![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
407 Cards in this Set
- Front
- Back
|
Three cell types with regard to cell cycle
|
Permanent, Stable, Labile
|
|
|
Rough Endoplasmic Reticulum rich cells
|
-Mucus-secreting goblet cells of small intestine
-Antibody-secreting plasma cells (ie lost of secretory protein) |
|
|
Cell cycle: Permanent cells
|
Remain in G0. If they regenerate, they regenerate from stem cells.
|
|
|
Cell cycle: Stable cells
|
Enter G1 from G0 when stimulated
|
|
|
Cell cycle: Labile cells
|
Never go to G0, divide rapidly with a short G1
|
|
|
Smooth Endoplasmic Reticulum: Functions
|
-Steroid synthesis
-Detoxification of drugs and poisons |
|
|
Permanent cells: cell types
|
-Neurons
-Skeletal and cardiac muscle -RBCs (regenerate from stem cells) |
|
|
Stable cells: cell types
|
-Hepatocytes
-Lymphocytes |
|
|
Smooth Endoplasmic Reticulum rich cells
|
-Liver hepatocytes
-Steroid hormone-producing cells of the adrenal cortex |
|
|
Labile cells: cell types
|
-Bone marrow
-Gut epithelium -Skin -Hair follicles (think about chemotherapy side effects) |
|
|
Rough Endoplasmic Reticulum: Functions
|
-Synthesis of secretory (exported) proteins
-N-linked oligosaccharide addition to many proteins |
|
|
Neurons: name of Rough Endoplasmic Reticulum and its function
|
Nissl bodies sytnhesize enzymes (eg ChAT) and peptide neurotransmitters.
|
|
|
Golgi apparatus
|
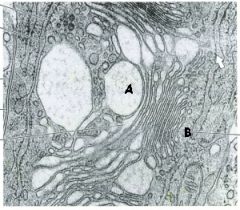
What organelle is this?
|
|
|
6 functions of Golgi apparatus
|
1. Distribution center
--Input: Proteins and lipids from endoplasmic reticulum --Output: Plasma membrane, lysosomes, secretory vesicles 2. Modifies N-oligosaccharides on asparagine 3. Adds O-oligosaccharides to serine and threonine residues (on protein) 4. Addition of mannose-6-phosphate to proteins designated for lysosome 5. Proteoglycan assembly from core proteins 6. Sulfation of sugars in proteoglycans and of selected tyrosine on proteins |
|
|
B
|
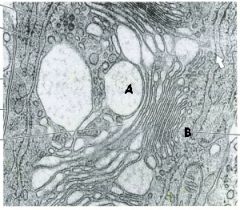
Which letter marks the cis-face?
|
|
|
I-cell disease: Problem
|
In Golgi apparatus, failure to add mannose-6-phosphate to intralysosomal designated proteins leads to their improper export
|
|
|
A
|
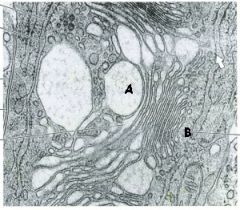
Which letter marks the trans-face?
|
|
|
I-cell disease: Presentation
|
-coarse facial features
-clouded corneas -restricted joint movement -high plasma levels of lysosomal enzymes -fatal in childhood |
|
|
3 types of vesicular trafficking proteins
|
COPI, COPII, and Clathrin
|
|
|
COPI: Function
|
Retrograde Intracellular transport: cis-Golgi to RER
|
|
|
COPII: Function
|
Anterograde Intracellular transport: RER to cis-Golgi
|
|
|
Clathrin: Function
|
Extracellular/lysosomal transport:
-lysosome: trans-Golgi to lysosome -trans-Golgi to plasma membrane to endosomes (for receptor mediated endocytosis) |
|
|
Microtubules: Diameter
|
24 nm
|
|
|
Microtubules: Structure
|
13 dimers of alpha/beta tubulin per circumference (each dimer bound to GTP), repeated in helical configuration
|
|
|
Microtubules: Found in ?
