![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
143 Cards in this Set
- Front
- Back
|
The graphic representation of the condition of the client's teeth observed on a specific date
|
Dental charting
|
|
|
The most commonly used forms of dental charting present ____________.
|
anatomic or geometric tooth representations.
|
|
|
Inlays can be ________ or _________. (what materials?)
|
porcelain or gold
|
|
|
Inlays do or do not cover cusps?
|
do NOT
|
|
|
Onlays do or do not cover cusps?
|
DO
|
|
|
Where are inlays and onlays made most of the time?
|
In a lab.
|
|
|
The most congenitally missing teeth in the mouth are the _______ and _______.
|
maxillary laterals and mandibular first premolars
|
|
|
Extra teeth are called _________.
|
Supernumerary
|
|
|
The functional unit of tissues that surrounds and supports the tooth is called _________.
|
the periodontium.
|
|
|
The fibrous connective tissue that surrounds and attaches the roots of teeth to the alveolar bone is called _________.
|
the periodontal ligament.
|
|
|
The periodontal ligament is located where?
|
In the periodontal space between the cementum and the alveolar bone.
|
|
|
The periodontal ligaments is composed of _____ & _______.
|
connective tissue cells and intracellular substance.
|
|
|
The fibers that are inserted into the cementum on one side and the alveolar bone on the other are called _________.
|
Sharpey's Fibers.
|
|
|
In health, the free gingiva is closely __________.
|
adapted to each tooth.
|
|
|
Where does the FG attach?
|
Connects with the attached gingiva at the free gingival groove.
|
|
|
T/F
The free gingival groove is a shallow linear groove that demarcates the free from the detached gingiva. |
False
|
|
|
The shallow linear groove that demarcates the free from the attached gingiva is called __________.
|
the free gingival groove.
|
|
|
Also called the gingival crest, this is the margin of the gingiva, or free margin.
|
Gingival margin
|
|
|
The gingival margin is located _______.
|
the edge of the gingiva nearest the incisal or occlusal surface.
|
|
|
What does the gingival margin mark?
|
The opening of the gingival sulcus.
|
|
|
What marks the opening of the gingival sulcus?
|
The gingival margin.
|
|
|
The crevice or groove between the free gingiva and the tooth is called _______
|
the gingival sulcus.
|
|
|
Boundaries of the gingival sulcus:
Inner:________ Outer:________ Base:_______ |
Inner: Tooth surface
Outer: Sulcular epithelium Base: coronal margin of the attached tissues. |
|
|
The base of the sulcus or pocket is also called the "___________"
|
"Probing depth"
|
|
|
Gingival Sulcus:
Healthy depth of sulcus is ___ and may be only ___mm. Average depth of the healthy sulcus is about ___mm. |
shallow and may only be 0.5 mm
1.8 mm |
|
|
Gingival sulcus fluid (_______fluid, ______ fluid)
Serum-like fluid that seeps from the __________ through the __________ of the ________ or _______. |
Sulcular fluid, cervicular fluid
connective tissue epithelial lining sulcus or pocket |
|
|
The gingival sulcus fluid increases with _______.
|
Inflammation.
|
|
|
Cuff-like band of stratified squamous epithelium that is continuous with the sulcular epithelium and completely encircles the tooth.
|
Junctional Epithelium
|
|
|
The junctional epithelium is widest at the junction with the _________.
|
sulcular epithelium.
|
|
|
The junctional epithelium narrows down to the width of a few cells at the __________.
|
apical end (base of pocket).
|
|
|
The junctional epithelium is
keratinized, or non-keratinized? |
Non-keratinized (not hard)
|
|
|
The junctional epithelium provides a ______ at the base of the sulcus.
|
seal
|
|
|
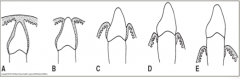
As the tooth erupts, the junctional epithelium attachment is __________.
|
on the enamel.
|
|
|
During eruption,The junctional epithelium migrates towards the __________.
|
CEJ (cementoenamel junction)
|
|
|
At full eruption,The junctional epithelium attachment is on the __________, where it becomes firmly attached.
|
cementum.
|
|
|
When does migration of the junctional epithelium along root surface occur?
|
with periodontal infections or occlusal/incisal trauma.
|
|
|

