![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
402 Cards in this Set
- Front
- Back
|
How many breaths per minute should be given during CPR in infants and children?
|
20 breaths/min
|
|
|
What is the first step of fluid resuscitation in a pulseless pediatric patient (volume and type of fluid)?
|
Lactated Ringer or normal saline should be given as a 20mL per kg bolus as quickly as possible
|
|
|
What is the first step in attempting to restore rhythm in a hemodynamically stable pediatric patient with supraventricular tachycardia?
|
Vagal maneuvers
|
|
|
What are examples of "distributive" etiologies of shock?
|
Anaphylaxis
Neurologic injury Drug toxicity |
|
|
What is the best PE finding to use as a determinant of the level of intravascular depletion in a child with suspected shock?
|
Tachycardia - the faster the HR, the more severe the shock
|
|
|
What are important therapies for a pediatric patient with septic shock?
|
Vasopressors
Fluids Antibiotics |
|
|
During which types of poisoning is ipecac administration recommended by the parent at home?
|
None
|
|
|
Name the early symptoms of lead poisoning in a child-
|
Irritability
Hyperactivity Apathy Decreased play Abdominal pain Consipation Vomiting |
|
|
Name the chronic symptoms of lead poisoning in a child-
|
Developmental delay
Behavioral problems Attention disorders |
|
|
In which bronchus are foreign bodies most likely to become lodged in pediatric patients?
|
There is no propensity to lodge in one bronchus or the other, unlike in adults
|
|
|
What item accounts for more than 50% of all foreign body aspirations in children?
|
Nuts
|
|
|
What is the treatment of choice for removing an inhaled foreign body in a child?
|
Rigid bronchoscopy
|
|
|
What are the top three causes of injury in children?
|
1. Motor vehicle accidents
2. Drowning 3. Burns |
|
|
What type of intracranial hemorrhage is associated with shaken baby syndrome?
|
Subdural hemorrhage with diffuse axonal injury and retinal hemorrhages
Falls do not cause these injuries |
|
|
Which genetic syndromes are often associated with heart disease associated with pathologic murmurs?
|
Turner
Down Williams Noonan DiGeorge |
|
|
What is acrocyanosis?
|
Blueness of the distal extremities only- caused by peripheral vasoconstriction and not central cyanosis
|
|
|
Irregularities in which four body systems can cause cyanosis in the newborns?
|
Cardiac
Pulmonary Hematologic Neurologic |
|
|
What additional cardiac malformation is almost always present in Truncus Arteriosus?
|
VSD
|
|
|
Which congenital heart malformation is suggested by a characteristic "egg-shaped" heart silhouette?
|
Transposition of the great vessels
|
|
|
What drug should be administered right away in a patient with transposition of the great vessels?
|
PGE1 administration to maintain a patent ductus arteriosus
|
|
|
50% of patients with 22q11 microdeletions have which congenital cardiac malformation?
|
Tetralogy of Fallot
|
|
|
How does the CXR appear in an infant with Tetralogy of Fallot?
|
The size is generally normal but it may be "boot shaped"
|
|
|
What type of drug is atomoxetine and what pediatric condition is it useful for?
|
A highly specific norepinephrine reuptake inhibitor that is used in childhood ADHD. It is not a stimulant and has few side effects and low abuse potential
|
|
|
Describe the typical rash associated with measles-
|
An erythematous maculopapular rash that erupts on the head and spreads caudally lasting 4 to 5 days
|
|
|
How does the rash of Roseola infantum typically present?
|
Maculopapular rash that appears on the trunk and spreads peripherally on the third or fourth day of illness
|
|
|
Where does the varicella (chicken-pox) virus lay dormant in the body?
|
The dorsal root ganglion
|
|
|
What is the differential diagnosis for diaper rash?
|
Atopic dermatitis
Primary irritant dermatitis Candida albicans infection (if it lasts over four days) |
|
|
What are treatment options for psoriasis?
|
Tar preparations
Natural sunlight (UV-B) Fluorinated steroids |
|
|
What causes erythema multiforme?
|
A hypersensitivity reaction that follows viral infection, mycoplasma infection, drugs (sulfas), immunizations, or food reactions.
|
|
|
Describe the clinical course of Stevens-Johnson's syndrome-
|
Prodrome of up to 14 days of fever, malaise, myalgias, arthralgias, arthritis, emesis and diarrhea.
Followed by sudden onset of high fever and erythema multiforme and bullae on mucus membranes |
|
|
What is the typical presentation of Type I DM?
|
New onset weight loss, polydipsia, polyphagia, polyuria
|
|
|
What is the treatment for Diabetes insipidus?
|
Desmopressin acetate (DDAVP), an ADH analogue given intranasally, subcutaneously or orally.
|
|
|
What might give rise to central diabetes insipidus?
|
Head trauma
Brain trauma CNS infection |
|
|
Are children with precocious puberty typically taller, shorter, or the same height when they reach adulthood?
|
There is initial accelerated growth, but subsequent short stature compared to genetic potential
|
|
|
What endocrine abnormalities are in the diagnosis for short stature?
|
GH deficiency
Primary hypothyroidism Cushing disease |
|
|
What are typical signs of hyperthyroidism in children?
|
Voracious appetite
Heat intolerance Emotional lability Poor sleep Exophthalmos is uncommon in children |
|
|
How is neonatal Graves disease usually treated?
|
It generally resolves on its own over the first several months of life. It is untreated as long as the infant stays hemodynamically stable
|
|
|
What causes neonatal Grave's disease?
|
Transplacental passage of materal thyroid stimulating antibodies
|
|
|
Are males or females more likely to have genital anomalies in 21 hydroxylase deficiency?
|
Female infants are born with ambiguous genitalia - clitoromegaly and labioscrotal fusion but internal structures are normal.
|
|
|
How does a male infant with 21-hydroxylase deficiency present?
|
Genitalia are normal
Emesis, salt wasting, dehydration and shock develop in the first 2-4 weeks of life. Hyponatremia and hyperkalemia result from lack of aldosterone |
|
|
How is 21-hydroxylase deficiency diagnosed?
|
Elevated serum levels of 17-hydroxyprogesterone
|
|
|
What are the clinical signs of 11-hydroxylase deficiency?
|
Hypernatremia, hypokalemia and hypertension due to excess mineralocorticoid activity
|
|
|
Precocious puberty is defined as appearance of secondary sex characteristics before what ages in boys and girls?
|
Boys - <9yo
Girls - <7.5yo |
|
|
What is the most common cuase of precocious puberty in boys?
|
Tumors of the CNS
|
|
|
What is the most common cause of Cushing syndrome in children?
|
Microadenoma of the pituitary resulting in ACTH oversecretion. Tumors of the adrenal gland are rare.
|
|
|
How many mEq of potassium should be added to each liter of maintenance fluids for children?
|
20mEq/L
|
|
|
What is the typical maintenance fluid for children?
|
One fourth normal saline with 5%dextrose and 20mEq KCl
|
|
|
In a dehydrated infant, what clinical signs should you check on the skin?
|
Capillary refill
Mucus membranes Skin turgor Fontanelle |
|
|
What percentage of weight loss can you assume in a patient with
Mild dehydration? Moderate dehydration? Severe dehydration? |
Mild - <5%
Mod - 5-10% Severe - >10% |
|
|
What needs to be checked before administering potassium in a pediatric patient receiving rehydration or maintenance fluids?
|
Urine status.
