![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
256 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
What is the isoelectric line? |
the baseline above and below which the waveform travels (in a biphasic wave)
|
|
|
|
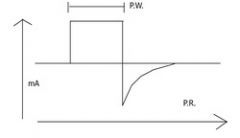
What is an asymmetrical, biphasic wave? |
A wave that is not symmetrical above and below the isoelectric line |
|
|
|
Why is frequency/pulse rate important in TENS setup? |
because different frequency settings target different nerve groups and the setting will determine if the "Gate Theory" or "Endorphin Theory" of TENS will be in effect
|
|
|
|
Why is pulse duration/pulse width important in TENS setup?
|
in general, the higher the pulse width, the more aggressive the stimulation feels (and less comfortable) |
|
|
|
Simply put, amplitude in a TENS unit is
|
what you feel when you turn the unit up, it's what causes the buzzing sensation of the TENS to go higher or lower |
|
|
|
Which TENS modes work on the Gate Control theory? |
conventional |
|
|
|
Which TENS modes work on the Endorphin theory? |
low frequency |
|
|
|
TENS is used only for |
pain control
|
|
|
|
Which fibers are believed to open pain gates? |
A–delta (small, myelinated, acute) and |
|
|
|
Which fibers are believed to close pain gates?
|
A–beta (large, heavily myelinated) |
|
|
|
How do the Gate Control and Endorphin theories affect pain with the application of TENS? |
– Gate Control tends to only work for the duration of the application; that is, there is little carry–over effect (thus treatment time for conventional is up to 24 hours) |
|
|
|
Another name for low–frequency TENS?
|
acupuncture TENS
|
|
|
|
Brief intense mode of TENS may achieve rapid relief of intense acute pain, however:
|
some patients may find the stimulation to be too much and may not be able to tolerate it for the treatment time required to achieve the desired results
|
|
|
|
Through which pain control theory is brief intense TENS thought to work?
|
through both
– Gate Control and – Endorphin theories because the pulse duration/pulse width is high – Endorphin, and frequency/pulse rate is high – Gate Control |
|
|
|
What tends to happen to patients that are mobile during TENS application?
|
they tend to lose the electrodes
|
|
|
|
What is the minimum number of electrodes needed for TENS application?
|
2 |
|
|
|
Contraindications for ES
|
– cancer
– phlebitis, thrombus, thrombophlebitis – pacemaker, other internal electrical device – arrhythmia – over carotid sinus – transcerebral – transthoracic – over fresh fracture – hemorrhage |
|
|
|
How far apart should TENS electrodes be placed?
|
– at least one inch
– ideally, the width of the electrode |
|
|
|
When a twitch is produced by a TENS treatment, where does it appear?
|
may be
– under the electrodes – between the electrodes |
|
|
|
How does pulse duration/pulse width of TENS relate to comfort?
|
imagine it like a needle
narrower needle goes into arm more comfortably wider needle hurts more |
|
|
|
Electricity is the force created by an imbalance in the number of negatively charged *** between two points known as *** |
electrons, poles |
|
|
|
Electric current takes the path of *** *** from the negative poles (cathode) an area of high electron concentration to the *** or positive pole and area of low electron concentration |
least resistance, anode |
|
|
|
What charged particles flow in human tissue? |
ions |
|
|
|
What is a charge? |
an excess or deficiency of electrons |
|
|
|
What is the charge of an atom? |
neutral |
|
|
|
What is an ion? |
a particle with a charge (either positive or negative) |
|
|
|
What is voltage? |
the potential difference between two points in an electrical field, V= I / R, volts = amps / ohms |
|
|
|
What are Ohms (symbol R) |
unit of electrical resistance Ohm's Law says that current is directly proportional to voltage and inversely proportional to resistance I = V / R amps = volts / ohms |
|
|
|
Amperage (symbol I) |
amperes (amps) the rate at which electrical current flows. 1 amp = 1 coulomb/sec I=V / R, amps = volts / ohms |
|
|
|
Capacitance |
the ability to store energy by means of an electrostatic field that provides frequency dependent resistance to electric current flow |