|
-Flagella
-Cilia -Mitotic spindles -Slow neuronal axoplasmic transport |
|
|
Microtubules: Speed of growth and collapse
|
Grows slowly and collapses quickly
|
|
|
Microtubules: Affected by which drugs?
|
-Mebendazole/thiabendazole (antihelminthic)
-Taxol (anti-breast cancer) -Griseofulvin (anti-fungal) -Vincristine/Vinblastine (anti-cancer) -Colchicine (anti-gout) |
|
|
Microtubule polymerization defects: Found in what syndrome
|
Chediak-Higashi syndrome
|
|
|
Chediak-Higashi syndrome
|
Microtubule polymerization defect resulting in decreased phagocytosis
|
|
|
Cilia: Structure
|
-9+2 arrangement of microtubule doublets
-The 9 peripheral doublets are linked by dynein atpase |
|
|
Cilia: Mechanism
|
The 9 peripheral doublets are linked by dynein atpase, which causes bending of cilium by differential sliding of doublets
|
|
|
Molecular motors and direction of transport in cell
|
Dynein: retrograde (DIES back towards nucleus)
Kinesin: anterograde (MOVES kinetically forward) |
|
|
Kartagener's syndrome: Defect
|
Dynein arm defect causing immotile cilia
|
|
|
What is phosphatidylcholine also known as?
|
lecithin
|
|
|
Kartagener's syndrome: Presentation
|
-Male infertility (immotile sperm)
-Female infertility (immotile fallopian cilia) -Bronchiectasis and recurrent sinusitis (bacteria and particles not pushed out) -Situs inversus |
|
|
What syndrome is situs inversus associated with?
|
Kartagener's
|
|
|
Plasma membrane: composition
|
-Cholesterol (~50%)
-Phospholipids (~50%) -Sphingolipids -Glycolipids -Proteins |
|
|
What is lecithin also known as?
|
phosphatidylcholine
|
|
|
Plasma membrane: melting temperature association
|
High cholesterol or long saturated fatty acid content means increased melting temperature
|
|
|
Where is phosphatidylcholine found?
|
Major component of:
1. RBC membranes 2. myelin 3. bile 4. surfactant (DPPC- dipalmitoyl phosphatidylcholine) |
|
|
Drugs that inhibit the sodium-potassium pump
|
-Ouabain
-Cardiac glycosides (digoxin, digitoxin) |
|
|
Ouabain: Mechanism
|
Inhibits Na-K atpase by binding to K site.
|
|
|
What process uses phosphatidylcholine?
|
Esterification of cholesterol with LCAT (lecithin-cholesterol acyltransferase)
|
|
|
Cardiac glycosides: Mechanism
|
Inhibits Na-K atpase, increasing cardiac contractility
|
|
|
True or False: Collagen is not the most abundant protein in the body?
|
False, it is. (25% of all protein in the human body is collagen)
|
|
|
True or False: Collagen is the most abundant protein in the body?