|
|
|
Junctional Epithelium:
Distance between the base of attachment (pocket) and the crest of the alveolar bone is ____-_____mm. |
1-1.5 mm
|
|
|
Junctional Epithelium:
Distance will be maintained in disease; When a patient loses ______ ______, they will also lose _____. |
gum attachment
bone When you start losing one, you lose the other because they tend to stay equal in relation. |
|
|
Gingiva firmly attached to the underlying bone.
|
Attached gingiva.
|
|
|
Attached gingiva is continuous with the oral epithelium of the __________ gingiva and is covered with _________________.
|
free gingiva
keratinized stratified squamous epithelium |
|
|
Attached gingiva:
Maxillary palatal gingiva is continuous with the ____________ __________. |
palatal mucosa.
|
|
|
_________ Junction: division from attached gingiva and moveable alveolar mucosa.
|
Mucogingival Junction
|
|
|
Mucogingival Junction Location:
Mandibular:_____________ Maxillary:____________ |
Mandibular: facial and lingual gingiva
Maxillary: facial gingiva, not palatal |
|
|
Moveable tissue loosely attached to the underlying bone is called the _____ _______.
|
Alveolar Mucosa
|
|
|
Alveolar Mucosa:
How does the surface look? Keratinized or Non-keratinized? Thin or thick epithelium? |
Smooth and shiny
NONKERATINIZED thin epithelium |
|
|
Is the alveolar mucosa keratinized or non-keratinized?
(possible test question) |
NON-KERATINIZED
|
|
|
Alveolar Mucosa:
_______ _______ may be seen through the epithelium. |
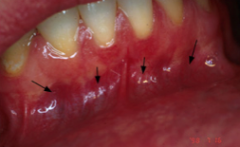
Underlying vessels.
|
|
|
This gingiva that occupies the interproximal area between 2 adjacent teeth.
|
Interdental Gingiva (Papilla)
|
|
|
An interproximal area is also called ________.
|
an embrasure
|
|
|
Type 1 Embrasure:
|
the gingival tissue fills the area.
|
|
|
Type 2 embrasure:
|
there is a slight to moderate recession of the interdental gingiva.
|
|
|
Type 3 embrasure:
|
There is extensive recession or complete loss of the papilla.
|
|
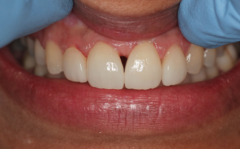
What type of embrasure is this?
|
Type 3
|
|
|
Interdental Gingiva shape:
Varies because of ______ or ______ of the teeth. |
spacing or overlapping.
|
|
|
Interdental Gingiva shape:
Between anterior teeth: ________, ________. |
pointed, pyramidal.
|
|
|
Interdental Gingiva shape:
Between posterior teeth: Flatter than ___________ because of wider teeth, wider _______ , and flattened _______ ________. |
anterior papillae
contacts interdental bone. |
|
|
Interdental Gingiva:
The depression between the lingual or palatal and facial papillae that conforms to the proximal contact area. |
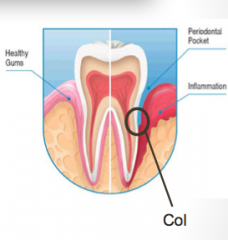
Col
|
|
|
The center of the col area is not usually _______ and thus is more susceptible to infection.
|
keratinized
|
|
|
Most ________ infection begins in the col area.
|
periodontal
|
|
|
Characteristics of clinically healthy gingiva:
(5) |

|
|
|
Gingival tissue discription: Descriptive terminology:
Severity: ____ Distribution: ~Localized: ______ ~Generalized:______ ~Marginal:_______ ~Diffuse:______ |

|
|
|
Gingival Tissue Description: Changes in Disease:
-Color change: _______ -Free gingiva: ______ or ______ -Interdental Papillae: ______, _____, _____, ______. _Festoon (McCall's festoon) (definition on next slide) |