|
|
|
One coulomb = |
the basic unit of charge
1 ampere / sec |
|
|
|
What is power (symbol P)? |
voltage * current |
|
|
|
What is resistance? |
opposition to movement by charged particles |
|
|
|
How is resistance measured? |
ohms |
|
|
|
Inductance |
the ability to store electrical energy by means of an electromagnetic field measured by the henry |
|
|
|
In AC inductance and capacitance resist current flow and are collectively known as *** |
Impedance, uses symbol Z |
|
|
|
What is Ohm's Law? |
flow of current is directly proportional to EMF (current) and inversely proportional to resistance of circuit |
|
|
|
What is conductance? |
ease with which current is allowed to pass symbol is mho |
|
|
|
What is a conductor? |
a material through which electricity flows easily |
|
|
|
What is an insulator? |
a material through which electricity does not flow easily |
|
|
|
What is the best conductor in the body? Followed by....? |
best conductor in body is nerves |
|
|
|
What is AC? |
alternating current |
|
|
|
What is DC? |
direct current |
|
|
|
Describe a DC and an AC waveform. |
DC – unidirectional flow |
|
|
|
What is the conventional theory of current flow? |
current flows from cathode to anode |
|
|
|
What is the electron theory of current flow? |
current flows from negative to positive pole |
|
|
|
What types of modes are available for E–stim? |
– continuous |
|
|
|
What is burst mode? |
a finite series of pulses delivered in a package or envelope as a single pulse at a defined frequency |
|
|
|
What is interrupted mode? |
current flows for at least one second and ceases to flow for at least one second, usually with a hand–held electrode where one manually opens and closes the circuit |
|
|
|
For what is interrupted mode used? |
– trigger points |
|
|
|
What shapes may a waveform take? |
may take any of the following shapes and with each may also be symmetrical or asymmetrical |
|
|
|
What pulse types may the waveform take? |
– monophasic (pulse deviates in one direction––DC) |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/8/5/51758402_m.jpg |
|
|
How does the TENS unit convert the DC charge from the 9V battery to AC (biphasic)? |
via a transducer in the unit |
|
|
|
What are the characteristics of a balanced biphasic wave? |
– it has the same amount of charge both above and below the isoelectric line |
|
|
|
Can a biphasic wave be balanced without being symmetrical? |
Yes |
|
|
|
How is DC frequency measured? |
in pulses per second (pps) |
|
|
|
How is AC frequency measured? |
in cycles per second (cps) |
|
|
|
Pulse width is also known as: |
pulse duration |
|
|
|
Waveform of a TENS unit? |
biphasic, asymmetrical |
|
|
|
What are the three main parameters to remember with E–stim? |
– Phase / pulse duration (width) – beginning to end of phase or pulse Amplitude Frequency
|
|
|
|
What is the intrapulse (a.k.a. interphase) interval? |
the time between two successive components of a pulse when no electrical activity occurs |
|
|
|
What is the interpulse interval? |
the time between the end of one pulse and the start of the next pulse |
|
|
|
What is rise time? |
the time from baseline (0) to peak amplitude |
|
|
|
What is decay time? |
the time from peak amplitude back to baseline (0)
|
|
|
|
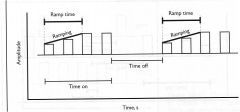
What is ramp time? |
the time it takes to reach peak amplitude of a pulse train |
|
|
|
What is total current? |
current delivered to tissue/sec |
|
|
|
How can one increase the total current delivered? |
increase the |
|
|
|
What is considered |
– less than 100 volts |
|
|
|
What is considered |
– up to 1,000 pps/cps/Hz |
|
|
|
How high does the frequency go in a TENS unit? |
up to roughly 120 pps, which is considered "high" even though that rate places it in the "low frequency" category |
|
|
|
What types of electrodes are used with E–stim? |
metal plate (need wet sponges) |
|
|
|
What are the considerations for electrode use? |
– size should fit treatment area |
|
|
|
Pulse Period |
pulse duration + interpulse interval + intrapulse interval |
|
|
|
How can electrodes be placed to get deeper tissue penetration?