|
True. (25% of all protein in the human body is collagen)
|
|
|
Collagen types and their primary locations
|
Be (So Totally) Cool, Read Books
1. (90% of all collagen) Bone, Skin, Tendon (bONE) 2. Cartilage (carTWOlage) 3. (Reticulin)-blood vessels 4. Basement membrane |
|
|
Collagen Type I locations
|
Be (So Totally) cool, read books
-Bone (bONE) -Skin -Tendon -dentin -fascia -cornea -late wound repair |
|
|
Collagen Type II locations
|
be (so totally) COOL, read books
-Cartilage (carTWOlage) -vitreous body -nucleus pulposus |
|
|
Collagen Type III locations
|
be (so totally) cool, READ books
(Reticulin) -blood vessels -skin -uterus -fetal tissue -granulation tissue |
|
|
Collagen Type IV locations
|
be (so totally) cool, read BOOKS
-basement membrane or basal lamina (four under the floor) |
|
|
Collagen synthesis: list of events and locations
|
Intracellular
1. Synthesis (Rough Endoplasmic Reticulum) 2. Hydroxylation (Endoplasmic Reticulum) 3. Glycosylation (Golgi) 4. Exocytosis Extracellular 5. Proteolytic processing 6. Cross-linking |
|
|
Collagen production step 1: Synthesis
|
-In rough endoplasmic reticulum
-translation of collagen alpha chains (aka preprocollagen) |
|
|
Composition and other name of collagen alpha-chains
|
-Gly-X-Y (where X and Y are proline, hydroxyproline, or hydroxylysine)
-aka preprocollagen |
|
|
Composition and other name of preprocollagen
|
-Gly-X-Y (where X and Y are proline, hydroxyproline, or hydroxylysine)
-aka collagen alpha-chains |
|
|
Collagen production step 2: Hydroxylation
|
-In endoplasmic reticulum
-Hydroxylation of specific proline and lysine residues (using vitamin C) |
|
|
Collagen production step for which vitamin C is required
|
Hydroxylation of Gly-X-Y chains to form hydroxyproline or hydroxylysine
|
|
|
Collagen production step 3: Glycosylation
|
-In Golgi apparatus
-Glycosylation of preprocollagen lysine residues and formation of procollagen (triple helix of three collagen alpha chains) |
|
|
Composition of procollagen
|
Triple helix of three collagen alpha chains (aka three preprocollagen chains)
|
|
|
Osteogenesis Imperfecta: Pathophysiology
|
Cannot take glycosylated alpha-chains and form procollagen (triple helix)
|
|
|
Collagen production step 4: Exocytosis
|
Exocytosis of procollagen
|
|
|
Collagen production step 5: Proteolytic processing
|
Cleavage of terminal regions of procollagen, transforming it into insoluble tropocollagen
|
|
|
Composition of tropocollagen
|
Procollagen (triple-helix) with terminal regions cleaved
|
|
|
Collagen production step 6: Cross-linking
|
Reinforcement of many staggered tropocollagen molecules by covalent lysine-hydroxylysine cross-linkage to make collagen fibrils
|
|
|
Enzyme which performs collagen cross-linking (final step)
|
Lysyl oxidase
|
|
|
Ehlers-Danlos syndrome: Pathophysiology
|
Nonfunctioning lysyl oxidase resulting in lack of collagen fibrils (linked tropocollagen molecules)
|
|
|
Ehlers-Danlos syndrome: Presentation
|
-Hyperextensible skin
-Tendency to bleed/easy bruising -Hypermobile joints |
|
|
Ehlers-Danlos syndrome: # of types
|
10
|
|
|
Ehlers-Danlos syndrome: Inheritance
|
Varies
|
|
|
Ehlers-Danlos syndrome: Most frequently affected collagen type and result
|
Type III collagen resulting in blood vessel instability
|
|
|
Osteogenesis Imperfecta: Types
|
-Abnormal collagen type I (bONE)
--Most common --Autosomal-dominant -Type II --Fatal in utero or neonatal period |
|
|
Osteogenesis Imperfecta: Presentation
|
1. Brittle bone disease: Multiple fractures with minimal trauma (often during birth)
2. Blue sclearae (due to translucency of connective tissue over the choroid) 3. Hearing loss (abnormal middle ear bones) 4. Dental imperfections due to lack of dentition |
|
|
Multiple fractures in a child: Differential Diagnosis
|
-Child abuse
-Osteogenesis Imperfecta |
|
|
Osteogenesis Imperfecta: Incidence
|
1:10,000
|
|
|
Immunohistochemical stain for: Connective tissue
|
Vimentin
|
|
|
Immunohistochemical stain for: Muscle
|
Desmin
|
|
|
Immunohistochemical stain for: Epithelial cells
|
Cytokeratin
|
|
|
Immunohistochemical stain for: Neuroglia
|
GFAP (Glial fibrillary acid proteins)
|
|
|
Immunohistochemical stain for: Neurons
|
Neurofilaments
|
|
|
Vimentin stains for:
|
Connective tissue
|
|
|
Desmin stains for:
|
Muscle
|
|
|
Cytokeratin stains for:
|
Epithelial cells
|
|
|
GFAP (Glial fibrillary acid proteins) stains for:
|
Neuroglia
|
|
|
Neurofilaments stain for:
|
Neurons