If a patient is not passing urine, they should not receive potassium |
|
|
What's the most common cause of an abnormally high potassium level on a blood chemistry reading in children?
|
Artifactual because of hemolysis of red blood cells during sample collection
|
|
|
What are treatment options for pediatric patients with hyperkalemia?
|
Calcium gluconate
Sodium bicarbonate Cation exchange resins Hemodyalysis |
|
|
What are the most common causes of hypokalemia in children?
|
Alkalosis secondary to vomiting
Loop diuretics (furosemide) diabetic ketoacidosis |
|
|
How do you calculate anion gap, and what range is considered normal?
|
Na + K - Cl - HCO3 = AG
12 plus/minus 4 is considered normal |
|
|
What are the two most common causes of normal anion gap acidosis in children?
|
Diarrhea
RTA |
|
|
At what age is the onset of symptoms of pyloric stenosis most commonly seen?
|
Peak incidence at 2-4 weeks of life
|
|
|
What is the therapy for most infants with GER?
|
Small, frequent feedings in the upright position
Thickening feeds with rice cereal Maintenance of prone head-up position for at least 20 minutes after feeding |
|
|
Should you feed infants with diarrhea due to gastroenteritis?
|
Yes, continue feedings
Maybe give smaller, more frequent feeds |
|
|
Should anti-diarrheal medication be given to infants with acute diarrhea?
|
No. Antidiarrheal medications are contraindicated because they may cause toxic megacolon
|
|
|
What is the difference between constipation and obstipation?
|
Constipation - infrequent passage of hard, dry stools
Obstipation - absence of bowel movements |
|
|
What is the treatment of anal fissures in children?
|
Soften stools
Keep rectum clean Apply petroleum jelly locally |
|
|
What is the treatment for Hirschsprung disease?
|
First, a diverting colostomy is created surgically. Later, the aganglionic segment is removed and the proximal segment is pulled through the rectum.
|
|
|
How much of the intravascular volume must be depleted in a child to register a drop in blood pressure?
|
40%
|
|
|
Is rectal bleeding more common in Crohn Disease or UC?
|
UC
|
|
|
Is perianal involvement more common in Crohn Disease or UC?
|
Crohn Disease
|
|
|
Are granulomas more common in Crohn Disease or UC?
|
Crohn Disease
|
|
|
What fetal abnormalities can be caused by the teratogen valproate?
|
Spina bifida
|
|
|
What fetal abnormalities can be caused by the teratogen warfarin?
|
Hypoplastic nasal bridge
Chondrodysplasia punctata |
|
|
What is the rate of Down syndrome to mothers over the age of 45?
|
1 in 50
|
|
|
What anomalies of the hand are seen in Down syndrome infants?
|
Single palmar crease
Short, broad hands Incurved fifth finger Hypoplastic middle phalynx |
|
|
What percentage of fetuses with Turner syndrome (XO) come to term?
|
2%
98% die in utero |
|
|
Which chromosome is involved in Prader Willi and Angelmann syndrome?
|
Ch 15
|
|
|
If a fetus inherits two paternal copies of chromosome 15, will it develop Prader Willi or Angelmann syndrome?
|
Angelmann
|
|
|
What is the genetic anomaly that leads to Fragile X syndrome?
|
Over 200 CGG repeats in the FMR-1 gene on the X chromosome
|
|
|
What anomalies are seen in the 22q11.2 deletion syndrome?
|
Cardiac - tetralogy of Fallot, interrupted aortic arch, vascular rings
Absent thymus Hypocalcemic hypoparathyroidism T-cell mediated immunodeficiency Palate abnormalities |
|
|
What is the most common genetic error of carbohydrate metabolism?
|
Galactosemia
|
|
|
What are common clinical manifestations of galactosemia?
|
Liver failure (Hepatomegaly)
Renal dysfunction (acidosis) Emesis Anorexia Poor growth Cataracts |
|
|
What are typical manifestations of glycogen storage diseases?
|
Growth failure
Hepatomegaly Fasting hypoglycemia |
|
|
Which disease manifests as children with Marfan-like bodies, dislocated eye lenses, mild to moderate mental retardation and vascular thromboses?
|
Homocystinuria
Screening tests for elevated methionine in the blood |
|
|
What is the first therapy to try in children with homocystinuria?
|
High doses of pyridoxine. 50% of patients respond to this therapy
|
|
|
What pediatric disease may present with a Erlenmeyer flask shaped distal femur?
|
Gaucher's disease
|
|
|
What molecule accumulates in Gaucher disease?
|
Glucocerebroside
|
|
|
At what age is "physiologic anemia of infancy" most pronounced?
|
2-3 months of age in term infants
6 weeks in the premature infant |
|
|
Name five microcytic anemias-
|
Iron deficiency
Severe lead poisoning Thalassemias Sideroblastic anemia Chronic disease |
|
|
Are most anemias of chronic disease micro, normo, or macrocytic?
|
75% are normocytic
25% are microcytic |
|
|
What are some of the signs of an infant with severe anemia (<3mg/dL)?
|
Signs of CHF
Tachycardia, an S3, cardiomegaly, hepatomegaly, distended neck veins, pulmonary rales |
|
|
What should be the next step when treating a child with presumed iron deficiency anemia who does not respond to iron therapy?
|
Suspect thalassemia - hemoglobin electrophoresis
|
|
|
What is the name for congenital macrocytic pure red cell aplasia?
|
Diamond Blackfan's syndrome
|
|
|
What is the most common cause of normocytic anemia with elevated reticulocyte count?
|
Hemolytic anemia
|
|
|
At what age do children with sickle cell anemia first start showing symptoms?
|
At around 4 months when hemoglobin F diminishes
|
|
|
What neurologic sequelae often present with vitamin B12 deficiency?
|
Paresthesias, peripheral neuropathies
In more severe cases - dementia, ataxia, posterior column degeneration |
|
|
What is the first treatment for significant bleeding due to ITP?
|
High-dose steroids, IV Ig and anti-D globulin
Chronic ITP is treated with splenectomy and/or IV Ig |
|
|
What is the treatment for DIC to stop the bleeding?
|
Platelets and fresh frozen plasma, in addition to treating the underlying cause
|
|
|
Which is prolonged in Hemophilia A - PT or PTT? What about in Hemophilia B?
|
In both Hemophilia A and B, PTT is prolonged but PT is normal
|
|
|
What drug is used as initial therapy to stop bleeding in patients with Hemophilia A?
|
DDAVP
|
|
|
What is the normal function of Von Willebrand factor?
|
It's an adhesive protein that connects collagen to activated platelets and also binds to circulating factor VIII
|
|
|
What are the clinical signs of Von Willebrand disease?
|
Mucocutaneous bleeding
Epistaxis Gingival bleeding Cutaneous bruising Menorrhagia |
|
|
Is PT or PTT (or both) prolonged in vitamin K deficiency?
|
Both are prolonged
|
|
|
At what age of infancy is there an immunologic nadir resulting in the highest rate of infections?
|
6-12 weeks, when maternally derived antibodies are decreasing and the infant immune system is just growing in production
|
|
|
What is the most common presenting complaint of an infant with DiGeorge syndrome?
