![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
41 Cards in this Set
- Front
- Back
|
Differences between HIV 1 and 2? |
HIV 1 has higher viral loads, accelerated progression
HIV 2 is 5-8x less transmissible, rare vertical transmission, longer latency, slower CD4 decline |
|
|
Diagnosis of HIV depends on... |
positive serology!
ELISA + (screen) and 2 viral protein markers on Western blot (p24, gp41, gp120/160) |
|
|
If a patient has a positive ELISA and 1 viral protein marker for HIV, what is the next step? |
They must have TWO protein markers for HIV to be diagnosed
Test them in 1 month
Several things can give a false positive: OTR, CT disease, pregnancy |
|
|
AIDS criteria? |
positive serology and either:
1. presence of an AIDS defining condition 2. CD4 count <200 (normal CD4 is 500-1500) |
|
|
Basic structure of HIV? |
single stranded RNA virus |
|
|
How does co-infection with HTLV-1 affect CD4 counts? |
Co-infection with HTLV-1 increases IL2 signaling --> this falsely elevates the CD4 count (via nonfunctional CD4 lymphocytes) |
|
|
Why can't we just wipe out CD4 cells and start a persons immune system over to get rid of HIV? |
HIV can be harbored in dendritic cells |
|
|
What is the acute retroviral syndrome? How long does it last? |
Initial replication in lymphatics --> produces a viremia in 2-4 weeks, which correlates with the initial maculopapular exanthem, fever and LAD
this morbiliform eruption lasts for 4-5 days |
|
|
When are antibodies to HIV detectable? |
6-12 weeks after exposure, IgG, IgM, IgA are present and detectable |
|
|
There are tons of AIDS defining conditions... the ones we are concerned about are:
1. fungal infections (coccidio, crypto, histo, candida) 2. active HSV 3. kaposi sarcoma 4. mycobacterial infection
How long does the patient need to have HSV to meet AIDS defining criteria? |
>1month! |
|
|
Side effect of foscarnet? |
genital ulcers |
|
|
Criteria for disseminated zoster? Internal manifestation? |
more than 20 lesions outside of a contiguous dermatome
increased risk of fatal pulmonary VZV |
|
|
Which type of molluscum contagiosum is sexually transmitted? |
MCV2 is sexually transmitted
MCV1 is in kids |
|
|
HAART therapy and HPV?
HAART therapy and HSV? |
HAART therapy does not decrease incidence of progression of HPV, HPV and HIV are both independent risk factors for anal SCC (HIV regulatory protein increases HPV expression)
HAART therapy does decrease incidence of HSV |
|
|
Candidal infections are AIDS defining if located where? |
esophagus, trachea, bronchial
NOT tongue |
|
|
Retinitis d/t CMV is AIDS defining when... |
it is associated with blindness |
|
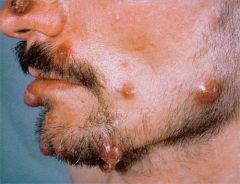
causes? |
Bacillary angiomatosis!!
B. henselae= visceral, cats B. quintana= subcutaneous and osseous, poor living conditions |
|
|
How does syphilis increase risk of HIV? |
increased CCR5 on monocytes at ulcer base increases the transmission of HIV |
|
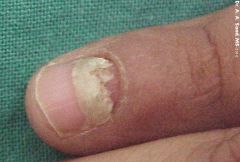
Cause? |
Proximal subungual onychomycosis, t.rubrum
very rare, almost always in HIV patients |
|
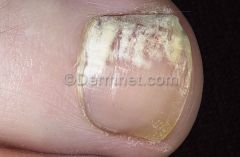
Cause? |
White superficial onychomycosis, t.mentag usually
if t.rubrum, think about HIV |
|
|
Thumb print purpura around the umbilicus in an HIV patient? |
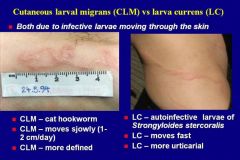
larva currens!!
|
|
|
What is the most common HIV ectoparasite? |
scabies
look in hyponychium, reservoir for recurrence |
|
|
New onset Reiters should always prompt HIV test. Triad? |
conjunctivitis, urethritis, arthritis |
|
|
What is HIV associated follicular syndrome? |
follicular spines acne conglobata hidradenitis suppurativa |
|
|
What is the best treatment for generalized pruritis in HIV? |
nbuvb |
|
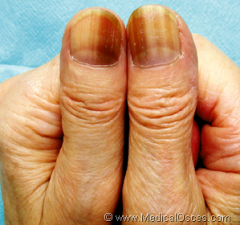
Which HAART therapy is this patient on? |
Zidovudine |
|
|
Zidovudine can cause what cutaneous manifestation? |
increased melanin in nails |
|
|
Indinavir can cause what cutaneous manifestation? |
protease inhibitor
paronychia |
|
|
What is the most common cause of facial lipoatrophy in Caucasians on long term HAART therapy? |

PI > NRTIs > NNRTIs |
|
|
What is the most common cause of visceral obesity in a female on long term HAART therapy? |
Protease inhibitors (protease pouch) |
|
|
Virus associated with Kaposi's sarcoma? Most common internal manifestations? |
HHV8
GI, lymphatics, lung tumors |
|
|
Protocol for all patients on Abacavir is what? |
To have HLA-B*5701 screening --> hypersensitivity syndrome
Abacavir (NRTI) |
|
|
Which HAART therapy is the most common cause of morbiliform drug eruptions? |
NNRTI |
|
|
side effects with Didanosine? |
optic neuritis, peripheral neuropathy, pancreatitis |
|
|
Side effects of protease inhibitors? |
lipodystrophy |
|
|
CYP3A4 interactions:
inhibitors? inducers? |
Inhibitors- protease inhibitors, delaviradine
Inducers- efavirenz, nevirapine (both NNRTI)
This is a big deal bc it can decrease efficacy of birth control... WFT these people shouldn't have sex anyways |
|
|
HAART therapy decreases the incidence of many other infective viruses EXCEPT: |
molluscum
HPV --> HIV Tat (transactivator of transcription) protein, HIV regulartory protein increases HPV expression |
|
|
Treatment for apthaea major in HIV patients? |
thalidomide |
|
|
HIV patients are at a higher risk for cutaneous neoplasms, including... |
BCC:SCC, 6:1
Increased polyoma virus --> increased merkel cell carcinomas |
|
|
HIV patients are at an increased risk for lymphomas, which types? |
non-Hodgkins |
|
|
Side Effects:
Side Effects:
Zidovudine
Didanosine
Stavudine
Lamivudine
Abacavir
Tenofovir |
Zidovudine- melanonychia, mucosal hyperpigmentation
Didanosine- pancreatitis, lactic acidosis
Stavudine- peripheral neuropathy, lactic acidosis
Lamivudine- alopecia
Abacavir- hypersentivitity (HLA B 5701)
Tenofovir- lactic acidosis, morbilloform rash |