|
|
|
Elastin: Description and Location
|
Stretchy protein within lungs, large arteries, elastic ligaments
|
|
|
Elastin and Collagen: Peptide composition difference
|
Both: Proline and lysine rich
Collagen: Hydroxylated forms Elastin: Non-hydroxylated forms |
|
|
Elastin: Structure
|
Tropoelastin with fibrillin scaffolding (fibrillin defect in Marfan's syndrome)
|
|
|
Elastin: Conformations
|
Relaxed and stretched
|
|
|
Elastase: function
|
Break down elastin
|
|
|
Elastase inhibitor
|
alpha-1-antitrypsin
|
|
|
Elastase excess: Found where
|
Found in emphysema
|
|
|
Association of emphysema with elastase
|
Excess elastase activity can cause emphysema
|
|
|
Apoptosis: Characteristics
|
1. Cell shrinkage
2. Chromatin condensation 3. Membrane blebbing 4. Formation of apoptotic bodies which are then phagocytosed |
|
|
Apoptosis: Events which initiate it
|
-Embryogenesis
-Hormone induction (menstruation) -Immune cell-mediated death -Injurious stimuli (eg radiation, hypoxia) -Atrophy |
|
|
Necrosis: Definition
|
Enzymatic degradation of a cell resulting from exogenous injury
|
|
|
Necrosis: Characteristics
|
1. Enzymatic digestion
2. Protein denaturation 3. Release of intracellular components 4. Inflammatory process. |
|
|
Necrosis: Types and where they are found
|
1. Coagulative (heart, liver, kidney)
2. Liquefactive (brain) 3. Caseous (Tuberculosis) 4. Fat (Pancreas) 5. Fibrinoid (blood vessels) 6. Gangrenous (limbs, GI tract) |
|
|
Reversible or irreversible cell injury: Cellular swelling
|
Reversible
|
|
|
Reversible or irreversible cell injury: Nuclear chromatin clumping
|
Reversible
|
|
|
Reversible or irreversible cell injury: Decreased ATP synthesis
|
Reversible
|
|
|
Reversible or irreversible cell injury: Ribosomal detachment
|
Reversible
|
|
|
Reversible or irreversible cell injury: Glycogen depletion
|
Reversible
|
|
|
Reversible or irreversible cell injury: Plasma membrane damage
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Lysosomal rupture
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Calcium influx leading to oxidative phosphorylation
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Nuclear pyknosis
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Karyolysis
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Karyorrhexis
|
Irreversible
|
|
|
Reversible or irreversible cell injury: Mitochondrial permeability
|
Irreversible
|
|
|
Inflammation: Classic signs
|
-Rubor (redness)
-Dolor (pain) -Calor (heat) -Tumor (Swelling) -Functio lassa (Loss of function) |
|
|
Characteristics of Inflammation: Fluid exudation
|
1. Increased vascular permeability
2. Vasodilation 3. Endothelial injury |
|
|
Characteristics of Inflammation: Leukocyte activation
|
1. Emigration
2. Chemotaxis 3. Phagocytosis and killing |
|
|
Characteristics of Inflammation: Fibrosis
|
1. Fibroblast emigration and proliferation
2. Deposition of extracellular material |
|
|
Characteristics of Acute Inflammation
|
Mediated by:
1. Neutrophils 2. Eosinophils 3. Antibodies |
|
|
Characteristics of Chronic Inflammation
|
Mediated by mononuclear cells:
-Characterized by persistant destruction and repair -Granulomas: nodular collections of macrophages and giant cells |
|
|
Characteristics of Inflammation: Resolution
|
1. Restoration of normal structure
2. Granulation tissue 3. Abscess 4. Fistula 5. Scarring |
|
|
Granulation tissue: histologic characteristics
|
-highly vascularized
-fibrotic |
|
|
Abscess: histologic characteristics
|
fibrosis surrounding pus
|
|
|
Fistula: characteristics
|
abnormal communication
|
|
|
Scarring: histologic characteristics
|
Collagen deposition resulting in altered structure and function
|
|
|
Steps in leukocyte emigration
|
1. Rolling
2. Tight binding 3. Diapedisis 4. Migration |
|
|
Leukocyte emigration step characteristics: Rolling
|
Binding between:
-E-selectin on vascular endothelium -Sialyl-LewisX on the leukocyte |
|
|
Leukocyte emigration step characteristics: Tight binding
|
binding between:
-ICAM-1 on vascular endothelium -LFA-1 on leukocyte |
|
|
Leukocyte emigration step characteristics: Diapedesis
|
leukocyte travels between endothelial cells and exits blood vessel
|
|
|
Leukocyte emigration step characteristics: Migration
|
Leukocyte travels through interstitium to the site of injury or infection guided by chemotactic signals
|
|
|
Chemotactic signals
|
1. Bacterial products
2. Complement 3. Chemokines |
|
|
Free radical injury: Initiated by what?