|
place them farther apart
|
|
|
|
Why does a smaller electrode deliver a higher current density? |
a smaller electrode is still conducting the same amount of current, therefore it will be concentrated in a smaller space |
|
|
|
How does polarity affect treatment? |
anode – positive pole |
|
|
|
What three types of electrode configurations can be used? |
– monopolar – 1 active electrode (smaller) on the target, and 1 dispersive electrode |
|
|
|
What are the basic uses of ES? |
– pain modulation (gate control/endogenous opiates) |
|
|
|
How are endogenous opiates (Endorphin theory) produced by ES? |
– low rate (1–5 pps) |
|
|
|
Breakdown of E–stim: |
NM – neuromuscular |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/9/5/51759461_m.jpg
|
|
|
Precautions for ES |
– cardiac disease |
|
|
|
When considering in ES:
– pulse duration/pulse width – amplitude – frequency/rate what is more comfortable to the patient? |
generally speaking
– shorter pulse duration/width is more comfortable – amplitude varies by patient tolerance – higher frequency/rate is more comfortable |
|
|
|
What is interference? |
the superposition of 2 or more waves, resulting in a new wave pattern |
|
|
|
What is IFC? |
– use of 2 sinusoidal current sources of medium frequency (1,000–10,000 Hz), created by two separate generators |
|
|
|
What is constructive interference? |
– two superimposed waves of the same frequency (exactly aligned) |
|
|
|
What is destructive interference? |
– two superimposed waves of different frequencies (out of sync) |
|
|
|
Full field or amplitude summation IFC characteristics |
– frequencies of both currents are equal |
|
|
|
Frequency difference IFC characteristics |
– the frequency of the two currents differs |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/9/1/51819145_m.jpg |
|
|
Contrast frequency difference IFC with scan off and scan on
|
With scan off and scan on |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/9/1/51819196_m.jpg |
|
|
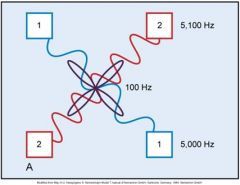
What is the carrier frequency? Which is it in the picture? |
it is the base frequency of the unit before modification (the slower/lower of the two currents when they differ) |
|
|
|
Advantages of IFC |
– medium frequency decreases skin impedance more effectively |
|
|
|
What are the indications for IFC? |
– pain
– inflammation – muscle spasm – edema |
|
|
|
What are the contraindications for IFC? |
same as for other ES: |
|
|
|
How many electrodes are required for true IFC? |
four |
|
|
|
Which tissue is more excitable, nerve or muscle? |
nerve |
|
|
|
Which tissue has higher capacitance, nerve or muscle? |
muscle
|
|
|
|
What is an action potential? |
– sequence of depolarization and repolarization of nerve (or muscle) in response to stimuli |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/3/2/51823008_m.jpg |
|
|
What happens when nerve or muscle cell depolarizes? |
– the cell at rest has a negative charge and there is a high concentration of sodium outside its membrane |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/3/2/51823098_m.jpg |
|
|
What is habituation |
the CNS process of filtering out a continuous non-meaningful stimulus |
|
|
|
What is accommodation |
when the nerve's rate of depolarization decreases while the electric current remains unchanged |
|
|
|
Indication for Iontophoresis |
Acute or Chronic Inflammation Arthritis Myositis ossificans as a means to deliver local anesthetic |
|
|
|
Iontophoresis Medication Dosage |
- measured in terms of milliamperes/minute - based on the relationship between amperage of the current and treatment duration
current amperage (mA)x treatment duration (min)= Ma*MIN |
|
|
|
Iontophoresis Meds and indications |
- Dexamethosone and Lidocaine: Inflammation & pain control - Lidocaine & epinephrine: pain control - acetic acid: heterotopic ossification |
|
|
|
Microcurrent Electrical Stimulation |
- uses monophasic, biphasic, DC or AC - intensity below depolarization threshold of sensory nerves - current produced is about 1/1000 amps of TENS |
|
|
|
Contrast natural physiologcial contraction (NPC) of muscle with an ES contraction (ESC) of muscle. *** |
NPC |
|
|
|
ES can be used to facilitate action potential in: |
– sensory nerves |
|
|
|
What is the relationship between strength and duration of ES application? |
– they are inversely proportional
– the stronger the current, the shorter duration needed |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/4/2/51824173_m.jpg |
|
|
What is rheobase? |
– the intensity of amplitude, with long duration stimulus, required to produce an action potential |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/4/2/51824281_m.jpg |
|
|
What is chronaxie? |
– the duration of ES application required to stimulate tissue at 2X rheobase (amplitude) |
//fce-study.netdna-ssl.com/images/upload-flashcards/back/4/2/51824282_m.jpg