|
They usually present with complaints unrelated to the immune system like congenital heart disease or hypocalcemic tetany due to thymic hypoplasia
|
|
|
What disease is tested for by the nitroblue tetrazolium test and the dihydrorhodamine reduction test?
|
Chronic Granulomatous Disease
a disorder of phagocytic immunity |
|
|
What prophylactic treatment should patients with Chronic Granulomatous Disease recieve?
|
Prophylactic TMP-SMX and interferon gamma therapy
|
|
|
Is heavy exposure to animal dander early in life a risk factor for allergy, or is it protective?
|
It appears to reduce the risk of atopic disease
|
|
|
What are the treatment options for allergic rhinitis?
|
Allergin avoidance
H1 blockers Nasal topical steroids |
|
|
What is the difference between Urticaria and Angioedema?
|
Urticaria - edematous hives on the skin that itch, blanch and resolve within hours or days
Angioedema - Confined to the lower dermis, a well demarcated area of swelling without pruritis, erythema or warmth. |
|
|
What four organs are typically involved in Henoch Schonlein Purpura?
|
GI tract, skin, joints, kidneys
|
|
|
The diagnosis of Kawasaki disease is based on fever for 5+ days and four out of which of the following clinical signs?
|
1. Bilateral conjunctivitis
2. Changes of lips and oral cavity (dry, red, fissures) 3. Erythema or edema of hands and feet 4. Polymorphous rash 5. Acute, nonpurulent swelling of cervical lymph node |
|
|
What is required to diagnose "Fever of Unknown Origin?"
|
Fever for over 14 days with documented temperature over 38.3 (101F) on multiple occasions and an uncertain etiology
|
|
|
What is the definition of sepsis?
|
Bacteremia with evidence of a systemic response (tachypnea, tachycardia etc)
|
|
|
What percentage of AOM are caused by viruses alone?
|
20%
|
|
|
What are the three most common bacterial pathogens causing AOM?
|
S pneumonia
H influenza M catarrhalis |
|
|
What are risk factors for AOM?
|
Caretaker smoking
Bottle feeding Day care attendance Allergic disease Craniofacial anomalies Immunodeficiency Pacifier use |
|
|
What is the recommended first line therapy for AOM?
|
High dose amoxicillin
If the patient has received ABs in the last month, second line therapy includes amoxicillin/clavulanic acid, or second or third generation cephalosporins |
|
|
What antibiotics are given for herpangina?
|
None, it is a self limiting viral disease
|
|
|
What is the AB therapy for documented group A streptococcal pharyngitis?
|
10 day course of oral penicillin. Macrolides are alternatives for those allergic to penicillins
|
|
|
What may happen if pharyngitis due to EBV is treated with amoxicillin or ampicillin?
|
Patients are more likely to develop a rash as a part of their syndrome
|
|
|
What is the treatment for severe stridor caused by croup?
|
Steroids and nebulized epinephrine
|
|
|
What are the three phases of pertussis?
|
Catarrhal phase - 7-10 day incubation with low grade fever, cough, coryza
Paroxysmal phase - intense coughing spasms Convalescent phase - cough may last for 2-8 additional weeks |
|
|
What is the treatment for pertussis?
|
Erythromycin They shorten the disease only if given early in the catarrhal stage, but should be given for 14 days regardless to decrease the period of infectivity
|
|
|
What is the typical presentation of atypical pneumonia?
|
Fever, headache, pneumonia, myalgia which lasts for 5-7 days followed by a cough that lasts for 2 weeks or more
|
|
|
What is the antibiotic of choice for pneumonia caused by S. pneumonia?
|
Amoxicillin/clavulanic acid
|
|
|
What is the antibiotic of choice for atypical pneumonia?
|
Erythromycin, clarithromycin or azithromycin
|
|
|
Which infectious agent causes the majority of pneumonias with large pleural effusions?
|
S. aureus
|
|
|
Children with suspected bacterial meningitis should be treated with which antibiotics?
|
Vancomycin plus a 3rd gen cephalosporin
|
|
|
What is the antibiotic of choice for treating Shigella?
|
TMP-SMX
|
|
|
What is the treatment for bacterial vaginosis?
|
A single oral dose of metronidazole effectively cures the infection
|
|
|
What is the risk of HIV transmission from a seropositive mother to her fetus without treatment?
|
About 25%
Falls to 2% with proper treatment |
|
|
What is the recommended therapy to avoid transmitting HIV from mother to fetus/infant?
|
The mother should receive antiretroviral therapy starting at week 14. The newborn should also receive AZT for the first 6 weeks of life and should not breast feed
|
|
|
What is the treatment of choice for Rocky Mountain Spotted Fever?
|
Doxycycline
|
|
|
What is the treatment for Lyme disease in children under 8yo? Over 8yo?
|
Under 8 - oral amoxicillin or cefuroxime
Over 8 - doxycycline |
|
|
What was the infant mortality rate in the US in 2000?
|
6.9 per 1,000 live births
|
|
|
What are the five criteria for Apgar scoring?
|
Heart Rate
Respiratory effort Color Muscle tone Reflex irritability |
|
|
How is fractured clavicle due to vaginal delivery usually discovered?
|
A callus is detected at 3-6 weeks of age. Fracture occurs in 2-3% of vaginal deliveries. No treatment is necessary
|
|
|
What qualifies as a "Low Birth Weight" infant?
"Very Low Birth Weight" infant? |
LBW - less than 2500g
VLBW - less than 1500g |
|
|
What are the clinical manifestations of congenital toxoplasmosis?
|
Microcephaly
Hydrocephaly Microphthalmia Chorioretinitis Intracranial calcifications Seizures |
|
|
What infection should you suspect in an infant with retinitis and intracranial calcifications? What treatment is indicated?
|
CMV infection
Treatment for several weeks with ganciclovir |
|
|
What is the antibiotic treatment of choice for neonatal sepsis?
|
10-14 days of ampicillin and gentamicin
|
|
|
What organisms are most responsible for neonatal sepsis in the first 3 days?
|
GBS
E coli Klebsiella Listeria |
|
|
At what day postpartum is neonatal conjunctivitis likely to present?
|
One week to several weeks postpartum
|
|
|
What is the proper treatment for chlamydial conjunctivitis or pneumonia?
|
Oral erythromycin for 14 days
|
|
|
What is the typical CXR pattern for RDS?
|
A uniform reticulonodular or ground-glass pattern and air bronchograms
|
|
|
What is the conventional therapy for RDS?
|
Respiratory support with oxygen and CPAP. Artificial surfactant can also be administered.
|
|
|
What may trigger premature passage of meconium during the peripartum period?
|
Fetal hypoxia/asphyxia
|
|
|
How many hours/days postpartum is the typical peak of physiologic jaundice of the newborn?
|
3-5 days of life, with a peak bilirubin of 12-15mg/dL
|
|
|
Name two bilirubin metabolism disorders that result in unconjugated hyperbilirubinemia-
|
Gilbert's
Crigler-Najjar |
|
|
Name two bilirubin metabolism disorders that result in Direct hyperbilirubinemia-
|
Dubin-Johnson
Rotor |
|
|
What is the treatment of NEC?