|
1. Radiation exposure
2. Metabolism of drugs (phase I) 3. Redox reactions 4. Nitric oxide 5. Transition metals 6. Leukocyte oxidative burst |
|
|
Free radical injury: Mechanism
|
-Membrane lipid peroxidation
-Protein modification -DNA breakage |
|
|
Free radical injury: Stopped by what?
|
-Spontaneous decay
-Antioxidants --Vitamin E --Vitamin A -Enzymes --Catalase --Superoxide dismutase --Glutathione peroxidase |
|
|
Major cause of injury after thrombolytic therapy
|
Free-radical production induced by reperfusion after anoxia
|
|
|
Hyperplasia: definition
|
reversible increase in number of cells
|
|
|
Metaplasia: definition
|
Reversible substitution of one cell type for another.
|
|
|
Metaplasia: When found?
|
Often secondary to irritation and/or environmental exposure (eg squamous metaplasia in trachea and bronchi of smokers)
|
|
|
Dysplasia: definition
|
Reversible abnormal growth with loss of cellular orientation, shape and size in comparison to normal tissue maturation
|
|
|
Dysplasia: When found?
|
In paraneoplastic syndromes
|
|
|
Anaplasia: definition
|
abnormal cells lacking differentiation, like primitive cells of same tissue.
|
|
|
Anaplasia: When found?
|
Undifferentiated malignancies
|
|
|
Neoplasia: Definition
|
A clonal proliferation of cells that is uncontrolled and excessive
|
|
|
Difference between hyperplasia and dysplasia
|
Can occur together
1. hyperplasia - increase in number 2. dysplasia - abnormal proliferation of cells with loss of size, shape, and orientation |
|
|
Appearance of cancerous cells
|
-High nuclear/cytoplasmic ratio
-Clumped chromatin |
|
|
How does carcinoma invade a basement membrane?
|
-Collagenases
-Hydrolases |
|
|
Seed and soil theory of metastasis
|
Seed: Tumor embolus
Soil: Target organ |
|
|
Tumor grade: definition
|
Degree of cellular differentiation based on histologic appearance of tumor
|
|
|
Tumor stage: definition
|
Degree of localization/spread based on site and size of primary lesion, spread to regional lymph nodes, and presence of metastases
|
|
|
Tumor grade vs stage: Quick characterization
|
grade: character of tumor itself
stage: spread of tumor in a specific patient (Stage=Spread) |
|
|
Tumor grade vs stage: Which has more prognostic value?
|
Stage
|
|
|
TNM staging system
|
Tumor size
Node involvement Metastases |
|
|
Benign tumors of cell type: Blood cells
|
Does not exist. The malignant blood cells are automatically metastasizing.