|
|
|
Indications for NMES? |
– decreased strength and endurance |
|
|
|
How is NMES used to treat decreased strength and endurance? |
in conjunction with active exercise
|
|
|
|
How is NMES used to treat decreased ROM? |
– to stimulate muscle groups that can increase ROM |
|
|
|
How is NMES used post injury or surgery? |
– assist in initiating movement in a muscle or muscle group |
|
|
|
How is NMES used to treat muscle spasms? |
– the involuntary contractions may fatigue the muscle and allow it to rest |
|
|
|
How is NMES used for edema reduction? |
– contractions can help pump fluid from the area |
|
|
|
How is NMES used for orthotic substitution and FES? |
– ambulation assistance––(e.g., attachment with heel switch to counter foot drop) |
|
|
|
Rehab post nerve injury (dennervated muscle) is more specifically referred to as: |
EMS
|
|
|
|
What factors need to be considered when using NMES for rehabilitation? |
– how to apply |
|
|
|
What three variations of electrode setup can be used with NMES? |
– monopolar |
|
|
|
What should be considered in electrode placement with NMES? |
– try to put one electrode on a motor point |
|
|
|
What is a motor point? |
– where the nerve enters the muscle |
|
|
|
High TENS Transcutaneous Electrical Nerve Stimulation |
Intensity: Sensory Pulse Frequency: 60 - 100 pps Pulse Duration: 60 - 100 µsec Mode: Modulated rate Treatment duration: as needed onset of relief: <10 min Duration of relief: minutes to hours |
|
|
|
Low TENS Transcutaneous Electrical Nerve Stimulation |
Intensity: Motor Pulse Frequency: 2 - 4 pps Pulse Duration: 150 - 250 µsec Mode: Modulated burst Treatment duration: 30 min onset of relief: 20 - 40 min Duration of relief: hours |
|
|
|
TENS Electrode Placement Direct Placement |
Electrodes are placed directly on the painful site. The electrical channels run parallel to each other |
|
|
|
Parameters for Russian |
– middle frequency 2500 Hz carrier w/ burst |
|
|
|
Frequency for NMES |
– 5 pps |
|
|
|
Pulse duration/width for NMES |
– generally high (200–400 microsec)
– need to consider comfort |
|
|
|
Voluntary Muscle Contraction |
- small diameter type I fibers (slow twitch) muscle fibers are recruited first - contractions and recruitment are asynchronous to decrease muscle fatigue - Golgi tendon organs protect muscles from too much force production - slow onset of fatigue |
|
|
|
Electrically Induced Contractions |
- large-diameter, fast twitch muscle fibers are recruited first (reversal of voluntary) - contractions and recruitment are synchronous, based on the number of pps - Golgi tendon organs can not override the developing tension within the musculotendinous unit - faster onset of fatigue |
|
|
|
Things to consider for contraction of denervated muscle |
– muscle cannot contract physiologically |
|
|
|
What happens to an injured nerve during the first 14 days or so? |
reaction of degeneration |
|
|
|
How fast can nerve tissue regenerate? |
IF the nerve regenerates, it heals
– approx. 1 mm/day, or – 1 inch/month |
|
|
|
What should the therapist remember to do before changing ES treatment parameters? |
TURN THE INTENSITY DOWN!
|
|
|
|
In what forms may AC be delivered? DC? |
both AC and DC may be delivered either continuously or pulsed |
|
|
|
At what pulse duration/pulse width is DC considered to be continuous? |
if the pulse is >= 1 second |
|
|
|
Which is more comfortable to the patient, AC or DC? |
DC is less comfortable than AC |
|
|
|
By what mechanisms has in vivo/vitro research suggested ES (specifically DC) can assist wound healing? |
– alters cell membrane function |
|
|
|
What is galvanotaxis? |
occurs when charged cells are attracted to an electric field |
|
|
|
Describe the electrical potential difference within the skin. |
the epidermis is negatively charged relative to the dermis |
|
|
|
What happens to the electrical potential difference across the skin when there is a soft tissue injury? |
the wound and adjacent epidermis become positive relative to the uninjured tissue
this electrical potential difference steadily declines over time, returning to normal only after the wound closes ES may accelerate tissue healing by replicating or enhancing this process |
|
|
|
Current of injury
|
– the transcutaneous potential of intact skin can be measured at 40–80 mV, but as soon as a full–thickness incision is made, this disappears so that a voltage gradient forms between the wound and surrounding intact skin (Jaffe & Vanabe, 1984)
– a microcurrent will then flow from the area of higher potential (the intact skin) into the wound so that a current of injury is generated – the voltage peaks immediately after injury and gradually decreases as the wound heals (McGinnis & Vanable, 1986), leading to the concept that current flows may be defective in chronic wounds, and that applying electrical currents to wounds may stimulate healing (Kloth, 1995) |
