![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
82 Cards in this Set
- Front
- Back
|
Why do humans need a cardiovascular system?
|
Limitations of diffusion
Limitations of surface area as organisms become larger |
|
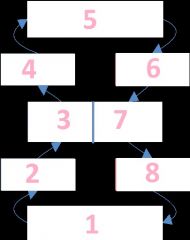
Name the order that blood flows in the circulatory system
|
Systemic Capillaries (body)
Systemic Veins Right heart Pulmonary arteries Lungs Pulmonary veins Left heart Systemic arteries |
|
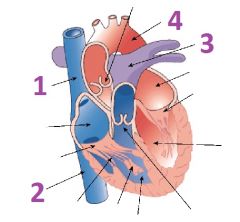
Name the arteries and veins of the heart
|
1- Superior vena cava
2- Inferior vena cava 3- Pulmonary trunk 4- Aorta |
|
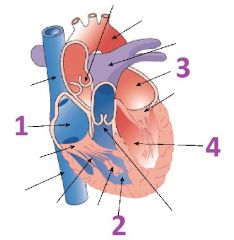
Name the four chambers of the heart
|
1- Right atruim
2- Right ventricle 3- Left atrium 4- Left ventricle |
|
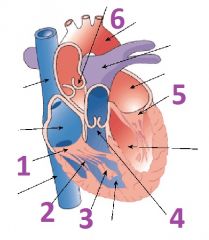
Name the valves and associated anatomy of the heart
|
1- Right atrioventricular (tricuspid) valve
2- Chordea Tendinae 3- Papillary muscle 4- Pulmonary (pulmonary semilunar) valve 5- Left atrioventricular valve (bicuspid or mitral) valve 6- Aortic (aortic semilunar) valve |
|
|
What occurs in ventricular systole?
|
The left and right ventricles contract simultaneously.
AV valves immediately close Semilunar valves open after a brief delay |
|
|
What occurs in ventricular diastole?
|
Left and right ventricles relax simultaneously
Semilunar valves immediately close AV valves open after a brief delay |
|
|
What occurs in Passive filling?
|
Ventricles are in diastole
Atria are in diastole AV valves are open Semilunar valves are closed |
|
|
What occurs in active filling?
|
Ventricles are in diastole
Atria are in systole AV valves are open Semilunar valves are closed |
|
|
What occurs in Isovolumic ventricular contraction?
|
Ventricles are in systole
Atria are in diastole AV valeves are closed Semilunar valves are closed |
|
|
What occurs in ventricular ejection?
|
Ventricles are in systole
Atria are in diastole AV valves are closed Semilunar valves open |
|
|
What occurs in Isovolumic ventricular relaxation?
|
Ventricles are in diastole
Atria are in diastole AV valves are closed Semilunar valves are closed |
|
|
What is the end diastolic volume?
|
135 ml
|
|
|
What is the end systolic volume?
|
65 ml
|
|
|
What is the stroke volume?
|
EDV-ESV= SV
135-65= 70 |
|
|
What are the two types of cells in the heart?
|
Contractile cells (99%)
Do the work Autorhythmic cells (1%) Set the pace |
|
|
What connects contractile cells?
|
Intercalated discs (gap junctions) They allow for more surface area and make it possible for action potential permiablility
|
|
|
Describe cardiac signal transduction.
|
1. the cardiac action potential arrives at the cardiac contractile cell from an adjacent cell via gap junctions
2. Ca++ flows into the cytosol from the ECF and the SR 3.Ca++ binds to troponin, which is found in the actin filament, this causes topomyosin to expose the active sites on the g-actin. 4. Myosin heads attach and go through the power stroke 5. Ca++ is pumped back into the SR and ECF, which causes the tropmyosin to cover the active sites on the actin, the cell relaxes |
|
|
What is the resting membrane potential of a contractile cell?
|
-90 mV
|
|
|
The action potientail of a contractile cell lasts about 250 msec, what consequences do this long action potential cause?
|
Maximum heart rate is limited to less than 240 BPM
Long refractory period prevents tetanus in cardiac muscle |
|
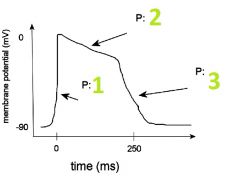
Name each phase of the action potential and state what ion the membrane is most permiable to during that time.