|
|
|
An enlargement of the marginal gingiva with the formation of a lifesaver-like gingival prominence.
Frequently, the total gingiva is very narrow, with associated apparent recession. |
Festoon (McCall's festoon)
|
|
|
Interdental Gingiva: Changes in disease:
2 Types of clefts: 1. ____ A localized recession may be V-shaped or form a slit-like indentation. |
"Stillman's cleft"
|
|
|
2. _____ cleft: created by incorrect floss positioning. Appears as a vertical linear or V-shaped fissure in the marginal gingiva.
|
Floss cleft
|
|
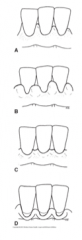
Interdental Papilla descriptions
|

|
|
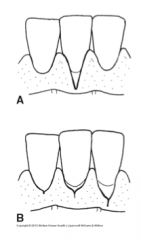
Cleft descriptions
|

|
|
|
Probe Depth: Probe Design
Working end? Cross section shape? Calibrated with ____ marking. Working end and shank meet in defined angle that is usually greater than ______ degrees. |
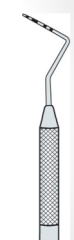
Blunt, rod-shaped working end
Circular or rectangular mm 90 degrees |
|
|
Probe depth functions:
(9) |

|
|
|
Probe Depth: Manual Probes:
Can be made of what? What shape is working end? |
Stainless steel or plastic
Straight or curved. |
|
|
Paired furcation probes have a smooth, rounded end for investigation of the topography and anatomy around ________________.
Ex of probe used __________ |
roots in furca
Nabers |
|

|

|
|
|
Probe depth: Periodontal Pocket:
Tooth is surrounded by a sulcus: The distance from the __________ margin to the coronal-most part of the ___________ epithelium. |
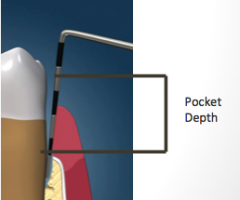
gingival margin
junctional epithelium |
|
|
Probe depth: Periodontal Pocket
Healthy sulcus is generally accepted: ___-___ mm. |
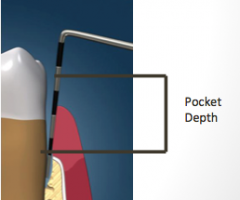
1-3
|
|
|
Pocket Characteristics:
Measured from _________(top of the attached periodontal tissue) to the ________. |
base of the pocket to the gingival margin.
|
|
|
Pocket Characteristics:
Measurement: over ___mm = not considered health or normal. |
3
|
|
|
Pocket Characteristics:
__________: where periodontal infections begin frequently. Probe needs to be placed in the ____ region for accurate measurement. |
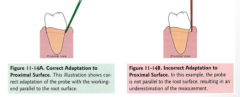
Col or contact area
col |
|
|
Pocket Characteristics:
Anatomic features influence: ____(4)____ |
concavities
anomalies furcation involvement |
|
|
Probing Depth Measurement:
Which 6 areas per tooth? One reading per area-if depths vary, which one do you take? MM measurements; do we round UP or DOWN? |
DF, F, MF, DL, L, ML
DEEPEST UP |
|
|
The distance in mm from the gingival margin to the base of the sulcus or periodontal pocket as measured with a calibrated probe is defined as _________.
|
Probing Depth
|
|
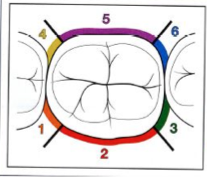
Measurement areas for 6 areas per tooth
|