|
Feeds should be discontinued and an NG tube inserted for decompression. Antibiotics should be started and feeding given via TPN.
|
|
|
What is the source of most bleeding in preterm infants with intraventricular hemorrhage (IVH)?
|
Bleeding of the germinal matrix - an area of immature vasculature that is the site of pluripotent cells that migrate to form neurons and glia
|
|
|
Blood levels of which chemicals should be checked to evaluate neonates with seizures?
|
Glucose
Sodium Calcium and Mg Ammonia |
|
|
What is the primary anticonvulsant used to manage neonatal seizures?
|
Phenobarbital
|
|
|
On which side of the abdomen are most congenital diaphragmatic hernias found?
|
90% are on the left
|
|
|
What genetic syndrome do 10% of neonates with omphalocele have?
|
Beckwith-Wiedemann's syndrome
|
|
|
What are the typical symptoms of Beckwith-Wiedemann's syndrome?
|
Exophthalmos, macroglossia, omphalocele, gigantism, hyperinsulinemia, hypoglycemia
|
|
|
How is omphalocele treated?
|
The sac should be wrapped with gauze to support the viscera, but no attempt should be made to reduce the sac. Broad spectrum antibiotics should be given. Definitive reduction by surgery can be delayed.
|
|
|
What is the primary difference between omphalocele and gastroschisis?
|
There is a hernial sac covering the viscera in omphalocele. Gastroschisis contains no sac- the intestine is herniated through the abdominal wall lateral to the umbilicus.
|
|
|
When are cleft lips typically repaired? Cleft palates?
|
Cleft lips are repaired shortly after birth. Cleft palates are repaired at 12-24 months of age.
|
|
|
What is the name for pearly white or pale yellow epidermal cysts found on the nose, chin and forehead of neonates?
|
Milia
|
|
|
What common rash consists of papules, vesicles and pustules that usually occur on the trunk of a newborn 24-72 hours after birth?
|
Erythema toxicum neonatorum. Occurs in 50% of newborns. It resolves in 3-5 days without therapy
|
|
|
What rash appears as an erythematous, dry, scaling lesion appearing between weeks 2-10 of life and is sometimes called "cradle cap" when it appears on the scalp?
|
Seborrheic dermatitis
|
|
|
What is the facial appearance of an infant with Fetal Alcohol Syndrome?
|
Micrognathia, a flattened philtrum, short palpebral fissures, a thin upper lip
|
|
|
What diagnostic test is used to detect abnormalities of ureteral insertion sites?
|
A voiding cystourethrogram (VCUG)
|
|
|
What is the most common cause of chronic renal failure in childhood?
|
Posterior urethral valves - occur only in males
|
|
|
If you hear that an infant was diagnosed with "posterior uretheral valves," where are those valves located?
|
In the prostatic urethra. It occurs only in males and is the most common cause of chronic renal failure in childhood.
|
|
|
What is the most common clinical presentation of vesicoureteral reflux?
|
Recurrent UTIs. Can also lead to pyelonephritis and hydronephrosis
|
|
|
At what age is surgery indicated for cryptorchidism?
|
Spontaneous descent after 12 months is rare, so surgery (orhiopexy) is indicated at 12-18 months
|
|
|
What is the underlying cause of varicocle?
|
Absence of venous valves causes dilated testicular vein and enlarged pampiniform plexus
|
|
|
What is the most common site of bacterial infection in a febrile infant?
|
UTI
|
|
|
What diagnostic screening is indicated in a child <24months with suspected cystitis?
|
Renal ultrasound to evaluate for hydronephrosis
|
|
|
What is the most common mechanism for infection of the urinary tract in infants?
|
Hematogenous seeding, as opposed to contamination from fecal flora in adults and older children
|
|
|
What are the clinical signs of nephrotic syndrome in children?
|
Periorbital edema is usually the first abnormality noted. Also, lower extremity and generalized edema and ascites.
|
|
|
When is renal biopsy indicated for diagnosing nephrotic syndrome?
|
In nephrotic syndrome that does not respond to steroid therapy.
|
|
|
Does treating a streptococcal infection reduce the risk of developing post-strep glomerulonephritis?
|
No
|
|
|
What is the underlying mechanism that causes both renal damage and hearing loss in Alport syndrome?
|
It's a mutation in type IV collagen which is important for the glomerular basement membrane and the cochlea
|
|
|
Are chloride levels increased or decreased in the RTA disorders?
|
There is hyperchloremic metabolic acidosis in all types of RTA.
|
|
|
What is the most common cause of acute renal failure in childhood?
|
Hemolytic uremic syndrome (HUS)
|
|
|
What pharmacologic agent might be helpful in reducing the severity of hydrocephalus?
|
Acetazolamide - decreases CSF production
|
|
|
What is the name of a partial seizure that begins as rhythmic twitching in one extremity that marches proximally until the entire limb is involved?
|
Jacksonian seizure
|
|
|
What drug is often given during status epilepticus to break the seizure?
|
IV or rectal short acting benzodiazepine like lorazepam or diazepam
|
|
|
The Cushing triad (bradycardia, hypertension, Cheyne-Stokes respirations) are the hallmark of which pathology?
|
Increased intracranial pressure
|
|
|
What is the most common cause of intracranial hemorrhage in the pediatric population?
|
Congenital vascular abnormalities like AVMs
|
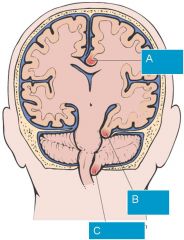
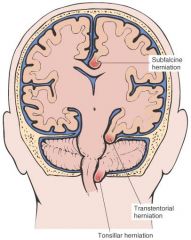
|
|
In what pediatric subpopulation is pseudotumor cerebri most common?
|
Overweight adolescent females or in association with tetracycline or corticosteroid use
Thought to be caused by impaired CSF reabsorption |
|
|
What dangerous pathologies are important to rule out in a pediatric patient with a new onset headache?
|
Tumors,
intracranial bleeds, acute hydrocephalus, meningitis |
|
|
What are possible therapies for a patient with Myasthenia Gravis?
|
Anticholinesterase therapy
Corticosteroids/immunosuppressants Thymectomy |
|
|
What pediatric disease presents with hypertrophied calves?
|
Duchenne muscular dystrophy
|
|
|
What is the leading cause of death in patients with Friedreich ataxia?
|
Cardiomyopathy related heart disease before the age of 30.
|
|
|
What is the best brain imaging study for a child with ataxia?
|
MRI is preferable to head CT given its superior detail of posterior fossa structures
|
|
|
What are Phakomatoses?
|
Neurocutaneous diseases characterized by lesions in the nervous system, skin and eyes, like:
Neurofibromatosis Tuberous sclerosis von Hippel-Lindau disease |
|
|
What is the hallmark of type 2 neurofibromatosis?
|
Bilateral acoustic neuromas
|
|
|
What is the most common finding that leads to the diagnosis of neurofibromatosis type 1?
|
Cafe-au-lait spots (six or more)
|
|
|
What are typical skin lesions found in patients with tuberous sclerosis?
|
Ash leaf spots (flat hypopigmented macules)
Shagreen patches (areas of abnormal skin thickening) |
|
|
What are the major clinical findings in Sturge-Weber disease?
|
port-wine stain over the region of the first division of the trigeminal nerve.
