![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
55 Cards in this Set
- Front
- Back
|
|
|
|
|
|
|
|
|
cells that have a wrinkly-raisin nucleus |
|
|
|
can you have hpv infected uterus? |
no, only vulva, vagina, cervix |
|
|
can condyloma progress to carcinoma? |
ye |
|
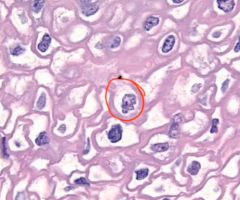
|
koilocyte, hpv infected |
|
|
Is there increased risk for squamous cell carcinoma with lichen sclerosis? |
yes, a little |
|
|
Is there increased risk for squamous cell carcinoma with lichen simplex chronicum? |
no |
|
|
thinning of the epidermis and fibrosis (sclerosis) of the dermis |
LICHEN SCLEROSIS |
|
|
hyperplasia of the vulvar squamous epithelium |
LICHEN SIMPLEX CHRONICUS |
|
|
Ddx for vulvar leukoplakia |
LICHEN SCLEROSIS LICHEN SIMPLEX CHRONICUS
VULVAR CARCINOMA |
|
|
VULVAR CARCINOMA Etiology |
1. HPV related (patient 40-50 yo) 2 non-HPV related - lichen sclerosis (pt 70 yo) |
|
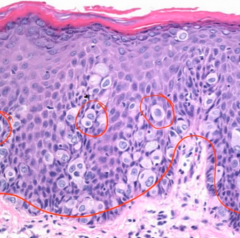
|
paget disease of vulva with malignant epithelial cells in the epidermis |
|
|
DiffDx for paget's disease of vulva and stains |
carcinoma - Paget cells: PAS+(mucus), keratin+ (intermediate filament in epithelial cells) melanoma - S100+ |
|
|
cancer cell vulva S100+ |
melanoma |
|
|
vulvar neoplastic cells: keratin+, PAS+ |
paget's disease |
|
|
vulvar neoplastic cells: S100+ |
melanoma |
|
|
does paget's disease in vulva mean underlying carcinoma? |
|
|
|
Mucosa of vagina is lined by _____ epithelium |
non-keratinizing stratified squamous epithelium |
|
|
where in the vagina are the cells derived from the urogenital sinus? |
lower 1/3 - stratified squamous;
- grow upward to replace the columnar epithelium lining of the upper 2/3 of the vagina (derived from the Miillerian ducts).
|
|
|
Increased incidence of adenosis in females |
who were exposed to diethylstilbestrol (DES) in utero |
|
|
why is adenosis important? |
can lead to clear cell adenocarcinoma |
|
|
adenosis |
Focal persistence of columnar epithelium in the upper 2/3 of the vagina |
|
|
Adenosis - Focal persistence of columnar epithelium in the upper 1/3 of the vagina |
|
|
Rare, but feared, complication of DES-associated vaginal adenosis |
CLEAR CELL ADENOCARCINOMA |
|
|
complications of exposure to DES in utero |
1. Adenosis --> CLEAR CELL ADENOCARCINOMA 2. improper smooth muscle formation in GU canal --> ectopic pregnancies, other complications |
|
|
malignant mesenchymal proliferation |
sarcoma |
|
|
vaginal or penis malignancy of a child (usually < 5 yrs of age) |
EMBRYONAL RHABDOMYOSARCOMA |
|
|
EMBRYONAL RHABDOMYOSARCOMA age population |
children <5yo |
|
|
grape-1 ike mass protruding from the vagina or penis |
EMBRYONAL RHABDOMYOSARCOMA |
|
|
EMBRYONAL RHABDOMYOSARCOMA |
Malignant mesenchymal proliferation of immature skeletal muscle; rare |
|
|
what kind of cells is EMBRYONAL RHABDOMYOSARCOMA made of? |
Rhabdomyoblasts, the characteristic cell, exhibits cytoplasmic cross-striations (like an immature muscle cell would) and positive immunohistochemical staining for desmin and myogenin. |
|
|
tumor positive immunohistochemical staining for desmin and myogenin. |
EMBRYONAL RHABDOMYOSARCOMA desmin - muscle cell myogenin - nuclear transcription factor that would be present in immature muscle cells |
|
|
When spread to regional lymph nodes occurs, cancer from the lower 1/3 ofvagina goes to, |
inguinal nodes |
|
|
When spread to regional lymph nodes occurs, cancer from the upper 2/3 goes to |
regional iliac nodes |
|
|
Exocervix is lined by , |
nonkeratinizing squamous epithelium |
|
|
Endocervix is lined by |
a single layer of columnar cells. |
|
|
can you get condyloma in the cervix? |
yes, HPV infection can affect vulva, vagina, cervix |
|
|
where does HPV like to especially invade? |
|
|
|
if you get infected with HPV, what are the chances that it will be a persistent infection? |
10%
(90% of infection are cleared by the immune system and have no risk of going to CIN) |
|
|
which genes in HPV make them more likely to cause CIN? |
E6 and E7 proteins which result in increased destruction of p53 and Rb, respectively
E6 - p53 E7 - Rb
(normally, if there is too much damage to the cell, p53 calls in Bax, which deactivates bcl2; without bcl2, the mitochondrial membrane no longer stable --> releases cytC, which activates apoptosis. Stops G1->S phase
Rb: Rb holds E2F, which is needed for progression through cell cycle. Need to phosphorylate Rb before it will release E2F. If no Rb, E2F freely available, helps cell move through cell cycle) |
|
|
is CIN neoplasia ? |
no, it's dysplasia |
|
|
what's the difference between CIN I and carcinoma in situ of cervix? |
CIN I-III could potentially reverse (because it's a dysplasia) Carcinoma in situ (CIS) will not reverse
CIN I - 66% potential to reverse CIN II - 33% potential to reverse |
|
|
next step after CIS |
cervical carcinoma (it's invasive) |
|
|
cervical carcinoma presents as |
Presents as vaginal bleeding, especially postcoital bleeding, or cervical discharge |
|
|
is CIN an AIDS defining illness? |
no, but cervical carcinoma is |
|
|
what kinds of cervical carcinoma can you get? |
squamous cell carcinoma (exocervix) adenocarcinoma (endocervix) |
|
|
what causes cervical carcinoma? |
squamous cell carcinoma (exocervix) and adenocarcinoma (endocervix)) |
|
|
what causes adenocarcinoma of the cervix? |
hpv |
|
|
what causes squamous cell carcinoma of the cervix? |
hpv |
|
|
late finding in advanced cervical carcinoma (both squamous and adeno) |
Hydronephrosis
Advanced tumors often invade through the anterior uterine wall into the bladder, blocking the ureters. Hydronephrosis with postrenal failure is a common cause of death in advanced cervical carcinoma
|
|
|
ostrenal failure is a common cause of death in ______ cancer |
advanced cervical carcinoma. |
|
|
Is Pap smear better at detecting squamous cell carcinoma or adenocarcinoma? |
limited efficacy in screening for adenocarcinoma
The risk of adenocarcinoma has not decreased significantly due to this screening test
Pap smear is good for squamous cell carcinoma rather than adenocarcinoma |
|
|
which strains does the hpv vaccine currently cover? |
|
|
|
how long does the hpv vaccine protection last? |
5 yrs |