|
|
|
Once a probe is inserted into a perio pocket, the working-end is kept _________.
|
parallel to the root surface.
|
|
|
Should you use pressure with a probing stroke?
|
NO
|
|
|
Probe insertion:
_______ slide the probe under the gingival margin. Healthy or firm fibrotic tissue makes insertion more difficult because gingival fibers are _______. |
GENTLY
Strong and tight. |
|
|
Insertion easy when the gingival margin is loose and flabby due to __________.
______ can be expected. |
destruction of underlying gingival fibers.
BOP (bleeding on probing) |
|
|
Circumferential Probing: Walking stroke:
Is it necessary to remove probe and reinsert to make readings? |
NO
|
|
|
Circumferential Probing: Walking stroke:
Slide probe up about ____mm and back down again to base of attachment. |
1-2 mm
|
|
|
Circumferential Probing: Walking stroke:
Should cover how much of the circumference of the sulcus or pocket base? |
the entire
|
|
|
Circumferential Probing: Walking stroke:
Is the junctional epithelium at a uniform depth from the gingival margin? |
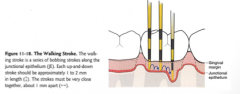
not necessarily
|
|
|
__________ are a series of bobbing strokes made within the sulcus or pocket.
|
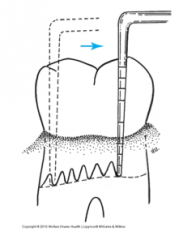
Walking strokes
|
|
|
Recession & Hyperplasia
Normal gingiva position: at the level of, or slightly below, the ________ or prominence of the _________ of a tooth. |
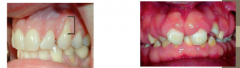
enamel contour
cervical third |
|
|
Recession & Hyperplasia-Changes in Disease
Enlargement: gingival margin may be _________. |
high on the enamel, partly or nearly covering the tooth.
|
|
|
Recession & Hyperplasia-Changes in Disease
Recession: _____. Measured from ____. |
the exposure of the root surface. Measured from the gingival margin to CEJ.
|
|
|
Space apical to root trunk between 2+ roots is called _________.
|
Furcation
|
|
|
Area of multi-rooted tooth from CEJ to entrance of the furcation is termed ________
|
Root trunk.
|
|
|
Entrance to a furcation may be as little as ___-___ mm apical to the CEJ.
|
3-4 mm
|
|
|
Health furcation cannot be felt or detected because it is _____________.
|
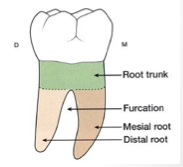
Filled with alveolar bone and PDL fibers.
|
|
|
Furcation anatomic features:
Teeth with 2 roots are labeled ________ Teeth with 3 roots are labeled ________ |
Bifurcation
Trifurcation |
|
|
Furcation involvement:
Loss of ______ and ______ fibers in the space between the roots of a multi-rooted tooth. |
bone and PDL fibers
|
|
|
Furcation involvement:
May be hidden _______. May be visible if _______ is present. Use of furcation probe (_________): to examine furcation's. |
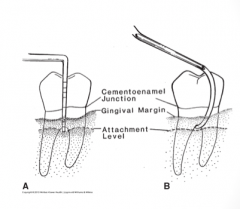
under gingival tissues
recession. NABERS |
|
|
Mandibular molars:
How many roots? Where are the furcations? |
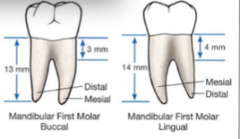
2 roots with furcations on the facial and lingual surfaces between the mesial and distal roots.
|
|
|
Maxillary first premolars:
Ones that are bifurcated have a ___ and ____ root. When bifurcated, the roots separate many mm apical to the ______. |
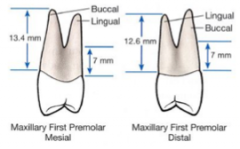
buccal and palatal root.
CEJ |
|
|
Maxillary Molars:
How many roots? Which roots? |
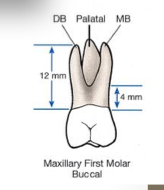
usually trifurcated (3 roots)
MB, DB, and palatal (lingual) roots. (Photo is Buccal view.) |
|
|
Maxillary molars:
On the mesial surface, the furcation is located more toward the ______ surface. On the distal surface, the furcation is located near ________. |
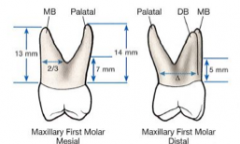
lingual
center |
|
|
Furcation Probes:
N2 is used for assessment of ______ and ______ furcation areas. |
facial and lingual
|
|
|
Furcation Probes:
N1 is used for assessment of ____ and ______ furcation areas. |
mesial and distal
|
|