|
|
|
How can ES (specifically DC) help with wound healing? |
– if barrier is broken, a flow of positive polarity occurs within the wound |
|
|
|
At what stage of healing should negative polarity be used? |
negative polarity (cathode) should be used in the acute stage of healing (3–7 days) |
|
|
|
When should the therapist switch to treatment with positive polarity in wound healing? |
change to positive polarity (anode) in proliferative phase to facilitate epithelial cell migration |
|
|
|
When would the therapist continue with treatment with negative polarity after the acute stage? ***
|
continue with negative polarity (cathode) if infection and/or inflammation present |
|
|
|
What treatment should be used if tissue necrosis without inflammation is noted? |
use positive polarity (anode)
|
|
|
|
What do some other wound treatment protocols suggest? |
alternating polarities every few days |
|
|
|
Protocol for DC wound ES |
– place one electrode in wound |
|
|
|
Cathode |
– negative, usually black
– positive, usually red |
|
|
|
What physiological effects tend to occur under the cathode? |
– sodium combines with water to form sodium hydroxide |
|
|
|
What physiological effects tend to occur under the anode? |
– chloride combines with water to form hydrochloric acid |
|
|
|
What is the other use of DC ES? |
– can be used to treat edema |
|
|
|
What is iontophoresis? |
introduction of ionic substances into the body for therapeutic purposes by use of DC |
|
|
|
Why is iontophoresis used? |
most common uses: |
|
|
|
What forms of medication are used in iontophoresis? |
– aqueous solutions
– ointments – creams |
|
|
|
What are the two most common medications used in iontophoresis, and what are their polarities? |
– Decadron (dexamethasone) – negative (–) |
|
|
|
How deeply do medications delivered by iontophoresis typically penetrate? ***
|
3–20 mm |
|
|
|
What are some other uses for iontophoresis? |
– calcium deposits– acetic acid (–) |
|
|
|
Parameters for iontophoresis delivery |
– current type is most commonly continuous DC |
|
|
|
What are the typical dosages for |
Recommended dosage with a |
|
|
|
How is the 40 mA–min dosage administered with the phoresor unit? |
time X mA |
|
|
|
Electrode configuration for iontophoresis |
– active electrode over pathology |
|
|
|
Which electrode in DC/iontophoresis tends to be a bit more irritating? |
the negative electrode (cathode) |
|
|
|
What can be done to reduce skin irritation with DC/iontophoresis? |
if skin irritation occurs, increase size of negative electrode, regardless of which is active
(because of alkaline reaction) |
|
|
|
What are the contraindications and precautions for iontophoresis? |
besides |
|
|
|
An electrical current is:
|
a flow of charged particles (electrons or ions) |
|
|
|
The effects of electrical currents include:
|
– nerve depolarization |
|
|
|
Most uses of electrical stimulation are based on its ability to depolarize nerves to produce:
|
action potentials
|
|
|
|
An electrically stimulated action potential can affect both:
|
– sensory nerves, producing a pleasant or painful sensation, or |
|
|
|
Sensations produced by electrically stimulated action potentials in sensory nerves can:
|
control pain
|
|
|
|
The muscle contractions produced by electrically stimulated action potentials in motor nerves can:
|
– strengthen muscles,
– increase muscle endurance, – improve function, – assist with joint positioning, – decrease spasticity, – increase circulation, – control pain – reduce edema due to poor circulation or lack of use |
|
|
|
The ionic effects of electrical currents can be used to:
|
– facilitate tissue healing
– control the formation of inflammation–related edema – promote transdermal drug penetration |
|
|
|
What parameters must be considered for application of electrical stimulation?
|
– electrode placement
– waveform – polarity – current amplitude – pulse duration – pulse frequency – on:off times – ramp time – treatment time |
|
|
|
Another term for low–rate TENS
|
acupuncture–like TENS
|
|
|
|
Acupuncture–like or low–rate TENS is used for what type of pain? |
acute or chronic, but mainly chronic |
|
|
|
The anode is the: |
positive electrode |
|
|
|
Burst mode TENS is used for what type of pain?
|
acute or chronic, but mainly chronic |
|
|
|
What is another name for conventional TENS? |
high–rate TENS |
|
|
|
Conventional or high–rate TENS is used for what type of pain? |
acute and chronic, but primarily acute
PD/PW = 50 – 80 microsec (LOW) A = sub–motor, tingling F/R = 100 – 150 cps (HIGH) Time = as needed up to 24 hrs. narrower PD/PW is more comfortable for acute pain |
|
|
|
The cathode is:
|
the negative electrode
|
|
|
|
Charge is:
|
one of the basic properties of matter (which is either neutral, negative, or positive) |
|
|
|
Charge is equal to:
|
current X time |
|
|
|
What is current density? How can it be altered?