|
1. Depolarization, Na+
2. Plateu, Ca++ 3. Repolarization, K+ |
|
|
What is the membrane potential of autorhythmic cells?
|
-40 mV
|
|
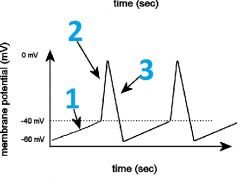
Name the part of the action potential and what ion the membrane is most permeable to.
|
1- Pacemaker potential, Na+
2- Depolarization, Ca++ 3- Repolarization, K+ |
|
|
Describe what effect the sympathetic system has on the stimulation of autorhythmic cells
|
NE and E increase the influx of Na+ and Ca++ influx
It increases the heart rate throught the first four throactic spinal nerves, targeting the SA and the AV nodes |
|
|
Describe what effect the parasympathetic system has on the stimulation of autorhythmic cells.
|
ACh increases K+ permeability and decreases Ca++ permeability
Decreases heart rate throught the Vagus Nerve (cranial nerve X), targeting the SA and AV nodes. |
|
|
What sets the pace for the heart and why?
|
SA node
The Autorhythmic cells of the SA node are set at the fastest clock, with the fastest depolarization cycle. |
|
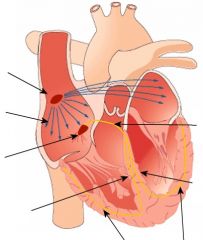
Describe the electrical coordination of the heart contraction.
|
The signal (action potential) begins at the SA node.
Travels through the internodal pathways Temporarily pauses at the AV node Travels down the bundle of HIS and down the left and right bundle branches Reaches the apex of the heart and draves up the ventricle outer walls via the purkinje system |
|
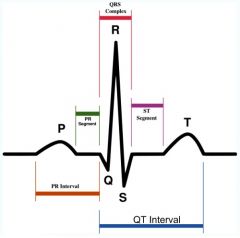
Describe what is happening at the P wave.
|
Produced by atrial depolarization
Marks the beginning of atrial systole |
|
|
Describe what is happening at the QRS complex.
|
Produced by ventricular depolarization
Marks the end of atrial systole and the beginning of ventricular systole |
|
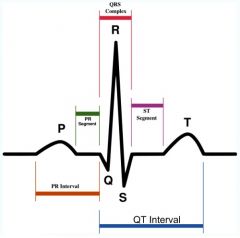
Describe what is happeneing at the QRS complex.
|
Produced by ventricular depolarization
Marks the end of atrial systole and the beginning of ventricular systole |
|
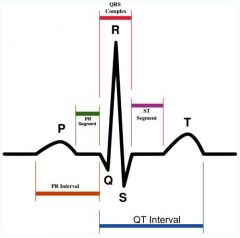
What is happening at the T wave?
|
Produced by ventricular repolariztion
Marks the end of ventricular systole |
|
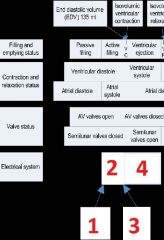
Describe the electrical system during the cardiac cycle
|
1- signal begins at SA node
2- Internodal pathways 3- Pause at AV node 4- Conduction down the septum and up the outerwalls |
|
|
What is bradycardia?
|
Less than 60 BPM
|
|
|
What is tachycardia?
|
Greater than 100 BPM
|
|
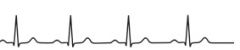
What kind of an abnormal ECG is this?
|
First degree (partial) AV block
conduction through AV node slowed, resulting in a long P-Q interval |
|
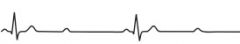
What is this abnormal ECG called?
|
Second-Degree AV block (2:1)
conduction through AV node does not always occur, resulting in some P waves that do not result in a QRS. |
|

What is this abnormal ECG called?
|
Third-Degree (complete) AV block
conduction through AV node completely blocked, resulting in P waves and QRS that are completely dissociated. |
|
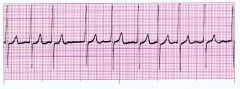
What is the abnormal heart rhythm called?
|
Atrial fibrillation.