Also - mental retardation, seizures, hemiparesis, visual impairment |
|
|
By what factor do infants increase in length in the first year? Weight?
|
Length - double in the first year
Weight - triple in the first year |
|
|
At what age should iron-fortified cereals be introduced to the infant diet?
|
4-6 months
|
|
|
At what age can cow's milk be introduced into a child's diet?
|
At 12 months whole milk can be given, and you can switch to skim at 24 months
|
|
|
What are contraindications to breast-feeding?
|
Maternal HIV infection or active TB
Mothers on street drugs Infants with galactosemia Maternal use of antithyroid medication, lithium, chemotherapy and isoniazid |
|
|
What is the clinical definition of failure to thrive?
|
Persistent weight below the 3rd percentile, or falling off previously established growth curve
|
|
|
What percent of all pediatric cancer is cancer of the CNS?
|
23%
|
|
|
What genetic syndromes predispose a patient to ALL and AML?
|
Trisomy 21
Bloom Fanconi anemia Ataxia telangiectasia |
|
|
Describe the age distribution of Hodgkin's disease-
|
It has a bimodal distribution - with peaks between 15-30 years and again after the age of 50.
|
|
|
How do patients with supratentorial tumors present compared with infratentorial tumors?
|
Supratentorial - signs of elevated ICP or seizures
Infratentorial - deficits of balance or brainstem function - ataxia, cranial nerve dysfunction |
|
|
Where do neuroblastomas arise?
|
The postganglionic sympathetic nervous system - usually in the abdomen, especially in the adrenal medulla
|
|
|
Which age and gender is Ewing sarcoma most prevalent in?
|
Ewing sarcoma is seen primarily in adolescents and is 1.5 times more common in males
|
|
|
At which parts of the long bone does Ewing sarcoma tend to arise? What about osteogenic sarcoma?
|
Ewing - midshaft
OS - metaphyseal portion |
|
|
Which bones are most commonly involved with Ewing sarcoma?
|
Femur (20%)
Pelvis (20%) Fibula (12%) Humerus and tibia (10% each) |
|
|
Which cancer of the bone is visualized as a radial "sunburst" pattern of periosteal inflammation on radiograph?
|
Osteogenic sarcoma
|
|
|
Is systemic spread more common in Ewing sarcoma or osteogenic sarcoma?
|
More common in Ewing sarcoma - rare in osteogenic sarcoma
|
|
|
What is leukocoria?
|
Absence of the red reflex in an eye
|
|
|
What is the differential diagnosis for lack of red reflex in an eye?
|
Retinoblastoma
Cataracts Retinopathy of prematurity Glaucoma |
|
|
What is the most common cause of ophthalmia neonatorum in the first 24 hours of life?
|
Chemical irritation (birth trauma, antibiotic prophylaxis)
|
|
|
What is the name for the disease defined as avascular necrosis of the femoral head?
|
Legg-Calve-Perthes disease
Usually occurs between ages of 4-8 |
|
|
What is the stereotypical patient who develops slipped capital femoral epiphysis?
|
An overweight patient during puberty
|
|
|
What is the name of a bone fracture when a force breaks one side of a bone and bends the other?
|
Greenstick fracture
|
|
|
What is the duration of antibiotic therapy for osteomyelitis?
|
4-6 weeks of borad spectrum anti-staphylococcal agents
|
|
|
What injury classically results in subluxation of the radial head?
|
A sudden strong jerking of the child's pronated hand resulting in rapid extension at the elbow
|
|
|
What is the differential diagnosis for an infant presenting with wheezing and respiratory distress?
|
Bronchiolitis, foreign body aspiration, GER, TE fistula
|
|
|
What does the disappearance of wheezing in an asthmatic child in respiratory distress represent?
|
Increased obstruction rather than improvement of the condition
|
|
|
How long after administration of inhaled corticosteroids does the effect take place for an asthmatic patient?
|
4-6 hours
|
|
|
What is the difference between puberty and adolescence?
|
Puberty is the physical changes, and adolescence encompasses the physical changes as well as the cognitive, social and psychological changes
|
|
|
What abnormal cardiac finding is present in many patients with anorexia nervosa?
|
30-40% of patients have a cardiac murmur consistent with mitral valve prolapse
|
|
|
What drug may be given to a patient who has severe agitation due to high marijuana use?
|
Benzodiazepines
|
|
|
What is the leading cause of death in the adolescent population?
|
Traumatic injury
|
|
|
What should you suspect if you see brief tremors of the arms and legs after birth?
|
Nothing, they are common for the first four days after birth.
|
|
|
Is the Denver Developmental Screening Test more sensitive or specific in screening for developmental delay?
|
Highly specific, but not too sensitive, so many children with mild developmental delay score as normal
|
|
|
What may cause small head size in an infant?
|
Premature closure of the sutures or microcephaly. Microcephaly can be caused by chromosomal abnormalities, congenital infections, maternal metabolic disorders or neurologic insults
|
|
|
What may cause large head size in an infant?
|
Hydrocephalus, subdural hematoma, brain tumor, or inherited syndromes
|
|
|
What is the average heart rate for an infant 0-2 months old?
|
140
Range of 90-190 |
|
|
What is the average heart rate for an infant 3-6 months old?
|
130
Range of 80-180 |
|
|
What is the average heart rate for an infant 6-12 months old?
|
115
Range of 75-155 |
|
|
What are the three best places to obtain an accurate pulse in an infant?
|
Femoral arteries
Brachial arteries Auscultating heart (or umbilical artery in a newborn) |
|
|
Where is the best place to look for central cyanosis in an infant?
|
Tongue and oral mucosa, not nail beds or extremities
|
|
|
What pathology is suggested by finding multiple light-brown skin lesions with smooth borders?
|
Cafe-au-lait spots (coast of California version)
Suggets neurofibromatosis |
|
|
What is the most common cause of jaundice in the first 24 hours of life?
|
Hemolytic disease of the newborn
|
|
|
How much of a newborn's body weight does the head account for?
|
One-third
|
|
|
When does the posterior fontanelle typically close?
|
2 months
|
|
|
How large is the anterior fontanelle typically at birth?
|
4-6 cm in diameter
|
|
|
What pathology may be suspected by an enlarged posterior fontanelle at birth?
|
Congenital Hypothyroidism
|
|
|
What is the name for pliable, springy cranial bones (like a ping pong ball)?
|
Craniotabes
|
|
|
What pathologies are suggested by pliable, springy cranial bones in infancy
|
Hydrocephaly, rickets, congenital syphilis
|
|
|
What is the name for small white dots in the iris, and what pathology does it suggest?
|
Brushfield spots
They strongly suggest Down syndrome |
|
|
How do you test for choanal atresia in the newborn physical exam?
|
Occlude each nostril one at a time and see if the newborn can breath through the other
|
|
|
What pathology is suggested by the triad of hypoglycemia, macroglossia and omphalocele?
|
Beckwith-Wiedemann syndrome
|
|
|
What should you suspect if you see "Thoracoabdominal paradox" (the inward movement of the chest and outward movement of the abdomen during inspiration) in a newborn?
|
Nothing, it is normal in preterm and newborn infants
|
|
|
What is the most common dysrhythmia in children?
