![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
34 Cards in this Set
- Front
- Back
|
Osteogenic Cells
|
Are spindle shaped connective tissue cells - derived from mesenchyme located in periosteium and endosteym.
Differentiate into osteoblasts which secrete the organic matrix that entraps these cells |
|
|
Affect of low O2 on osteogenic cells?
|
May cause them to change into chondriogenic cells.
|
|
|
Osteocytes
|
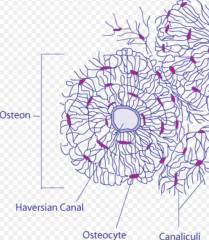
Are entrapped (live in cavities) called lacunae. Derive from osteoblasts which become trapped in the matrix that they secrete.
Are mature bone cells housed in lacunae and maintain communication through gap junction extending through canaliculi |
|
|
Osteoclasts
|
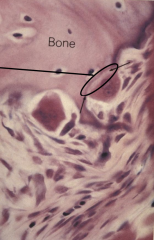
Osteolyis by creating acid environment that decalcifies bone. Acid hydrolases, collgenous and enzymes degrade decalcified material and cell reabsorbs it. They are derived from monoblasts and are giant multinucleated cells. Are located in depression called Howship's lucanae.
|
|
|
Periosteum and Endosteum
|
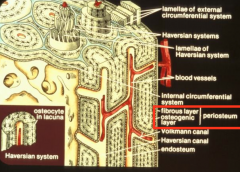
Periosteum is dense irregular connective tissue that is a membrane that lines the outside of bones. Contains inner layer of osteogenic cells and osteoblasts.
Functions to supply blood to bone. Appositional growth occurs from osteoblasts from periostium. |
|
|
Bone Matrix composition
|
Organic portion is made of 95% type 1 collagen and ground substance. Contains chondroitin 4 sulfate, chondroitin 6 sulfate and osteomucoid. Has abundance of tyrosine and leucine.
Inorganic portion - 50% dry weight of calcium |
|
|
Sharpey's Fibers
|
Are collagen fibers of the periostium that penetrate the bone matrix, function to attach periosteum to bone.
|
|
|
Osteoblasts
|
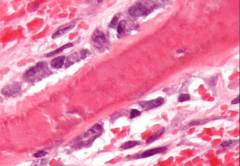
Derived from osteogenic cells, basophilic. Resemble cuboidal layer as the secrete matrix. As synthesis declines, they become flat. Have cytoplasmic processes that bring them into close contact with other osteoblasts
PAS positive granules - prescursors of GAGS -becomes entrapped in ow matrix and ceases function to become osteocyte |
|
|
4 Regions of Osteoclasts:
|
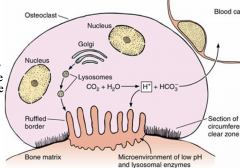
1) Ruffed Border - finger live evaginations where active absorption occurs
2) Vesicular region - composed of vesicle-like structures 3) Clear Zone - region of cytoplasm around ruffed border containg microfilaments, which assist osteoclast in keeping contact with bony surface 4) Basal Region - houses the organelles and nuclei |
|
|
Bone Reabsorption
|
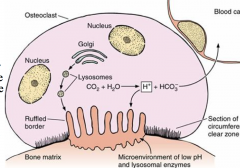
Lysozmal enzymes packed in golgi and H+ produced are released into attached bone matrix. acidification of this space facilitates calcium phosphate breakdown from bone. Bone matrix is removed and resorption takes place into cytoplasm of osteoclasts. Digested further and transferred to blood.
|
|
|
Compact Bone and Spongy bone
|
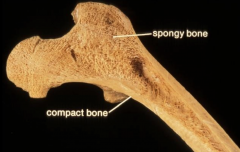
1) Adult bone where matrix is laminated. Is very dense.
2_ Filled with spaces, contain bone marrow in long bone - either red hemopoietic cells or yellow fat. |
|
|
Primary Bone
|
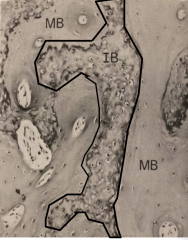
Is immature bone (IB) or woven bone. Contains high osteocytes and irregular collagen.
Is remodeled and replaced by secondary or mature bone, except in places like tooth or tendon insertion sites. |
|
|
Secondary Bone
|
Is mature or lamellar bone
Contains haversion system or osteons. Has calicifed matrix arranged in layers of lamellae surround H-cannel. |
|
|
Lamellae
|
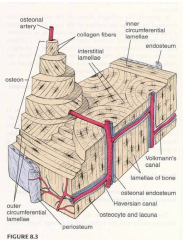
Have special arrangement in diaphysis, there is outer and inner circumferential as well as the Haversion systems.
|
|
|
Volkmann's Canal
|
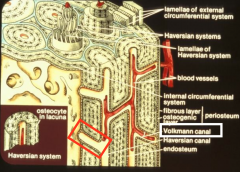
Connects haversion canals to the marrow cavity
|
|
|
Endosteum
|
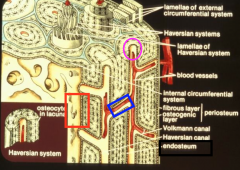
Consists of osteogenic cells which line the marrow cavity, volkmann's canal and the Haversion canal.
|
|
|
Development of Haversion System - 1
|

1) New Haversion forms under periosteium, longitudinal ridges form and periosteal cell differentiate into osteoblast
2) ridges fuse and groove becomes a bony tunnel enclosing BV |
|
|
Development of Haversion System -2
|

3) Additional bone lamellae are deposited around the tunnel and converted into haversion canal
4) Volkmann canal extending across diaphysis, appositional growth widens the shaft of the bone |
|
|
Intramembranous Bone formation
|
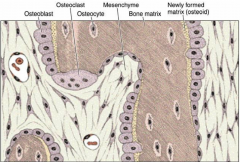
Involves bone formation development within layer of condesned mesenchyme.
