![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
50 Cards in this Set
- Front
- Back
|
Pediatric complications of gastroenteritis |
Hypoglycemia Metabolic acidosis Electrolyte abnormalities Dehydration Shock |
|
|
Risk factors for infectious diarrhea |
Premature Infants younger than 3 months Immunosupressed Malnourished Recent Abx Use Recent hospitalization Travel to developing country |
|
|
Causes of Vomiting in Pediatric Patients |
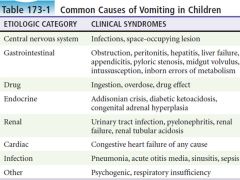

|
|
|
Causes of Diarrhea in Pediatric Patients |

|
|
|
Secretory Diarrhea - Pathophysiology - Features - Example pathogens |
Toxin cause increased intestinal secretion of electrolytes and bicarbonate
No reduction in stool volume with fasting, pH > 6, no reducing substances in stool
Vibrio cholerae, Salmonella, Shigella, C difficle
|
|
|
Osmotic Diarrhea - Pathophysiology - Features - Example pathogens |
Caused by osmotic gradient in the colon from altered bacterial gut flora, damage to the mucosal absorptive surface, or ingestion of substances
Reduction in stool volume with fasting, pH < 6, reducing substances present
Viral gastroenteritis |
|
|
Dysentery |
Diarrhea with blood and mucus in stool indicating compromise of bowel wall
May have fever/white count
Samonella, Shigella, Campylobacter |
|
|
Common Causes of Infectious Diarrhea |

|
|
|
Spectrum of illness associated with nontyphoidal Samonella |
Asymptomatic carrier state Acute gastroenteritis Bacteremia Disseminated abscess syndrome |
|
|
Animal reservoirs for nontyphoidal Samonella |
Poultry Livestock Reptiles
Transmission is usually through foods such as poultry, beef, eggs, and dairy products.
|
|
|
Whom to treat for non-typhoidal Samonella |
Infants younger than 3 months Complications - Longer than 5-7 days without improvement - Bacteremia - Focal infection: CNS, pericardium, joint, kidney - Immunosupressed - Asplenia
Rx is with Ampicillon, Amoxicillin, Septra |
|
|
Most common cause of dysentery in North America |
Shigella Sonnei |
|
|
Complications of shigella |
Reactive Arthritis Bacteremia HUS Encephalopathy |
|
|
Antibiotics for shigella |
Prolonged symptoms Dysentery Immunocompromise |
|
|
Campylobacter jejuni |
Transmitted by ingestion of contaminated |
|
|
Yersina Entercolitica |
Can cause dysentery and appendicitis like syndrome due to reactive mesenteric adenitis
Transmission from from eating undercooked pork or drinking unpasteurized milk
Antibiotics are indicated for the immunocompromised with enterocolitis and in cases of septicemia and extraintestinal infections. |
|
|
Colstridium difficule |
Spectrum of illnesses ranging from asymptomatic to watery diarrhea to pseudomembranous colitis
Risk factors: Hospitalization, antibiotics within 60 days
Complications: Intenstinal perforation, toxic megacolon
Fecal-oral transmission |
|
|
Toxin mediated diarrheas |
Clostridium perfingens S. Aureus |
|
|
Vibrio cholerae |
Ingestion of contaminated food/water in returning traveler
Mechanism: Heat-labile enterotoxin that increases cAMP through adenylate cyclase, resulting in inhibition of sodium reabsorption with chloride and fluid secretion into the gut
Antibiotics for moderate to severe disease
Complications: Dehydration, hypokalemia, metabolic acidosis, and occasionally hypovolemic shock |
|
|
Vibrio Parahemolyticus |
Found in seawater, shellfish, and fish
Transmission via ingestion of contaminated raw or undercooked seafood |
|
|
Subtptypes of E coli by somatic/flagellar antigens |
ETEC (Enterooxicogenic) - Secretory diarrhea EIEC (Enteroinvasive) - Shigella like dysentery EPEC (Enteropathogenic) - sporadic and endemic diarrhea outbreak that can become chronic EAEC (Enteroagretative) - Prolonged diarrhea
EHEC (Enterohemorhagic)/ STEC (Shiga toxin producing E Coli) - Bloody diarrhea without fever - E Coli O157:H7 is prototype
|
|
|
Hemolytic Uremic Syndrome Triad |
MAHA Thrombocytopenia Renal Failure |
|
|
Prototypical HUS Culprit |
E Coli O157:H7 |
|
|
Infectious Diarrhea for which Azithromycin is 1st line |
Campylpobacter ETEC Shigella |
|
|
Infectious Diarrhea for which Septra is 1st line |
Yersinia Non-typohidal Samonella
|
|
|
Abx for Vibrio Cholerae |
Doxycycline Tetracycline |
|
|
Assessing Degree of Dehydration - Pediatric |
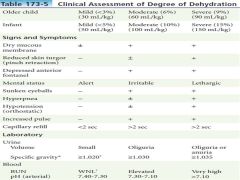