|
Paroxysmal supraventricular tachycardia (PSVT)
|
|
|
Do male or female infants tend to have larger liver spans?
|
Females tend to have slightly larger livers on average
|
|
|
In what percent of newborn males can one or both testes not be felt in the inguinal canal or scrotum?
|
3% of neonates
In 2/3 of these, the testes are fully descended by 1 yr |
|
|
What is the most frequent "cause" of an elevated blood pressure measurement in children?
|
An improperly performed exam due to an incorrect cuff size
|
|
|
In children, are blood pressure readings normally higher or lower in the thigh vs. the arm?
|
Usually 10mmHg higher in the thigh. If the reading is equal or lower, suspect coarctation
|
|
|
What is the single best physical exam finding for ruling out pneumonia?
|
Absence of tachypnea
|
|
|
What is the average heart rate of children 1-2 years old?
|
110
Range 70-150 |
|
|
What is the average heart rate of children 2-6 years old?
|
103
Range 68-138 |
|
|
What is the average heart rate of children 6-12 years old?
|
95
Range 65-125 |
|
|
In young children, is the external auditory canal directed forward or backward?
|
Backward in young children (and upward)
|
|
|
What are the signs of acute otitis media in a child?
|
Red, bulging tympanic membrane with a dull or absent light reflex and diminished movement on pneumatic otoscopy
|
|
|
What is the most likely diagnosis for small papules or pustules appearing on the second day of life in a newborn?
|
Erythema toxicum - a benign lesion that may last a few weeks
|
|
|
What is the best way to differentiate a cephalhematoma from a caput succedaneum on physical examination of a newborn?
|
Cephalhematoma is a subperiosteal bleed that does not cross suture lines.
Caput succedaneum does cross suture lines |
|
|
What problems should you be concerned about if you see pre-auricular skin tags or pits on a newborn?
|
Hearing loss and/or genitourinary anomalies
|
|
|
How is congenital torticollis usually treated?
|
With stretching exercise
|
|
|
What is classically seen on chest X ray in a newborn with RDS?
|
Ground glass appearance over the lung fields and air bronchograms
|
|
|
What is the treatment for RDS?
|
Steroids should be given 48 hrs before delivery
Exogenous surfactant can be given O2 and mechanical ventilation after birth, if needed |
|
|
What is the differential diagnosis of dyspnea in a newborn?
|
RDS
Sepsis (GBS) Meconium aspiration Persistant fetal circulation Diaphragmatic hernia Transient tachypnea of the newborn |
|
|
Which is neurotoxic-
Conjugated bilirubin Unconjugated bilirubin Both Or Neither? |
Only unconjugated bilirubin is neurotoxic, although high conjugated bilirubinemia is usually indicative of serious disease states
|
|
|
What is the proper empiric therapy for neonatal sepsis?
|
Ampicillin + 3rd gen cephalosporin
or Ampicillin + aminoglycoside |
|
|
Which TORCHS infection causes cataracts?
|
Rubella
|
|
|
Which TORCHS infection causes meningoencephalitis?
|
Herpes
|
|
|
What are the presenting symptoms of TE fistula?
|
Coughing or choking, especially when feeding.
Polyhydramnios might also be the presenting feature |
|
|
What is the diagnostic test for TE fistula?
|
Inability to pass a catheter into the stomach demonstrated on radiograph
|
|
|
Pneumatosis intestinalis on plain abdominal radiograph is pathognomonic for which neonatal condition?
|
Necrotizing enterocolitis
|
|
|
What is the most common cause of neonatal seizures?
|
Hypoxic-ischemic encephalopathy
|
|
|
What is the risk to the fetus if the mother uses phenobarbital during pregnancy?
|
Vitamin K deficiency
|
|
|
What are the risk factors for need of neonatal resuscitation at birth?
|
Twin gestation
Prematurity Presence of meconium |
|
|
Besides the GI tract, what organ can be damaged by ingestion of cow's milk before the age of 1?
|
Kidneys can be damaged because of the increased solute load of cow's milk
|
|
|
What precaution should be taken in infants and children who primarily drink goat's milk?
|
Folate supplementation
|
|
|
Over what span of time should the deficit be replaced in a patient with...
Isonatremic dehydration? Hyponatremic dehydration? Hypernatremic dehydration? |
Iso/Hyponatremic dehydration - fluid should be replaced over 8-24 hours.
In hypernatremic dehydration, the fluid should be replaced over 48 hours |
|
|
At what age do infants develop a social smile?
|
~6-8 weeks
|
|
|
At what age do infants typically walk alone?
|
15 months
|
|
|
What criteria are necessary for the diagnosis of ADHD?
|
Symptoms must be seen by 7yo
Must last at least 6 months Must occur in more than one setting Must impair function |
|
|
What is meant by secondary enuresis, and what is the most common cause?
|
Bed wetting after the child has previously achieved dryness at night. It is usually secondary to emotional difficulties
|
|
|
How should acetaminophen overdose be treated in a child?
|
Activated charcoal should be given, and N-acetylcysteine given if levels are above 150ug/mL and can be started within 8 hours.
|
|
|
What treatment is given to enhance the excretion of salicylate in an aspirin overdose?
|
Bicarbonate helps to enhance renal excretion. Urine pH should be raised to 7-7.5.
|
|
|
How should a child who has ingested caustic acids or alkalis be treated?
|
Emesis and gastric lavage are contraindicated.
Stomach should be flushed copiously with water and endoscopy should be performed in the first 24 hours |
|
|
What 2 drugs should be administered in the face of an organophosphate toxicity?
|
Atropine
Pralidoxime |
|
|
What substance is the most common cause of death from poisoning in childhood?
|
Iron poisoning
|
|
|
What levels of lead in the blood are considered abnormal and worrisome in a child during a finger stick screen?
|
>10ug/dL
|
|
|
Tricyclic antidepressant overdose cause what EKG abnormalities in children?
|
QRS widening and QT prolongation
|
|
|
What three factors help grade the severity of concussions?
|
Grade I: Just confusion
Grade II: Also amnesia Grade III: Also loss of consciousness |
|
|
Which childhood bone neoplasm has a "sunburst" appearance, and which has an "onion skin" appearance?
|
Osteosarcoma - sunburst
Ewing sarcoma - onion skin |
|
|
Which viral vaccines are live attenuated viruses?
|
MMR
Varicella Yellow Fever |
|
|
At what age do pneumococcal vaccines begin?
|
2 months
|
|
|
Does the varicella vaccine prevent all varicella infections?
|
The vaccine is 100% effective against severe disease, but some breakthrough infections may result in mild disease
|
|
|
What 3 bacteria are most responsible for causing neonatal fever without a focus of infection?
|
GBS
Listeria E coli |
|
|
What noninfectious etiologies should be in the DD for meningitis?
|
Toxins
Malignancy Collagen vascular disease |
|
|
How should a child with an arboviral encephalitis be treated?
|
Supportive care, including seizure control
|
|
|
How soon after onset of symptoms do radiographs show signs of osteomyelitis?
|
10-14 days
|
|
|
What is the best lab test to follow whether or not osteomyelitis is responding to therapy?
|
ESR or CRP
|
|
|
Which antibiotic is indicated for the treatment of Pertussis?
