![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
80 Cards in this Set
- Front
- Back
|
Kallman gene(s) and inheritance pattern(s) |
KAL1 (XL) FGFR1 (AD) |
|
|
Mutations in AR gene cause _____ |
Androgen insensitivity syndrome |
|
|
Collagen 4 defect. Name syndrome |
Alport |
|
|
Predominant Hb on electrophoresis is Hb F |
Beta thal major |
|
|
Severe motor delay and hypotonia, microcephaly |
Canavan disease |
|
|
Cobblestone lissencephaly. Name syndrome |
Congenital muscular dystrophy - Walker Warburg |
|
|
Congenital progressive hypotonia + contractures. Name syndrome and inheritance pattern |
Congenital muscular dystrophy. AR |
|
|
Which triplet is repeated in myotonic dystrophy 1? |
CTG |
|
|
What is the most common terminal deletion syndrome |
Monosomy 1p36 |
|
|
GLI3 gene syndrome(s) and inheritance pattern(s) |
Pallister-Hall and Greig cephalopolysyndactyly, AD |
|
|
Acute intermittent porphyria inheritance pattern and gene |
AD, HMBS |
|
|
CADASIL gene |
NOTCH3 |
|
|
Which gene causes hypopigmention in Angelman syndrome |
OCA2 |
|
|
Hypohydrotic ectodermal dysplasia inheritance pattern and main gene |
XL; EDA |
|
|
What does VACTERL stand for? How many features are needed to meet diagnostic criteria? |
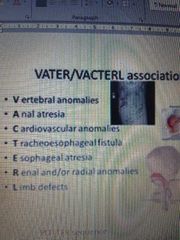
At least 3 features needed |
|
|
Syndrome with characteristic maladaptive behaviours. I.e., self harm |
Smith Magenis |
|
|
RAI1 mutation Name syndrome |
Smith magenis |
|
|
17p11.2 deletion. Name syndrome |
Smith Magenis |
|
|
CREBBP gene. Name syndrome |
Rubinstein Taybi |
|
|
What does CHARGE stand for? |
Coloboma, heart defect, atresia choanae, growth and mental retardation, genitourinary malformations, ear anomalies/deafness |
|
|
EYA1 gene. Name syndrome |
Branchio oto renal syndrome |
|
|
Branchio oto renal syndrome gene and inheritance pattern |
EYA1, AD |
|
|
What are the primary features of Bardet Biedl? |
Rod cone dystrophy, polydactyly, truncal obesity, LD, male hypogonadism, female genital abnormalities, renal anomalies |
|
|
Craniosynostosis and ambiguous genitalia. Name condition and inheritance pattern |
Antley bixler, AR |
|
|
Maternal virilization during pregnancy. Name condition in fetus |
Antley bixler |
|
|
Shawl scrotum. Name condition and inheritance pattern |
Aarskog, XL |
|
|
Stimulus induced drop attacks. Name condition |
Coffin Lowry |
|
|
DD, dysmorphic, fleshy hands with tapered fingers. Name condition |
Coffin Lowry |
|
|
RPS6KA3 gene. Name condition |
Coffin Lowry |
|
|
Name syndrome(s). PTPN11 gene |
Noonan and LEOPARD |
|
|
Alagille genes and inheritance pattern |
JAG1 NOTCH2, AD |
|
|
Butterfly vertebrae. Name condition |
Alagille |
|
|
Posterior embryotoxon. Name condition |
Alagille |
|
|
Albinism and bleeding problems. Name condition and inheritance pattern |
Hermansky pudlak, AR |
|
|
Inheritance pattern of diastrophic dysplasia |
AR |
|
|
Waardenburg syndrome is associated with an increased risk of which birth defect |
NTD |
|
|
Usher syndrome inheritance pattern |
AR |
|
|
MYO7A gene. Name condition and inheritance pattern |
Usher syndrome; AR |
|
|
Gene and inheritance pattern for Hutchinson gilford progeria |
AD, LMNA |
|
|
Which conditions have defective nucleotide excision repair? |
XP, Cockayne |
|
|
ERCC6 gene. Name condition |
Cockayne |
|
|
Name 2 disorders of premature aging. What are the inheritance patterns? |
Cockayne (AR) and progeria (AD) |
|
|
GNAS gene. Name condition |
McCune Albright |
|
|
Blueberry muffin baby. Name teratogen and trimester of exposure |
Rubella; first (8 to 10 weeks) |
|
|
Name a teratogenic exposure that decreases birth weight and one that increases birth weight. |
Cigarettes decreases, maternal diabetes increases |
|
|
Which teratogenic exposure mimics FASD? |