Contains obvious QRS waves but no defined P or T waves. The atria are fluttering and atrial systole is not occuring. Not immediately fatal because ventricles will fill passively |
|
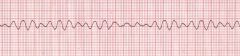
What is this abnormal heart rhythym called?
|
Ventricular fibrillation
contains no clearly discernible waves. Ventricles are fluttering and ventricular systole is not occurring. Fatal within seconds. |
|
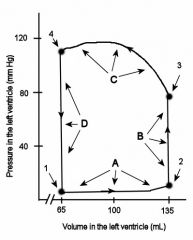
Describe what is happening at each of the points
|
1- mitral valve opens
A- ventricular filling, first passive then active 2- mital valve closes B- isovolumic vetricular contraction 3-Aortic valve opens C- ventricular ejection 4- aortic valve closes D- Isovolumic ventricular relaxation |
|
|
what is happening at B and C in the ventricles?
|
Ventricular systole
|
|
|
Describe how the first heart sound is produced.
|
Produced by the highly turbulent flow of blood through the AV valves as they close.
"Lub" Lower in pitch and longer |
|
|
Describe how the second heart sound is produced.
|
Produced by the highly turbulent flow of blood through the semilunar valves as they close.
"Dup" Higher in pitch and shorter |
|
|
What is a heart murmur?
|
ANy abnormal sound that occurs at any time during the cardiac cycle.
|
|
|
What would cause a diastolic heart murmur?
|
Lub Dup Swoosh
Stenosis of an AV valve Incompetence of a semilunar valve |
|
|
What would cause a systolic heart murmur?
|
Lub Swoosh Dup
Stenosis of a semilunar valve incompetence of an AV valve |
|
|
Describe an Artery
|
4mm diameter
1 mm thick Connective, smooth muscle, and endothelium tisses Very elastic |
|
|
Describe an arteriole
|
.03mm diameter
.005 mm thick smooth muscle and endothelium Very muscular and innervated |
|
|
Describe a capillary
|
.008 mm diameter
.0005 mm thick endothelium tissue very permiable |
|
|
Describe a venule
|
.03 mm diameter
.001 mm thick Connective and endothelium tissue |
|
|
Describe a Vein
|
5mm diameter
.5mm thick connective, smooth muscle, and endothelium tissue Highly distensible |
|
|
What are the five things that blood pressure is dependent upon?
|
1: ventricular contraction rate
2: ventricular contraction force 3: arteriole radius 4: total blood volume 5: distribution of blood volume |
|
|
What controls the ventricular contraction rate?
|
parasympathetic stimulation
sympathetic stimulation |
|
|
What controls the ventricular contraction force?
|
Sympathetic stimulation
|
|
|
What is the relationship between force and rate of heart contractions and cardiac output?
|
HR * SV = CO
|
|
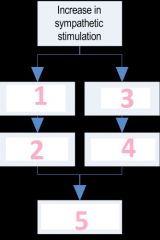
Name the steps during an increase in sympathetic stimulation
|
1) ventricular myocardium
2) SV increases 3) SA node 4) HR increases 5) CO increases |
|
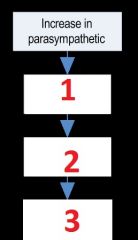
Describe the effects of an increase in the parasympathetic stimulation
|
1) SA node
2) HR decreases 3) CO decreases |
|
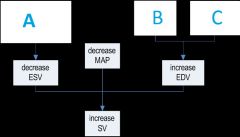
What three factors affect stroke volume?
|
A) Sympathetic stimulation of ventricular myocardium
B) Better venous return C) Stronger atrial systole |
|
|
Sympathetic stimulation controls arteriole diameter via _____ on ______ receptors (vasoconstriction) and _______ on ________ receptors (vasodilation).
|
NE
Alpha E Beta 2 |
|
|
What are the 6 main types of capillary beds?
|
Brain
Heart GI tract Muscle Kidney Other tissue |
|
|
What is the point of valves in veins?
|
valves keep blood from going in the wrong direction.
|
|
|
How many total liters of blood does an adult have in their body
|
5
|
|
|
Describe how much blood is in the heart, systemic arteries and arterioles, systemic capillaries, systemic veins and venules, and the pulmonary circut at one time?