|
Erythromycin - it only shortens the course of disease if given in the catarrhal stage
|
|
|
What is the treatment for Cat Scratch Disease?
|
No treatment is necessary, the lesions usually resolve spontaneously in 2-4 months
|
|
|
How is Lyme disease diagnosed?
|
Antibodies to B. burgdorferi in the serum
|
|
|
What is the other name for Fifth Disease?
|
Erythema infectiosum, caused by parvovirus B19
|
|
|
What is the other name for Rubeola?
|
Measles
|
|
|
What is the other name for Exanthem Subitum?
|
Roseola, caused by HHV-6
|
|
|
What is the other name for Rubella?
|
German Measles
or Three-Day Measles |
|
|
Vitamin A therapy is recommended to some children with which viral rash?
|
Measles
|
|
|
What viral exanthem is often accompanied by retroauricular, posterior cervical and postoccipital lymphadenopathy?
|
Rubella
|
|
|
Can children <8 recieve tetracycline/doxycycline for Rocky Mountain Spotted Fever?
|
Yes, because the tooth discoloration is dose dependent and it's unlikely that they will require multiple courses of the drug.
|
|
|
How is VZV spread?
|
Through respiratory secretions
|
|
|
How does mumps initially present?
|
Fever, headache, muscle pain and malaise.
These symptoms are the prodrome before parotiditis or orchitis |
|
|
Does the orchitis of mumps usually present before or after puberty?
|
After puberty
|
|
|
Besides mumps virus, which other viruses can cause orchitis?
|
HIV infection
CMV Coxsackie virus |
|
|
What can be done to reduce the risk of vertical transfer of HIV from a pregnant woman to her child?
|
Cesarean section
Prenatal, intrapartum and neonatal zidovudine therapy |
|
|
Which will fluoresce under a Wood's lamp:
Tinea corporis Tinea capitis Both Or neither? |
Tinea capitis will
But tinea corporis (ringworm) will not |
|
|
What is the treatment of choice for tinea corporis infection?
|
Griseofulvin
|
|
|
By which age do most children develop 20/20 vision?
|
5 years old
|
|
|
What is a hordeolum?
|
AKA stye
Infection (usually staphylococcal) of the ciliary follicle and glands along the lid margin |
|
|
At what age does teething typically begin?
|
6-8 months
|
|
|
Which viruses can cause AOM?
|
RSV
Rhinovirus Influenza Adenovirus |
|
|
What is the drug of choice of uncomplicated AOM?
|
Amoxicillin
|
|
|
What two bacteria most commonly cause otitis externa (AKA swimmer's ear)?
|
Pseudomonas aeruginosa
S aureus |
|
|
What is used as prevention for otitis externa in frequent swimmers?
|
Instilling dilute alcohol in the ear canal immediately after swimming
|
|
|
What is the treatment of choice for Streptococcal pharyngitis?
|
Penicillin, and amoxicillin is an acceptable alternative
|
|
|
Name 4 complications of Strep pharyngitis-
|
Rheumatic fever
Glomerulonephritis Peritonsillar abscess Retropharyngeal abscess |
|
|
Which disease may present with a sudden onset of high fever, drooling and respiratory distress with a younger patient sitting in a tripod position with the neck hyperextended?
|
Epiglottitis
|
|
|
Why might there be abdominal pain and a palpable liver and spleen in an asthmatic patient?
|
Pain due to excess use of abdominal muscles in breathing, and palpable liver and spleen due to hyperinflation
|
|
|
Which lobe is most commonly atelectatic in asthmatic patients?
|
Right middle lobe
|
|
|
At what age does teething typically begin?
|
6-8 months
|
|
|
Which viruses can cause AOM?
|
RSV
Rhinovirus Influenza Adenovirus |
|
|
What is the drug of choice of uncomplicated AOM?
|
Amoxicillin
|
|
|
What two bacteria most commonly cause otitis externa (AKA swimmer's ear)?
|
Pseudomonas aeruginosa
S aureus |
|
|
What is used as prevention for otitis externa in frequent swimmers?
|
Instilling dilute alcohol in the ear canal immediately after swimming
|
|
|
What is the treatment of choice for Streptococcal pharyngitis?
|
Penicillin, and amoxicillin is an acceptable alternative
|
|
|
Name 4 complications of Strep pharyngitis-
|
Rheumatic fever
Glomerulonephritis Peritonsillar abscess Retropharyngeal abscess |
|
|
Which disease may present with a sudden onset of high fever, drooling and respiratory distress with a younger patient sitting in a tripod position with the neck hyperextended?
|
Epiglottitis
|
|
|
Why might there be abdominal pain and a palpable liver and spleen in an asthmatic patient?
|
Pain due to excess use of abdominal muscles in breathing, and palpable liver and spleen due to hyperinflation
|
|
|
Which lobe is most commonly atelectatic in asthmatic patients?
|
Right middle lobe
|
|
|
At what age does teething typically begin?
|
6-8 months
|
|
|
Which viruses can cause AOM?
|
RSV
Rhinovirus Influenza Adenovirus |
|
|
What is the drug of choice of uncomplicated AOM?
|
Amoxicillin
|
|
|
What two bacteria most commonly cause otitis externa (AKA swimmer's ear)?
|
Pseudomonas aeruginosa
S aureus |
|
|
What is used as prevention for otitis externa in frequent swimmers?
|
Instilling dilute alcohol in the ear canal immediately after swimming
|
|
|
What is the treatment of choice for Streptococcal pharyngitis?
|
Penicillin, and amoxicillin is an acceptable alternative
|
|
|
Name 4 complications of Strep pharyngitis-
|
Rheumatic fever
Glomerulonephritis Peritonsillar abscess Retropharyngeal abscess |
|
|
Which disease may present with a sudden onset of high fever, drooling and respiratory distress with a younger patient sitting in a tripod position with the neck hyperextended?
|
Epiglottitis
|
|
|
Why might there be abdominal pain and a palpable liver and spleen in an asthmatic patient?
|
Pain due to excess use of abdominal muscles in breathing, and palpable liver and spleen due to hyperinflation
|
|
|
Which lobe is most commonly atelectatic in asthmatic patients?
|
Right middle lobe
|
|
|
What is done to prevent exercise induced asthma?
|
Inhalation of B2 agonist immediately before exercise
|
|
|
Which disease can be complicated by infection with Burkholderia cepacia?
|
Cystic fibrosis
Infection with B cepacia may be associated with poor outcomes |
|
|
Apnea is defined as cessation of breathing for at least how long?
|
20 seconds
|
|
|
What is the gold standard for diagnosing Obstructive sleep apnea?
|
Polysomnography - a sleep study test
|
|
|
For what condition might a neonate receive caffiene?
|
Apnea of prematurity
|
|
|
Which respiratory infection classically features a "staccato cough"?
|
Chlamydia trachomatis pneumonia in infants
|
|
|
What is the treatment for chlamydia pneumonia in infants?
|
Erythromycin ethyl succinate drops (EES) by mouth for 14 days
|
|
|
What is the most common presentation of heart failure in infants?
|
Feeding difficulties, or sweating during feeding
|
|
|
Where are VSD murmurs typically heard, and what is their quality?
|
A harsh holosystolic murmur best heard at the left lower sternal border - frequently with a thrill
|
|
|
Is PDA more common in girls, boys, or is it equal?