|
the amount of current delivered per unit area |
|
|
|
What is electrical current?
|
the movement or flow of charged particles though a conductor in response to an applied electrical field |
|
|
|
What is electrical muscle stimulation (EMS)? |
application of an electrical current directly to muscle to produce a muscle contraction |
|
|
|
What is functional electrical stimulation (FES)?
|
application of an electrical current to produce muscle contractions that are applied during a functional activity |
|
|
|
What is galvanotaxis?
|
the attraction of cells to an electrical charge |
|
|
|
What is the gate control theory?
|
a theory of pain control and modulation that states pain is modulated at the spinal cord level by inhibitory effects of nonnoxious afferent input |
|
|
|
What is impedance?
|
the total frequency–dependent opposition to current flow
noted by Z and measured in Ohms for biological systems, impedance describes the ratio of voltage to current more accurately than resistance because it includes the effects of capacitance and resistance |
|
|
|
What is iontophoresis?
|
the transcutaneous delivery of ions into the body for therapeutic purpose using an electrical current
|
|
|
|
What is a motor point?
|
the place in a muscle where electrical stimulation will produce the greatest contraction with the least amount of electricity
generally located over the middle of the muscle belly |
|
|
|
What is neuromuscular electrical stimulation (NMES)?
|
application of an electrical current to motor nerves to produce contractions of the muscles they innervate
|
|
|
|
What is Ohm's law?
|
a mathematical expression of how voltage, current, and resistance relate where voltage equals current multiplied by resistance |
|
|
|
What is the overload principle?
|
a principle of strengthening muscle that states the greater the load placed on a muscle and the higher force contraction it produces, the more strength that muscle will gain |
|
|
|
What is phase?
|
in pulsed current, the period from when current starts to flow in one direction to when it stops flowing or starts to flow in the other direction |
|
|
|
What is polarity?
|
the charge of an electrode that will be |
|
|
|
What is pulse?
|
in pulsed current, the period when current is flowing in any direction |
|
|
|
What is resistance?
|
a material's opposition to the flow of electrical current |
|
|
|
What is TENS?
|
transcutaneous electrical nerve stimulation |
|
|
|
What is voltage?
|
the force or pressure of electricity |
|
|
|
Voltage is also known as:
|
potential difference
|
|
|
|
What is alternating current?
|
a continuous bidirectional flow of charged particles
AC has equal ion flow in each direction, and thus no pulse charge remains in the tissues most commonly, AC is delivered as a sine wave with AC, when the frequency increases, the cycle duration decreases and when the frequency decreases, the cycle duration increases |
|
|
|
What is medium frequency AC?
|
an AC with a frequency between 1,000 and 10,000 Hz (1–10 kHz)
most medium frequency currents available on clinical units have a frequency of 2500 to 5000 Hz medium frequency AC is rarely used alone therapeutically but two medium frequency ACs of different frequency may be applied together to produce an interferential current |
|
|
|
What is continuous current?
|
a continuous flow of charged particles without interruptions or breaks, a continuous current that goes in one direction only is known as a direct current (DC) |
|
|
|
What is a direct current (DC)?
|
a continuous unidirectional flow of charged particles |
|
|
|
What is interferential current?
|
interferential current is the waveform produced by the interference of two medium frequency (1,000 to 10,000 Hz) sinusoidal ACs of slightly different frequencies |
|
|
|
Why is interferential current thought to be more comfortable?
|
it is proposed that interferential current is more comfortable than other waveforms because it allows a low–amplitude current to be delivered through the skin, where most discomfort is produced, while delivering a higher current amplitude to deeper tissues |
|
|
|
What is premodulated current?
|
an alternating current with a medium frequency and sequentially increasing and decreasing current amplitude, produced with a single circuit and only two electrodes |
|
|
|
What is pulsed current? |
an interrupted flow of charged particles where the current flows in a series of pulses separated by periods when no current flows |
|
|
|
What is monophasic pulsed current?
|
monophasic pulsed currents may be used for any clinical application of electrical stimulation but are most commonly used in tissue healing and acute edema management applications |
|
|
|
What is biphasic pulsed current?
|
a biphasic pulsed current may be symmetrical or asymmetrical, and if asymmetrical, may be balanced or unbalanced |
|
|
|
What is Russian protocol?