|
Class I furcation
|
|

|
Class II Furcation
|
|

|
Class III Furcation
|
|

|
Class IV Furcation
|
|
|
CAL (clinical attachment level):
What position does the CAL refer to? |
The position of the periodontal attached tissues at the base of a sulcus or pocket.
|
|
|
CAL (clinical attachment level):
Why is this a useful tool? |
Because measurements are made from a fixed point that doesn't change -- the CEJ.
|
|
|
CAL (clinical attachment level):
Probing depth is measured from a ________ point (the crest of the free gingiva) to the ______. |
changeable
attachment Changes due to tissue swelling, overgrowth, and tissue recession. |
|
|
CAL (clinical attachment level):
Provides an estimate of a tooth's _____ and the loss of _______. |
stability
bone support. (probably on quiz) |
|
|
CAL (clinical attachment level):
When recession of the gingival margin is present, the CAL is calculated by ________ the probing depth to the gingival margin level. |
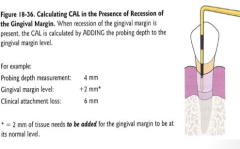
ADDING
|
|
|
CAL (clinical attachment level):
When the gingival margin is excessive to the CEJ, the CAL is calculated by ________ the gingival margin level from the probing depth. |

SUBTRACTING
|
|
|
CAL (clinical attachment level):
When the gingival margin is slightly coronal to the CEJ, no calculations are needed since the probing depth and the clinical attachment level are ______. |
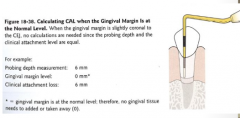
Equal.
|
|

|

|
|
|
Bleeding:
Signs of health: _____ Changes in disease: _____ |
no BOP
Spontaneous or bleeding on probing. |
|
|
Exudate:
Signs of health: ______ Changes in disease: (2) |
none
increased gingival sulcus fluid and presence of exudate. |
|
|
Mobility:
Because of the function of the PDL, teeth have a slight _______ mobility. |
Normal
|
|
|
Mobility:
Can be considered abnormal or pathologic when it ________ normal. |
EXCEEDS
|
|
|
Mobility:
Increased mobility can mean (2) |
perio infection
trauma from occlusion |
|
|
Mobility Examination:
What can interfere with eval of true tooth movement? What fixes this? |
motion of head, lips, or cheek.
Stabilization of head against headrest |
|
|
Mobility Examination:
What type of instruments do you use? What are not recommended? Why? |
2 ended METAL instruments
wooden tongue depressors, plastic mirror handles, fingers are not recommended bc of their flexibility. |
|
|
Mobility Examination:
_________ prevent slipping of the instruments or finger. |
dry teeth
|
|
|
Mobility Examination:
How do we test horizontal mobility? |
Apply the blunt ends of the instruments to opposite sides of a tooth, and then rock the tooth to test.
|
|
|
Mobility Examination:
How do we test vertical mobility? (depression of a tooth into its socket) |
By applying pressure with one of the mirror handles on the occlusal or incisal surface.
|
|
|
Mobility Examination: Record degree of movement
Normal, physiologic |
N
|
|
|
Mobility Examination: Record degree of movement
slight mobility, greater than normal |
1
|
|
|
Mobility Examination: Record degree of movement
moderate mobility, greater than 1 mm displacement |
2
|
|
|
Mobility Examination: Record degree of movement
severe mobility, may move in all directions (vert and horiz) |
3
|
|
|
Radiographic findings (5)
|
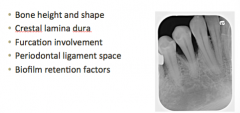
|
|
|
You can ID causative factors of perio disease on an x-ray such as (2)
|
calculus, bone loss
|
|
|
Limitations of radiographic assessment when ID'ing perio disease factors.
(3) |
Soft tissue changes cannot be seen on an x-ray.
Not all perio defects can be seen. 2D picture of 3D object. |
|
|
PA and Vertical BWs are better at seeing _______.
|
Bone levels in bone loss.
|
|
|
Periodontal Classification:
Case Type I: |
Gingivitis
(Generalized 2-3 mm, localized 4mm) No clinical attachment loss (CAL) |
|
|
Periodontal Classification:
Class Type II: |
Early Periodontitis
(Generalized 3-4mm/Heavy Calc) |
|
|
Periodontal Classification:
Class Type III |
Moderate Periodontitis
(Generalized 4-5 mm, localized 6 mm) |
|
|
Periodontal Classification:
Class Type IV |
Advanced Periodontitis
(Generalized 6+ mm) |
|
|
Periodontal Classification:
Case Type V |
Aggressive/Refractory Periodontitis
|
|
|
true or false
relation bt crest of alveolar bone and JE is always maintained |
True
when pt loses gum attachment they will also lose bone |