|
|
|
Stool analysis |
C & S O & P Microscopy for leukocytes, occult blood Consider fecal electrolytes fat, ELISA for viruses, |
|
|
Patients at increased risk with infectious diarrhea in whom antibiotics should be considered |
septicemia immunosuppression chronic diseases premature articular or valve prostheses
Antibiotics are also recommended |
|
|
Antibiotics for cryptosporidium |
Nitazoaxnidie |
|
|
Antibiotics for Giardia |
Metronidazole |
|
|
Entamoeba Histolytica |
Metronidazole followed by Iodoquinol |
|
|
Causes of Dehydration |
Decreased intake (e.g stomatitis) Increased outputs (e.g. Gastroenteritis, diabetes) Increased insensible losses (e.g. Fever) |
|
|
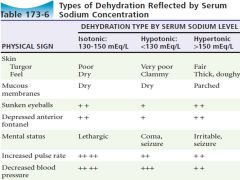
Types of Dehydration as characterized by serum sodium |
|
|
|
Differential Diagnosis of Volume Depletion |
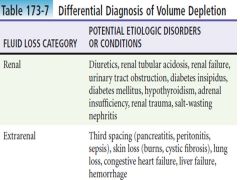

|
|
|
How to make ORS at home |
1 liter of water 6 teaspoons sugar 1/2 teaspoon of salt |
|
|
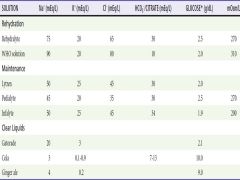
Composition of Common ORS |
|
|
|
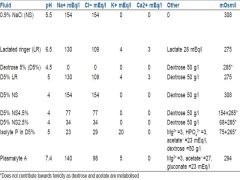
Composition of common IV Fluids |
|
|
|
Indications for Zofran in CAEP Pathway |
- Needs ORS (5-10% Dehyrdated) - Significant vomitting (6 or more times in last 6 hours) - Vomitted within last 60 minutes |
|
|
Zofran dosage as per CAEP pathway |
0.2mg/kg for less than 8kg 2mg if child 8 - 15 kg 4mg if child 15 - 30 kg 8mg if child >30 kg |
|
|
Criteria for Discharge as Per CAEP pathway |
Taking ~15ml/kg/hr ORS Well appearing with Normal VS Gorelick score less than/equal to 1 At least 2 % weight gain Not vomitting/diarrhea excessively (2 X q 30 minutes) |
|
|
CAEP suggested criteria for admission/consult |
Continued significant vomitting/diarrhea Hyper/hypo natremia Significant social issues Diagnostic uncertainity Required resuscitiation for abnormal VS/LOC Persistent metabolic acidosis |
|
|
Inclusion and Exclusion criteria for CAEP pediatric vomitting and diarrhea pathway |
Inclusion Age 3 months - 10 Years with vomitting/diarrhea
Exclusion Chronic medical problem Localized abdominal pain Vomitting/Diarrhea for > 7 days duration S/S of abdominal obstruction |
|
|
Abbreviated Gorelick Score Used in CAEP Pathway |
Gorelick Score - CR > 2 seconds - Absence of tears - Dry MM - Ill general apperance
0-1: Mild (<5%; ORS & early D/C) 2: Moderate (5-10%; ORS +/- Zofran) 3-4: Severe (>10%) Shock: Resuscitate |
|
|
Replacement for Ongoing Vomitting and Stool |
2ml/kg: Emesis 10ml/kg: Stool
8ml/kg as per CAEP |
|
|
Phases of IV Rehydration for Vomitting/Diarrhea |
Phase I: Emergency Phase: Restore circulatory volume
Phase II: Repletion phase: Fluid and electrolyte derangement reversed with replacement of ongoing losses over 1st 24 hours
Phase III: Early refeeding phase: Recovery of fluid, electrolyte, and nutritional homeostasis -> 1st few days |
|
|
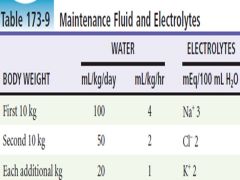
Pediatric Maintenance Fluids and Electrolytes |
|
|
|
Salmonella typhi infection
- Epidemiology - Features - Treatment |
Human to human transmission, more commonly international traveler
Typhoid fever: Febrile generalized illnesses, rose spots, HSM Rx: Ceftriaxone pending susceptibility |
|
|
Why kids more prone to dehydration with gastroenteritis
|
Larger ECF space compared with adults
Increased BSA Higher metabolic rate Less metabolic stores |
|
|
Most common Bacterial Causes of Bacterial Diarrhea
|
Y yersinia
E E coli C Camplyobacter S Shigella S samonella |

