![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
45 Cards in this Set
- Front
- Back
|
Which drug is known to cause scotomas?
dapsone isotretinoin quinacrine chloroquine gold |
chloroquine- irreversible bull's eye maculopathy results in permanent visual field changes if not found early on, in contrast, very few case reports of HCQ ocular toxicity, but it can occur
|
|
|
What antimalarial can cause yellow tears? |
quinacrine |
|
|
What are the antimalarials we use? What are their indications? |
Hydroxychloroquine, chloroquine, quinacrine
Indicated for cutaneous LE, SCLE, dermatomyositis, lichen planus, PCT |
|
|
What is the most feared toxicity of Quinicrine? What about Hydroxychloroquine or chloroquine?
What monitoring do we use? |
The most feared toxicity of quinacrine is BM tox/apalstic anemia, often preceded by a lichenoid rash --> get CBC
The most feared toxicity of hydroxychloroquine or chloroquine is is renal toxicity --> get CMP
Worry about occular toxocity with chloroquine > hydroxychloroquine (quinacrine only causes yellow tears, not retinal tox) --> get baseline eye exam, then if high risk, get annual |
|
|
Raynaud's phenomenon is a potential adverse effect of which chemotherapeutic agent?
5-FU doxorubicin bleomycin vinca alkaloids hydroxyurea
What is the MOA of this drug? |
Bleomycin!!!
inhibits DNA synthesis in infected keratinocytes (induces DNA strand breaks) --> this is why we inject it into therapy resistant verrucae vulgaris; this injection is super PAINFUL :,( |
|
|
Which of the following is not a side effect of bleomycin?
Erythromelalgia Pulmonary fibrosis Flagellate hyperpigmentation Serpentine supravenous hyperpigmentation Acrosclerosis |
Erythromelalgia- YES, pain and burning post injection
Pulmonary fibrosis- YES when used systemically
Flagellate hyperpigmentation- YES, dermatographism too
Serpentine supravenous hyperpigmentation- NO
Acrosclerosis- YES, combination of Raynauds and scleroderma
don't have to monitor any labs with local injection |
|
|
Which antihistamine has suppressor T cell inhibitory activity? |
Cimetidine |
|
|
What do we use cimetidine for? MOA? |
off label uses for acne, hirshitism, androgenetic alopecia, mucocutaneous candidiasis, verruca vulgaris, condyloma acuminata
MOA: antiandrogen, H2 antihistamine, suppressor T cell inhibitory activity |
|
|
56 year old male presents with blue-gray discoloration of his face, ears, and dorsal hands. What is the most likely offending agent?
Minocycline Amiodarone Chloroquine Quinacrine Clofazimine |
Amiodarone |
|
|
56 year old male presents with orange-brown discoloration of his face, ears, and dorsal hands. What is the most likely offending agent?
Minocycline Amiodarone Chloroquine Quinacrine Clofazimine |
Clofazamine- red/brown hyperpigmentation within skin lesions |
|
|
What is the FDA indication for Clofazamine (Lamprene)? MOA? |
Lepromatous leprosy (typically in combo with dapsone and rifampin), PG |
|
|
Patient has a gouty attack and GERD. You treat him appropriately. What do you warn him about? |
Acute gouty flares treated with colchicine when NSAIDS aren't tolerated (GI upset)-- can cause abdominal cramping, hyperperistalsis |
|
|
What are the indications for colchicine? |
gout- when NSAIDs aren't tolerated
familial mediterranean fever- gene defect in MEFV --> recurrent attacks of fever, abdominal pain, pleuritis, pericarditis, scrotal pain, erysipelas
Bechets disease- oral/genital ulcers, silk road in the middle east
Sweets- neutrophilic dermatosis of tender red papules, ppl with AML, RA, IBD
LCV
Calcinosis cutis |
|
|
What is the MOA of podophyllin? |
Lipid-soluble compound that easily crosses cell membranes --> potent cytotoxic agents that inhibit cell mitosis and deoxyribonucleic acid (DNA) synthesis in a manner similar to that of colchicine. Cell division is arrested, and other cellular processes are impaired, gradually resulting in the disruption of cells and erosion of the tissue. |
|
|
MOA of colchicine? |
Antimitotic and anti inflammatory by binding tubulin and preventing microtubular formation
Similar to podophyllin |
|
|
What is the TOC for Wegner's granulomatosis? MOA? |
Cyclophosphamide- alkylating agent that functions in a cell cycle independent fashion |
|
|
This alkylating agent acts in an cell cycle independent fashion... |
Cyclophosphamide |
|
|
What drug causes hemorrhagic cystitis? How is it prevented? |
Cyclophosphamide, prevented with Mesna |
|
|
What are Danazol and Stanazol FDA approved for? MOA? |
FDA approved for treatment of hereditary angioedema, cryofibroginemia, lipodermatosclerosis, livedoid vasculopathy
MOA: anabolic steroid derived from testosterone |
|
|
What are the side effects associated with Danazol and Stanazol? |
Think of Tony Danza and John Stamos!!