|
Russian protocol is a waveform with specific parameters intended for quadriceps muscle strengthening |
|
|
|
What is frequency?
|
the number of cycles or pulses per second
frequency is measured in Hertz (Hz) for cycles or pulses per second (pps) for pulses |
|
|
|
What is the interphase interval (intrapulse interval)?
|
the time between phases of a pulse
|
|
|
|
What is the interpulse interval?
|
the time between pulses
|
|
|
|
What is on:off time?
|
on time is the time during which a train of pulses occurs
off time is the time between trains of pulses when no current flows on and off times are usually only used when electrical stimulation is used to produce muscle contractions during the on time, the muscle contracts, and during the off time it relaxes the off times are needed to reduce muscle fatigue during the stimulation session the sequential on and off times also attempt to mimic the voluntary contract and relax phases of normal physiological exercise the relationship of the on and off time is often expressed as a ratio, for example, if a muscle is stimulated for 10 seconds and then allowed to relax for 50 seconds, this may be written as a 10:50 second on:off time or a 1:5 on:off ratio |
|
|
|
What is phase duration?
|
the duration of one phase of a pulse
phase duration is generally expressed in microseconds (μs = 10 –6 seconds) or milliseconds (ms = 10 –3 seconds) |
|
|
|
What is pulse duration?
|
the time from the beginning of the first phase of a pulse to the end of the last phase of a pulse
pulse duration is generally expressed in microseconds (μs= 10 –6' seconds) |
|
|
|
What is ramp up/ramp down time?
|
the ramp up time is the time it takes for the current amplitude to increase from zero, at the end of the off time, to its maximum amplitude during the on time
a current ramps up by having the amplitude of first few pulses of the on time gradually be sequentially higher than the amplitude of the previous pulse the ramp down time is the time it takes for the current amplitude to decrease from its maximum amplitude during the on time back to zero |
|
|
|
Why is ramp time used?
|
ramping is used to produce a "soft start," allowing patients to become accustomed to the stimulation as it increases to reach motor threshold
the ramp up time is generally included in the on time while the ramp down time is generally included in the off time ramp up and ramp down time are different from rise and decay time; the latter describe the time for the current amplitude to increase and decrease during a phase. |
|
|
|
What is rise time/decay time?
|
rise time is the time it takes for the current to increase from zero to its peak during any one phase
decay time is the time it takes for the current to decrease from its peak level to zero during any one phase note that this is different from ramp up/ramp down time |
|
|
|
What is wavelength?
|
the duration of 1 cycle of AC
a cycle lasts from the time the current departs from the isoelectric line (zero current amplitude) in one direction and then crosses the isoelectric line in the opposite direction to when it returns to the isoelectric line the wavelength of alternating current is similar to the pulse duration of pulsed current |
|
|
|
What is amplitude (intensity)?
|
the magnitude of current or voltage
|
|
|
|
What is amplitude modulation?
|
variation in peak current amplitude over time
|
|
|
|
What is burst mode?
|
a current composed of series of pulses delivered in groups known as bursts
the burst is generally delivered with a preset frequency and duration burst duration is the time from the beginning to the end of the burst the time between bursts is called the interburst interval PD/PW = 200 – 300 microsec (HIGH) A = local motor contraction F/R = 1 – 10 bps (LOW) Time = approx. 30 min. for acute and chronic pain, but primarily chronic because producing a contraction and a long pulse duration would likely be too uncomfortable for acute pain |
|
|
|
What is frequency modulation?
|
variation in the number of pulses or cycles per second delivered
|
|
|
|
What is modulation?
|
any pattern of variation in one or more of the stimulation parameters
modulation is used to limit neural adaptation to an electrical current and may be cyclic or random |
|
|
|
What is phase duration or pulse duration modulation?
|
variation in the phase or pulse duration
|
|
|
|
What is scan?
|
amplitude modulation of an interferential current
amplitude modulation of an interferential current moves the effective field of stimulation, causing the patient to feel the focus of the stimulation in a different location this may allow the clinician to target a specific area in soft tissue. |
|
|
|
What is sweep?
|
the frequency modulation of an interferential current
|
|
|
|
What is accommodation?
|
a transient increase in threshold to nerve excitation
|
|
|
|
What is adaptation?