- beings with mesenchymal cells condensing to form primary ossification center, give rise to osteoblasts which secrete osteoid. -spongy bone first developed then BV invade and ossification centers fuse -flat bones of skull are formed this way |
|
|
Bone Trabeculae
|
Fused spicules - name given to bone developing at these sites.
|
|
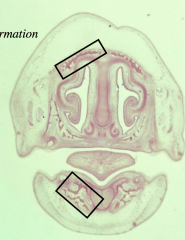
Know these slides
|
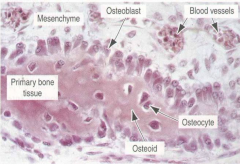
|
|
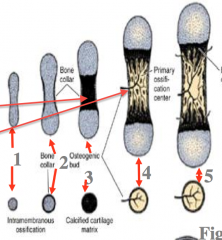
Endochondral Bone Formation
|
Occurs via a hyaline cartilage template that is laid down and then replaced with bone
1) outline of bone in cartilage 2) formation of periosteum 3) cartilage is calcified 4) Formation of periosteal bud, which have osteogenic cells and BV (primary ossification) |
|
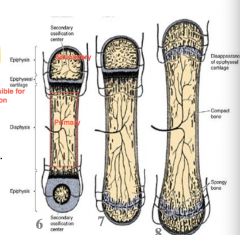
|
6) Secondary ossification centers form in epiphyses. Epiphyseal plate (cartialge) forms between primary and secondary ossifcationc enters
3) epiphyseal plate eventuallly disappears 2) Diaphysis and epiphysis marrow cavities fuse |
|
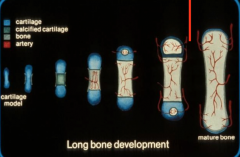
How is the secondary ossification center involved growth?
|
Epiphyseal plate adds new cartilage at one end while being replaced at other end. Diapyseal bone and epiphyseal bone eventually become continuos at 20 years.
|
|
|
What are the 5 distinctive zones at the epiphyseal plate?
|
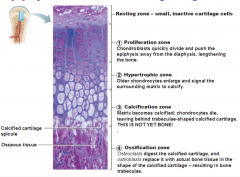
Zone of Reserve Cartilage - contains cartilage with small inactive chondrocytes
Zone of cell proliferation: - rapid mitotic divisions five rise to row of cartilage cells Zone of Cell maturation and hypertrophy: chondrocytes become enlarged and contain glycogen Zone of Calcifying cartilage: cartilage becomes calcified Zone of provisional ossification - osteoclasts and osteoblasts break down calcified cartilage and replace with bone |
|
|
Process of Bone Repair
|
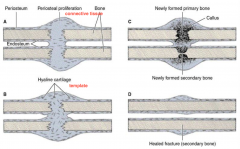
1) Hemorrhaging is followed by blood blotting and macrophages remove much of debris
2) Fibroblasts proliferate in periosteium and endosteum to form callus 3) Chondrocytes also differentiate from connective tissue to form cartilage that is replaced by bone via endocondral bone formation - forming bony callus 4) Bony callus is reabsorbed and replaced with secondary bone |
|
|
Functions of bone
|
-support for body and attachment of muscles
-dynamic tissue, undergoes changes in shape -growth is directed toward applied stress and resorption where pressure is applied -99% calcium reserve |
|
|
Importance of Vitamin D
|
Can results from low instake calcium which results in inadequate absorption of vitamin D in intestine. Results in poorly calcified bone. Leads to rickets in children and osteomalacia in adults.
- Needed for ossification, too much causes resorption |
|
|
Importance of Vitamin A
|
Deficiency inhibits proper bone formation and growth, while excess accelerate ossification of epiphyseal plates. Results in small stature
|
|
|
Importance of Vitamin C
|
Needed for collage formation, its deficiency results in scurvy, characterized by poor bone growth
|
|
|
Parathyroid Hormone influence on bone
|
Stimulates osteoclasts to resorb and release calcium, elevation blood calcium. May active osteocytes to initiate osteolysis from their lacunae, elevate blood calcium
-Excess renders bone more susceptible to fracture and calcium deposition in arterial walls and kdiney |
|
|
Calcitonin influence on bone
|
Hormone inhibits matrix resorption, preventing release of calcium
|
|
|
Pituitary Growth Hormone
|
Stimulates epiphyseal cartilage growth. Excess produces giant and lack produces dwarf.
|
|
|
Sex Hormone influence
|
Influences epiphyseal ossification. Excess results in small stature, lack results in tall stature.
|