Toluene |
|
|
What is the critical period for thalidomide exposure? |
2 to 5 weeks GA. Aka 34 to 50 days post LMP |
|
|
Developmental regression, RP, hypotonia, seizures, ataxia, childhood onset. Name conditions. |
Leigh syndrome and NARP |
|
|
Name main gene and inheritance pattern for Cornelia de Lange |
NIPBL, AD |
|
|
Name main gene and inheritance pattern for kabuki |
MLL2 |
|
|
Short stature, CHD, bleeding diathesis. Name condition |
Noonan |
|
|
Gene that can cause waardenburg type 1, 2 and 3 |
PAX3 |
|
|
Craniosynostosis with mitten type syndactyly. Name condition and gene |
Apert; FGFR2 |
|
|
What is the chance of fetal infection if mother has CMV? what percentage of infected babies are symptomatic |
25%; 1-3% |
|
|
What are the main anomalies seen in fetal CMV infection? |
Growth restriction, ocular abnormalities, organ enlargement, cerebral calcifications, heart defects (GOOCH) |
|
|
Which feature are associated with fetal rubella infection. |
Skin, heart, ears, eyes, rubella (SHEER) |
|
|
Which dose of radiation is potentially teratogenic? |
> 5 rads |
|
|
What are the main teratogenic effects of maternal diabetes |
Heart defect, NTD, macrosomia (HNM) |
|
|
What are the main teratogenic effects of elevated maternal phenylalanine? |
Heart defect, ID/IUGR, microcephaly |
|
|
Blueberry muffin baby. Name teratogenic exposure. |
Rubella |
|
|
Name main teratogenic effects of warfarin. |
Limb hypoplasia, epiphyses stippled, respiratory distress due to nasal hypoplasia (LERN) |
|
|
Name main teratogenic effects of retinoid exposure. |
Brain, ears, heart, thymus (BETH) |
|
|
What is chance of having an affected baby if the mother used retinoids during the first trimester? |
30% |
|
|
Name teratogenic effects of ace inhibitor exposure |
Hypocalvaria, IUGR, Potter's sequence (HIP) |
|
|
What is the critical period for ACE inhibitor exposure? |
2nd to 3rd trimester (HIP problems later in life means later in pregnancy) |
|
|
Name gene for thanatophoric dysplasia, inheritance pattern and recurrence risk. |
FGFR3, AD, theoretical germline mosaicism |
|
|
Name 3 prenatal features of thanatophoric dysplasia |
Short long bones, IUGR, polyhydramnios, bowed femurs, cloverleaf skull, macrocephaly |
|
|
Craniosynostosis with 2 3 digit syndactyly of the hand. Name condition and gene |
Saethre-Chotzen, TWIST1 |
|
|
Craniosynostosis with mitten hand syndactyly. Name condition and gene |
Apert; FGFR2 |
|
|
What is the best way to establish a diagnosis for DMD or BMD? |
Molecular testing (del dup detects 75%, sequencing detects 25%) |
|
|
Describe the managment for homocystinuria |
Low protein diet, B6, B12 and betaine therapy |
|
|
For which ethnicities should hemoglobin electrophoresis be performed prior to pregnancy |
African, Mediterranean, middle eastern, south east asian, west indian |
|
|
Woman with PKU should maintain what levels of phenylalanine during pregnancy? |
6 mg/dL or less |
|
|
What is chance of microcephaly for fetus of mother with poorly controlled PKU? |
75% |
|
|
What is chance of DD for fetus of mother with poorly controlled PKU? |
90% |
|
|
What is chance of CHD for fetus of mother with poorly controlled PKU? |
10% |
|
|
What is the carrier frequency of PKU? |
1/60 |
|
|
Under which circumstances does ASHG strongly recommend that research participants be recontacted? |
Updated results available which could impact medical management and research has appropriate resources to recontact |
|
|
Tf. Recontacting a research participant with updated results is not advised of the update is not expected to impact medical management. |
F. It is still advised but not as strongly |
|
|
Does ASHG support NIPT for sex chromosome abnormalities? For microdeletions? |
No, no |