|
|
|
Benign tumors of cell type: Blood vessels
|
Hemangioma
|
|
|
Benign tumors of cell type: Smooth muscle
|
Leiomyoma
|
|
|
Benign tumors of cell type: Skeletal muscle
|
Rhabdomyoma
|
|
|
Benign tumors of cell type: Bone
|
Osteoma
|
|
|
Benign tumors of cell type: Fat
|
Lipoma
|
|
|
Benign tumors of cell type: >1 cell type
|
Mature teratoma (women)
|
|
|
Benign tumors of cell type: Epithelium
|
-Adenoma
-Papilloma |
|
|
Malignant tumor of cell type: Epithelium
|
-Adenocarcinoma
-Papillary carcinoma |
|
|
Malignant tumor of cell type: Blood cells
|
-Leukemia
-Lymphoma |
|
|
Malignant tumor of cell type: Blood vessels
|
Angiosarcoma
|
|
|
Malignant tumor of cell type: Smooth muscle
|
Leiomyosarcoma
|
|
|
Malignant tumor of cell type: Skeletal muscle
|
Rhabdomyosarcoma
|
|
|
Malignant tumor of cell type: Bone
|
Osteosarcoma
|
|
|
Malignant tumor of cell type: Fat
|
Liposarcoma
|
|
|
Malignant tumor of cell type: >1 cell type
|
Immature teratoma, Mature teratoma (men only)
|
|
|
Name the cell type: Adenoma
|
Epithelium
|
|
|
Name the cell type: Papilloma
|
Epithelium
|
|
|
Name the cell type: Adenocarcinoma
|
Epithelium
|
|
|
Name the cell type: Papillary carcinoma
|
Epithelium
|
|
|
Name the cell type: Leukemia
|
Blood cells
|
|
|
Name the cell type: Lymphoma
|
Blood cells
|
|
|
Name the cell type: Hemangioma
|
Blood vessels
|
|
|
Name the cell type: Angiosarcoma
|
Blood vessels
|
|
|
Name the cell type: Leiomyoma
|
Smooth muscle
|
|
|
Name the cell type: Leiomyosarcoma
|
Smooth muscle
|
|
|
Name the cell type: Rhabdomyoma
|
Skeletal muscle
|
|
|
Name the cell type: Rhabdomyosarcoma
|
Skeletal muscle
|
|
|
Name the cell type: Osteoma
|
Bone
|
|
|
Name the cell type: Osteosarcoma
|
Bone
|
|
|
Name the cell type: Lipoma
|
Fat
|
|
|
Name the cell type: Liposarcoma
|
Fat
|
|
|
Name the cell type: Teratoma
|
>1 cell type
|
|
|
Neoplasm associated with: Down syndrome
|
ALL (we ALL fall Down), AML
|
|
|
Neoplasm associated with: Xeroderma pigmentosum
|
Melanoma and basal/squamous cell carcinomas of the skin
|
|
|
Neoplasm associated with: albinism
|
Melanoma and basal/squamous cell carcinomas of the skin
|
|
|
Neoplasm associated with: Chronic atrophic gastritis
|
Gastric adenocarcinoma
|
|
|
Neoplasm associated with: Pernicious anemia
|
Gastric adenocarcinoma
|
|
|
Neoplasm associated with: Post surgical gastric remnants
|
Gastric adenocarcinoma
|
|
|
Neoplasm associated with: Tuberous sclerosis (facial angiofibroma, seizures, mental retardation)
|
Astrocytoma and cardiac rhabdomyoma
|
|
|
Neoplasm associated with: Actinic Keratosis
|
Squamous Cell Carcinoma of skin
|
|
|
Neoplasm associated with: Barrett's esophagus
|
Esophageal adenocarcinoma
|
|
|
Neoplasm associated with: Plummer-Vinson syndrome (atrophic glossitis, esophageal webs, anemia; all due to iron deficiency)
|
Squamous Cell carcinoma of the esophagus
|
|
|
Neoplasm associated with: Cirrhosis (alcoholic, hepatitis B and C)
|
Hepatocellular carcinoma
|
|
|
Neoplasm associated with: Ulcerative colitis
|
Colonic adenocarcinoma
|
|
|
Neoplasm associated with: Paget's disease of bone
|
Secondary osteosarcoma and fibrosarcoma
|
|
|
Neoplasm associated with: Immunodeficiency states
|
Malignant lymphomas
|
|
|
Neoplasm associated with: AIDS
|