Hirsuitism, deepening voice, CHF (so hot they break your heart)
also acne, weight gain, menstrual irregularities, myalgias, insulin resistance |
|
|
Dapsone is used for a patient with dermatitis herpetiformis. Dapsone induces anti-inflammatory effects by primarily inhibiting which type of cell? |
polymorphonuclear leukocytes |
|
|
What medication suppresses the halide-myeloperoxidase system? |
Dapsone (thought to be the MOA in treating DH) |
|
|
What is the MOA of dapsone? |
As antibiotic: blocks dihydropterase synthetase, so bacteria can't make dihydrofolic acid
As anti-inflammatory: inhibits neutrophil respiratory burst by blocking myeloperoxidase from converting hydrogen peroxide into hypochlorus acid |
|
|
Which medication reduces the formation of methemoglobin?
dapsone cimetidine azathioprine cyclosporine rifampin |
cimetidine- remember, methemoglobin is when Fe2+ is oxidized to Fe3+, convernting Hb to metHb, decreasing O2 carrying capacity and inducing hypoxia |
|
|
How does a deficiency in G6PD cause methemoglobinemia? |
decreased G6PD --> decreased NADPH --> decreased reduced glutathione, therefore no reduction of free radicals --> lots of oxidative damage
Too much stress and oxidation --> Fe2+ is oxidized to Fe3+, converting hemoglobin to methemoglobin --> decreased O2 carrying capacity and hypoxia |
|
|
What is dapsone used for? |
TOC for DH, linear IgA, bullous SLE, EED |
|
|
What do we assess neurologically in a patient on dapsone? |
Dapsone/auto zone- peripheral motor neurological function |
|
|
Treatment of choice to acutely lower methemoglobin levels in patients taking dapsone is: |
oral methylene blue (1-2mg/kg IV) |
|
|
What supplement is likely to decrease hemolysis associated with patients taking dapsone? |
Vitamin E!! oral administration of 800 units of vitamin E daily for 4 weeks confers partial protective effect against dapsone-induced hemolysis in patients with dermatitis herpetiformis |
|
|
Finasteride is currently used off label for male and female pattern androgenetic alopecia. What is it's mechanism of action? |
5a reductase inhibitor |
|
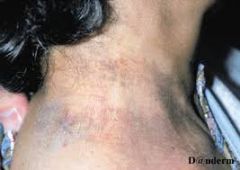
75 year old woman with long history of RA comes in for a progressive 'rash' on her neck that started to appear after she went to the beach. What other dermatologic manifestations should you be concerned about? |
Chrysiasis--- gold deposition in the upper dermis after exposure to UV light. This patient was treated with gold therapy for RA. Other side effects of gold can include:
stomatitis, chelitis, lichen planus-like eruptions, pityriasis rosea like eruptions |
|
|
Psoriasis maintenance therapy that can induce leg ulcers? |
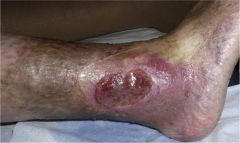
Hydroxyurea can induce leg ulcers |
|
|
MOA of hydroxyurea? |
inhibits M subunit of ribonucleotide reductase, thus blocking DNA synthesis
** in psoriasis, it causes hypomethylation of genes, inducing differentiation and normalization of psoriatic skin |
|
|
This drug is indicated for maintenance therapy for psoriasis and works by inhibiting the M subunit of ribonucleotide reductase |
HYDROXYUREA |
|
|
This drug has an indication for Sjogren-Larsson syndrome. |
Leukotriene inhibitors (monteleukast) |
|
|
What is Sjogren Larsson syndrome? |
inborn error of metabolism resulting in the deficiency of enzyme fatty aldehyde dehydrogenase, which is needed to produce normal oils and fats in the body --> red, dry skin, scaling, PK, itching and scratching, neurological involvement (white dots on retina, abnormal gait, paresis, spasticity, delayed speech)
Sjogren- that guy likes drying out stuff, no oil, no lubey fat in skin or brain |
|
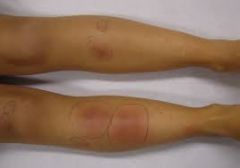
27 year old female on OCP presents with this. Now you put her on a pill, she complains of a brassy taste in her mouth since taking it. |
You put her on SSKI to treat her erythema nodosum. Side effects include goiter, hypothyroidism, brassy taste, parotid enlargement, GI irritation |
|
|
What is the Wolff-Chaikoff effect? |
autoregulatory phenomenon that inhibits organification int he thyroid gland, the formation of thyroid hormones inside the thyroid follicle, and the release of thyroid hormones into the blood stream
WTF?! |
|
|
If a patient has a personal history of breast cancer, what medication can you not use for acne? |
spironolactone |
|
|
Peak vulnerability to thalidomide occurs during what days of gestation? |
If thalidomide is administered during days 21-36 of gestation, 100% chance of birth defect |
|
|
What is the most common adverse effect of thalidomide therapy? |
sedation-- remember this is how it was marketed in the old days... as an anxiolytic |
|
|
What are the differences in neurological side effects between dapsone and thalidomide? |
DAPSONE- motor neuropathy (dapsone, auto Zone cars)
Thalidomide- sensory neuropathy |
|
|
What is Celgene? |
Celgene is thalidomide, marketed as a treatment for multiple myeloma |
|
|
MOA of thalidomide? |
TNF-a inhibitor, decreases neutrophil chemotaxis |
|
|
Neutrophilic eccrine hidradenitis is a side effect of which therpeutic agent? |
CYTARABINE |

