![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
12 Cards in this Set
- Front
- Back
|
Clinical Chediak-Higashi
|
|
|
|
Inheritance
|
Autosomal recessive; LYST gene on 1 q42; high consanguinity
|
|
|
Prenatal
|
Fetoscopy fetal hair shafts reveal clumping of melanosomes on light microscopy fetal blood reveals characteristic neutrophilic granules
|
|
|
Incidence
|
Rare; fewer than 100 cases reported; M = F
|
|
|
Age at Presentation
|
Birth to a few months old
|
|
|
Pathogenesis
|
LYST gene mutation codes for a lysosomal tracking protein that regulates microtubules, mediated lysosomal fusion/fission and protein sorting; this defect leads to accumulation of giant lysosomal granules in a variety of cells:
Neutrophils defective phagocytosis, decreased chemotaxis Melanocytes pigmentary dilution Neurons progressive neurologic deterioration Platelet storage pool deficiency bleeding diathesis Decreased natural killer cell and anti body dependent cell mediated cytolysis function |
|
|
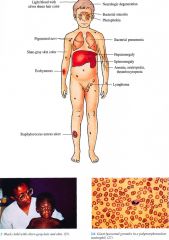
Clinical
|
Skin
Light cream to slate gray color, recurrent bacterial infections Staphylcoccus aureus most common Hair Light blonde color (in caucasians) with a silver sheen Eyes Photophobia, strabismus, nystagmus, decreased uveal pigment Upper and Lower Respiratory Tract Recurrent bacterial sinusitis, pneumonia Central Nervous System Progressive neurologic deterioration with ataxia, muscle weakness, sensory los, seizures (rare) Accelerated Phase (approximately 85% of patients): Hematologic Lymphohistiocytic proliferation with infiltration of liver, spleen, and lymph nodeassociated anemia, neutropenia, thrombocytopenia manifested as petechiae, ecchymoses, gingival bleeding, epistaxis, gastrointestinal hemorrhage, overwhelrning; infection |
|
|
D/Dx
|
OCA2 (p. 58)
Hermansky Pudlak syndrome (p. 60) Chronic granulornatous disease (p. 258) Griscelli syndrome (p. 64) Elejalde syndrome |
|
|
Lab
|
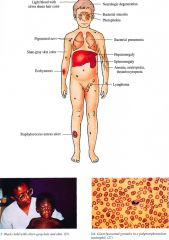
Diagnostic complete blood cell count (CBC) revealing giant granules in neutrophils
|
|
|
Management
|
Referral to pediatric hematologist oncologist bone marrow transplant, chemotherapy, high dose ascorbic acid; Antibiotics, sun protection
Referral to dermatologist, infectious disease specialist, immunologist, neurologist, ophthalmologist |
|
|
Prognosis
|
Death by late childhood from overwhelming infection or hemorrhage during lymphoma like phase; may reverse deterioration with bone marrow transplantation
|
|
|
Clinical Chediak Higashi
|
|