Aggressive malignant lymphomas (non-Hodgkin's) and Kaposi's sarcoma
|
|
|
Neoplasm associated with: Autoimmune diseases
|
Benign/malignant thymomas
|
|
|
Neoplasm associated with: Acanthosis nigricans (hyperpigmentation and epidermal thickening)
|
Visceral malignancy (stomach, lung, breast, uterus)
|
|
|
Neoplasm associated with: Dysplastic nevus
|
Malignant melanoma
|
|
|
Condition associated with: ALL
|
Down syndrome (we ALL fall Down)
|
|
|
Condition associated with: AML
|
Down syndrome
|
|
|
Condition associated with: Melanoma
|
Xeroderma pigmentosum and albinism
If malignant, dysplastic nevus |
|
|
Condition associated with: Basal cell carcinoma of skin
|
Xeroderma pigmentosum and albinism
|
|
|
Condition associated with: Squamous cell carcinoma of skin
|
Actinic keratosis, Xeroderma pigmentosum and albinism
|
|
|
Condition associated with: Gastric adenocarcinoma
|
1. Chronic atrophic gastritis
2. Pernicious anemia 3. Postsurgical gastric remnants |
|
|
Condition associated with: Astrocytoma
|
Tuberous sclerosis (facial angiofibroma, seizures, mental retardation)
|
|
|
Condition associated with: Cardiac rhabdomyoma
|
Tuberous sclerosis (facial angiofibroma, seizures, mental retardation)
|
|
|
Condition associated with: Esophageal adenocarcinoma
|
Barrett's esophagus
|
|
|
Condition associated with: Squamous cell carcinoma of esophagus
|
Plummer-Vinson syndrome
|
|
|
Plummer-Vinson syndrome: Presentation
|
-Atrophic glossitis
-Esophageal webs -Anemia |
|
|
Plummer-Vinson syndrome: Cause
|
Iron deficiency
|
|
|
Condition associated with: Hepatocellular carcinoma
|
Cirrhosis due to:
1) alcohol 2) hepatitis B or C |
|
|
Condition associated with: Colonic adenocarcinoma
|
Ulcerative colitis
|
|
|
Condition associated with: Secondary osteosarcoma
|
Paget's disease of bone
|
|
|
Condition associated with: Fibrosarcoma
|
Paget's disease of bone
|
|
|
Condition associated with: Malignant lymphomas
|
Immunodeficiency states
|
|
|
Condition associated with: aggressive malignant non-Hodgkin's lymphoma
|
AIDS
|
|
|
Condition associated with: Kaposi's sarcoma
|
AIDS
|
|
|
Condition associated with: Benign thymoma
|
Autoimmune diseases (eg Hashimoto's thyroiditis, myasthenia gravis)
|
|
|
Condition associated with: Malignant thymoma
|
Autoimmune diseases (eg Hashimoto's thyroiditis, myasthenia gravis)
|
|
|
Condition associated with: Visceral malignancy
|
Acanthosis nigricans
|
|
|
Acanthosis nigricans: Presentation
|
-Hyperpigmentation
-Epidermal thickening |
|
|
Tumor associated with this gene: abl
|
CML
|
|
|
Tumor associated with this gene: c-myc
|
Burkitt's lymphoma
|
|
|
Tumor associated with this gene: bcl-2
|
Follicular and undifferentiated lymphomas (inhibits apoptosis)
|
|
|
Tumor associated with this gene: erb-B2
|
Breast, ovarian, and gastric carcinomas
|
|
|
Tumor associated with this gene: ras
|
Colon carcinoma
|
|
|
Tumor associated with this gene: L-myc
|
Lung tumor (L for Lung)
|
|
|
Tumor associated with this gene: N-myc
|
Neuroblastoma (N for Neuroblastoma)
|
|
|
Tumor associated with this gene: ret
|
Multiple endocrine neoplasia types II and III
|
|
|
Gene associated with this tumor: CML
|
oncogene abl (philadelphia chromosome)
|
|
|
Gene associated with this tumor: Burkitt's lymphoma
|
oncogene c-myc