|
More common in girls 2:1
|
|
|
What is the most common congenital heart disease to present with cyanosis in the first 24 hours?
|
Transposition of the great vessels
|
|
|
What are the five major Jones criteria for diagnosing Acute Rheumatic Fever?
|
Carditis
Polyarthritis Erythema marginatum Chorea Subcutaneous nodules |
|
|
What are some diagnostic tests if pyloric stenosis is suspected?
|
Abdominal ultrasound shows a thickened pylorus
Barium swallow shows a dilated stomach Labs show a hypokalemic, hypochloremic alkalosis |
|
|
What are some extra-intestinal manifestations of Crohn Disease in children?
|
Fever
Arthritis Erythema nodosum Weight Loss Growth retardation |
|
|
What conditions may increase the likelihood of developing intussusception?
|
Lymphoid hyperplasia
Meckel diverticulum Polyps CF HSP Rotavirus vaccine |
|
|
What are the two organs primarily affected by Reye syndrome?
|
Brain - encephalopathy
Liver - Fatty degeneration |
|
|
How does Reye syndrome typically present?
|
Acute onset of vomiting.
Delirium, combative behavior follow Can progress with seizures, coma and death |
|
|
What lab tests are abnormal in Reye syndrome?
|
Ammonia elevated
Liver enzymes elevated CK and LDH elevated Maybe hypoglycemia PTT elongated |
|
|
What are common symptoms of UTIs in infants?
|
Fever
FTT Weight loss Vomiting and diarrhea |
|
|
How should UTI be treated in a neonate?
|
IV ampicillin and gentamycin
|
|
|
Any child under 5 yo requires what diagnostic scan after diagnosis of a UTI?
|
A VCUG (Voiding Cystourethrogram)
Performed to investigate the presence of valves, reflux and diverticula |
|
|
If a VCUG (Voiding Cystourethrogram) shows evidence of reflux, what is the next step?
|
A renal scan with DMSA (Dimercaptosuccinic acid) should be performed to assess for renal scarring
|
|
|
What is the most important therapy for managing children with vesicoureteral reflux?
|
Antibiotic prophylaxis with TMP-SMX
|
|
|
How long after a streptococcal infection does Acute Poststreptococcal Glomerulonephritis present?
|
1-2 weeks
|
|
|
How is Acute Poststreptococcal Glomerulonephritis treated?
|
Antibiotics do not change the course of the disease. Antihypertensive medications should be given if the child develops HTN, and renal failure should be treated if it occurs.
|
|
|
What is the clinical course of Alport syndrome?
|
There is no therapy, and patients develop end-stage renal failure in the 2nd or 3rd decade of life and require dialysis or transplant
|
|
|
How are WBC count, Hb and Platelet count affected in HUS?
|
WBC elevated (~30,000)
Hb decreased (5-9) Platelets decreased (20-100K) |
|
|
What is the primary suspicion when a patient with nephrotic syndrome develops acute abdominal pain?
|
Spontaneous peritonitis
|
|
|
What is the first-line therapy for Juvenile Rheumatoid Arthritis?
|
NSAIDs
Methotrexate is second line Corticosteroids have few indications |
|
|
What is the therapy for Kawasaki disease?
|
IVIG and high dose aspirin
|
|
|
To diagnose DM, what glucose levels should be measured during
Random plasma glucose? Fasting glucose? 2-hr glucose tolerance? |
Random >200
Fasting >126 2hr challenge >200 |
|
|
A 2 month old has decreased muscle tone, a large fontanelle, a large tongue, and an umbilical hernia. What pathology do you suspect?
|
Hypothyroidism
|
|
|
What is often the earliest sign of congenital hypothyroidism?
|
Prolonged jaundice
|
|
|
What is usually the first manifestation of sickle cell disease?
|
Dactylitis around 5-6 months
|
|
|
What is the MCV in Diamond Blackfan Syndrome?
|
A macrocytic anemia
|
|
|
What disease do you suspect in an infant with microcephaly, microphthalmia, hearing loss, hyperpigmentation, and absent radii and thumbs?
|
Fanconi anemia - bone marrow failure
|
|
|
What is usually the first presenting sign of acquired aplastic anemia?
|
Hemorrhage secondary to thrombocytopenia
|
|
|
Patients with which conditions are at an increased risk of ALL?
|
Down syndrome
Ataxia telangiectasia Neurofibromatosis Type I Sideroblastic anemia |
|
|
What is the two most common posterior fossa tumors of childhood?
|
#1 - Cerebellar astrocytoma
#2 - Medulloblastoma |
|
|
What are two common physical exam findings in patients with craniopharyngiomas?
|
Short stature
Visual problems |
|
|
Besides abdominal mass, what are other findings associated with Wilm's tumor?
|
Anomalies of the genitourinary tract
Hemihypertrophy Anirida Hypertension |
|
|
What is the typical EEG finding in patients with Infantile spasms?
|
Hypsarrhythmia - abnormal interictal high amplitude waves and a background of irregular spikes
|
|
|
What is the treatment of choice for infantile spasms?
|
ACTH and prednisone
|
|
|
What is the treatment of choice for absence seizures?
|
Ethosuxamide
|
|
|
In Wilson disease, is serum copper elevated or decreased?
What about ceruloplasmin? What about urine copper concentration? |
Serum copper - decreased
Ceruloplasmin - elevated Urine copper - elevated |
|
|
What drug is the treatment of choice for Wilson disease?
|
D-Penicillamine
|
|
|
What are the medical and surgical treatments for Hydrocephalus?
|
Medical - acetazolamide and furosemide
Surgical - shunt |
|
|
What is the primary pathology in Werdnig-Hoffmann disease?
|
Atrophy of the anterior horn cells in the spinal cord resulting in severe hypotonia
|
|
|
What lab finding is abnormal in the CSF of a patient with Guillain Barre?
|
CSF protein is elevated, and other values are normal
|
|
|
How is the diagnosis of Duchenne Muscular Dystrophy made?
|
Muscle biopsy demonstrates necrosis, fat cells and fibrous tissue
|
|
|
What is the prognosis of Duchenne Muscular Dystrophy?
|
Death usually occurs by 18 years of age from respiratory problems
|
|
|
In which disease do half of children have rhabdomyomas of the heart?
|
Tuberous sclerosis
|
|
|
What are the "tubers" of Tuberous Sclerosis?
|
Periventricular calcified lesions that may be seen on CT scan of the head
|
|
|
What is the average age of menarche in girls?
|
13.5
|
|
A neonate has hypoplasia of the mandibular area including micrognathia, glossoptosis, and a cleft soft palate. This is suggestive of which pathology?
|
Pierre Robin Sequence
|
|
|
Potter Sequence is all caused by which primary lesion?
|
Bilateral renal agenesis
|
|
|
How many drinks per day during pregnancy are typical to cause fetal alcohol syndrome with its characteristic features?
|
8-10 drinks per day
|
|
|
A vertical crease on the earlobe is suggestive of which pathology?
|
Beckwith-Wiedemann Syndrome
|
|
|
What is the triad of Prune Belly Syndrome (Eagle-Barrett Syndrome)?
|
Urinary anomalies
Deficiency of abdominal wall muscles Undescended testes |

