial component.
??? |
|
|
True or false:
Although everyone is taught to take a thorough history and physical before the clinical examination, in the context of soft tissue masses this information is commonly not helpful in the differentiation or categorization of the mass. Similarly, the epidemiological information such as age, sex, and race among others is of little concrete use. |
True
|
|
|
What is probably the most important diagnostic tool for characterization and gross classification of the soft tissue mass?
|
Physical examination
|
|
|
The most specific and sensitive study for imaging soft tissue masses is __________.
|
MRI
|
|
|
What is the primary goal of a biopsy of a tumor/lesion?
|
Diagnosis
|
|
|
True or false:
When planning an incisional biopsy, it is most important to orient the incision in a transverse fashion or in other words, perpendicular to the muscle beneath it. |
FALSE
When planning an incisional biopsy, it is most important to orient the incision in a longitudinal fashion or in other words, parallel to the muscle beneath it. In case the lesion is malignant, the longitudinal incisional scar can easily be excised at the next operation. Yet if erroneously fashioned or transversely fashioned, the incision tract will acquire a much wider excision that may compromise closure |
|
|
**Student presentation on CRPS:
In a patient with positive “Kick-Off” position, when the patient’s leg has been pushed down from its initial extended position and then the patient is distracted, the leg will ________________________________________. |
Involuntarily return to the initial extended position
|
|
|
According to student presentation on CRPS:
1) What nerve is by far the most common nerve involved in CRPS type 2 2) How long after injury should u start to consider a DX of CRPS? 3) How long do u expect patient to have pain after bunion SX? |
1) Superficial peroneal nerve
2) Atleast 3 months 3) 4 months |
|
|
Random important info on earlier student presentations:
-Trisas presentation on charcot. What goal of the surgery was prob obtained but not really studied in this paper? Goal Was to redistribute weight on bottom of foot to prevent future ulceration so want to know foot shape & if they got subsequent ulcers -26% pin tract infection rate in study. -The limb salvage rate of the diabetic Charcot foot and ankle deformities in this study was 96%. *Acute phase of charcot foot is about 2 WEEKS *Coalescence phase is about 2 MONTHS *Remodeling phase is about 2 YEARS -Ring fixator-gonna leave on 10-12 weeks and according to this article, 1 of those 4 pins get infected! -Average external fixator has 10 wires. *12 wires 12 weeks! If you see one of these frames think of it as each wire last a week. 3 in FF 3 in RF and 3 in each tibial ring. -Cliffs presentation. 81% recurrence rate after 2 years. FDB flap for calcaneous |
none
|
|
|
What is the most common ST malignancy of the FOOT?
|
Synovial sarcoma
|