|
Heart ~ .4L
Arteries and Arterioles~ .8L Capillaries~ .2 L Veins and Venules ~ 3L Pulmonary Circut ~ .6 L |
|
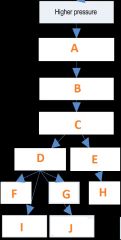
Fill in the pathway for the Baroreceptor reflex
|
A) Increase in AP firing frequency back to CNS
B) Integration by CNS (brainstem) C) efferent signals out to the body D) decrease in sympathetic E) Increase in para sympathetic F)Decrease SV G) Decrease HR H) Decrease HR I) Vasodilation of arterioles J) Decrease in venomotor tone |
|
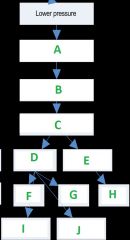
Fill in the blanks for the baroreceptor reflex pathway
|
A) Decrease in AP firing frequency back to CNS
B) Integration by CNS (brainstem) C) Efferent signals out to the body D) Increase in sympathetic E) Decrease in parasympathetic F) Increase in SV G) Increase in HR H) Increase in HR I) Vasoconstricion of arterioles J) Increase in venomotor tone |
|
|
State the changes that occur immedately after a significant hemmorrhage in blood volume, HR, SV, CO, Peripherial resistance, MAP
|
Blood Volume: Decrease
HR: none SV: decrease CO: Decrease Peripheral resistance: None MAP: Decrease |
|
|
State the changes that occur in a hemorrhage after the baroreceptor reflex has responded in blood volume, HR, SV, CO, peripheral resistance, MAP
|
Blood volume: Decrease
HR: Increase SV: Increase, but still below original value CO: Increase, but still below original value peripheral resistance: increase MAP: increase, but still below original value |
|
|
State the changes that occur immediately after a saline infusion for blood volume, HR, SV, CO, Pheripheral resistance, MAP
|
Blood volume: Increase
HR: None SV: Increase CO: Increase Peripheral resistance: None MAP: Increase |
|
|
State the changes that occur after infusion and after the baroreceptor reflex has responded for blood volume, HR, SV, CO, Peripheral resistance, MAP
|
Blood Volume: Increase
HR: Decrease SV: Decrease, but still above original value CO: Decrease, but still above original value Peripheral resistance: Decrease MAP: Decrease, but still above original value |
|
|
When do you hear Kortokoff sounds?
|
During ventricular systole
|
|
|
What is the equation for MAP?
|
MAP= DP + (PP/3)
|
|
|
Sympathetic stimulation controls arteriole diameter via _____ on ______ receptors (vasoconstriction) and _______ on ________ receptors (vasodilation).
|
NE
Alpha E Beta 2 |
|
|
What are the 6 main types of capillary beds?
|
Brain
Heart GI tract Muscle Kidney Other tissue |
|
|
What is the point of valves in veins?
|
valves keep blood from going in the wrong direction.
|
|
|
How many total liters of blood does an adult have in their body
|
5
|
|
|
Describe how much blood is in the heart, systemic arteries and arterioles, systemic capillaries, systemic veins and venules, and the pulmonary circut at one time?
|
Heart ~ .4L
Arteries and Arterioles~ .8L Capillaries~ .2 L Veins and Venules ~ 3L Pulmonary Circut ~ .6 L |
|
|
What are the three organs that require more cardiac output during exercise?
|
Skin
Muscle Heart |
|
|
What are the driving forces for movement in and out of capillaries?
|
Concentration gradients
Pressure gradients |
|
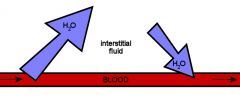
What pressure gradients cause the mass flow of water in and out of the capillaries?
|
Out: Blood pressure (38) is slightly higher than osmotic pressure, causing water to flow out of the capillaries
In: Over distance the blood pressure will decrease below 25 which will cause water to be reabsorbed into capillaries |
|
|
What causes hypertension?
|
Carotid and aortic baroreceptors are down regulated.
|
|
|
What is a beta blocker?
|
Hypertension medication that acts antagonistically on cardiac beta one receptors, reducing the ability of catecholamines to stimulate the heart.
|
|
|
What is an ACE inhibitor?
|
Hypertension medication that promotes vasodilation by reducing the conversion of angiotensin I to angiotensin II, which normally promotes vasoconstriction.
|