|
a decrease in the frequency of action potentials and a decrease in the subjective sensation of stimulation that occurs in response to electrical stimulation with unchanging characteristics |
|
|
|
What is accommodation? |
When a stimulus sufficient to cause depolarization of a cell membrane remains unchanged, the resting potential of the membrane rises to above its pre-stimulus level. When the nerves rate of depolarization decreases while the depolarization stimulus remains unchanged. |
|
|
|
What is habituation? |
the CNS process of filtering out a continuous, non-meaningful stimulus. |
|
|
|
What is Sensory level? |
Stimulation depolarizes only sensory nerves. This level is found by increasing the output to the point at which a slight muscle twitch is seen or felt and then decreasing the output intensity by ~10% |
|
|
|
What is motor level? |
Stimulation is an intensity that produces a visible muscle contraction without causing pain. |
|
|
|
Direct Current (Ionto) |
uninterrupted, unidirectional flow of electrons
DC can produce polarity-based changes in the tissue, resulting in ions being moved to and from the area iontophoresis: medication delivery low voltage stimulation |
|
|
|
Alternating Current (Interferential) |
uninterrupted, bidirectional flow of electrons high frequency of the AC decreases skin resistance leading to a more comfortable current Interferential - pain control, muscle contractions Premod - NEMS - muscle contractions |
|
|
|
Pulsed Current (Hi Volt Pulsed) |
Monophasic unidirectional flow of electrons marked by periods of non-current flow
monophasic currents are applied to the body with a known charge under each electrode. The resulting current can depolarize sensory and motor nerves. HI Volt pulsed - muscle contractions, pain control |
|
|
|
Biphasic Symmetrical (NMES) |
each phase is a mirror image of the other the electrode carries equal positive and negative charges there is no residual electrical charge NEMS |

|
|
|
Biphasic Asymmetrical Balanced (TENS) |
the two phases do not match each other the two phases carry equal electrical charges the shape of the pulse allows for greater positive (anodal) or negative (cathodal) effects. Net electrical charge is 0 TENS pain control |
|
|
|
Biphasic Asymmetrical Unbalanced (NmENS) |
the two phases do not carry equal electrical charges the shape of the pulse allows for greater positive (anodal) or negative (cathodal) effects
NEMS |
|
|
|
Excitable Tissues |
Nerves, muscle fibers, cell membranes |
|
|
|
Non-Excitable Tissues |
bones, cartilage, tendons, adipose tissue and ligaments |
|
|
|
Electrode size |
the size of the electrode is inversely proportional to the current density. as the size of the electrode increase the current density decreases |
|
|
|
Muscle fibers and conductivity |
muscle fibers are 4x more conductive when the current flows in the direction of the fibers than when it flows across them |
|
|
|
Bipolar technique |
bipolar technique requires the use of electrodes that are equal or nearly equal in size
if electrode A is placed over a motor point or other hypersensitive area and electrode B is not, the effects of the treatment will be weighted towards electrode A |
|
|
|
Monopolar technique |
this technique involves the use of 2 classifications of electrodes
1. active electrode 2. a dispersive electrode |
|
|
|
Quadrapolar technique |
involves the use of two sets of electrodes, each originating from its own electrical channel this is the concurrent application of two bipolar circuits ex. interferential |
|
|
|
Subsensory level |
stimulation occurs between the point at which the output intensity rises from zero to the point where the patient first receives a discrete electrical sensation |
|
|
|
Sensory level |
stimulation depolarizes only sensory nerves. This level is found by increasing the output to the point at which a slight muscle twitch is seen or felt and then decreasing by intensity 10% |
|
|
|
Motor level |
stimulation is an intensity that produces a visible muscle contraction without causing pain |
|
|
|
Noxious level |
stimulation is current applied at an intensity that stimulates pain fibers |
|
|
|
Voltage vs. Amperage |
Voltage: measures the pressure, or FORCE, of electricity, the force that causes charged particles to move
Amperage (Amps): is a measure of the AMOUNT of electricity used, the rate at which electrical current flows
|
The amps multiplied by the volts gives you the wattage (watts), |
|
|
Interferential Stimulation Pain Control via Gate Mechanism |
Carrier Freq. based on patient comfort Burst Freq: 80 - 150 Hz Sweep: fast Electrode Arrangement: quadrapolar Output Intensity: strong sensory level Treatment duration: 20 - 30 minutes |
|
|
|
Interferential Stimulation Pain Control via Opiate Release |
Carrier Freq. based on patient comfort Burst Freq: 1 - 10 Hz endorphin 80 - 120 Hz enkephalin Sweep: slow Electrode Arrangement: quadrapolar Output Intensity: moderate to strong sensory level Treatment duration: 20 - 30 minutes |
|