|
|
|
Gene associated with this tumor: Follicular lymphoma
|
oncogene bcl-2 (inhibits apoptosis)
|
|
|
Gene associated with this tumor: Undifferentiated lymphoma
|
oncogene bcl-2 (inhibits apoptosis)
|
|
|
Gene associated with this tumor: Breast carcinoma
|
oncogene erb-B2
|
|
|
Gene associated with this tumor: Ovarian carcinoma
|
oncogene erb-B2
|
|
|
Gene associated with this tumor: Gastric carcinoma
|
oncogene erb-B2
|
|
|
Gene associated with this tumor: Colon carcinoma
|
oncogene ras
|
|
|
Gene associated with this tumor: Lung tumor
|
oncogene L-myc (L for Lung)
|
|
|
Gene associated with this tumor: Neuroblastoma
|
oncogene N-myc (N for neuroblastoma)
|
|
|
Gene associated with this tumor: Multiple Endocrine Neoplasia type I
|
oncogene MEN1 encoding menin on chromosome 11q
|
|
|
Gene associated with this tumor: Multiple Endocrine Neoplasia type II
|
oncogene ret
|
|
|
Gene associated with this tumor: Multiple Endocrine Neoplasia type III
|
oncogene ret
|
|
|
Chromosome and tumor associated with this gene (what type of gene): Rb
|
Tumor suppressor gene on 13q: Retinoblastoma, osteosarcoma
|
|
|
Chromosome and tumor associated with this gene (what type of gene): BRCA1
|
Tumor suppressor gene on 17q: Breast and ovarian cancer
|
|
|
Chromosome and tumor associated with this gene (what type of gene): BRCA2
|
Tumor suppressor gene on 13q: Breast and ovarian cancer
|
|
|
Chromosome and tumor associated with this gene (what type of gene): p53
|
Tumor suppressor gene on 17p: Most human cancers and Li-Fraumeni Syndrome
|
|
|
Chromosome and tumor associated with this gene (what type of gene): p16
|
Tumor suppressor gene on 9p: Melanoma
|
|
|
Chromosome and tumor associated with this gene (what type of gene): APC
|
Tumor suppressor gene on 5q: Colorectal cancer
|
|
|
Chromosome and tumor associated with this gene (what type of gene): WT1
|
Tumor suppressor gene on 11q: Wilm's tumor
|
|
|
Chromosome and tumor associated with this gene (what type of gene): NF1
|
Tumor suppressor gene on 17q: Neurofibromatosis type 1
|
|
|
Chromosome and tumor associated with this gene (what type of gene): NF2
|
Tumor suppressor gene on 22q: Neurofibromatosis type 2
|
|
|
Chromosome and tumor associated with this gene (what type of gene): DPC
|
Tumor suppressor gene on 18q: Pancreatic cancer
|
|
|
Chromosome and tumor associated with this gene (what type of gene): DCC
|
Tumor suppressor gene on 18q: Colon cancer
|
|
|
Gene and associated tumor on chromosome: 5q
|
Tumor suppressor gene APC: Colorectal cancer
|
|
|
Gene and associated tumor on chromosome: 9p
|
Tumor suppressor gene p16: melanoma
|
|
|
Gene and associated tumor on chromosome: 11q
|
Tumor suppressor gene WT1: Wilm's tumor
|
|
|
Gene and associated tumor on chromosome: 13q
|
Tumor suppressor genes Rb (Retinoblastoma, Osteosarcoma) and BRCA2 (Breast and Ovarian cancer)
|
|
|
Gene and associated tumor on chromosome: 17p
|
Tumor suppressor gene p53: Most human cancers and Li-Fraumeni syndrome
|
|
|
Gene and associated tumor on chromosome: 17q
|
Tumor suppressor genes BRCA1 (Breast and ovarian cancer) and NF1 (Neurofibromatosis type 1)
|
|
|
Gene and associated tumor on chromosome: 18q
|
Tumor suppressor genes DPC (Pancreatic cancer) and DCC (Colon cancer)
|
|
|
Gene and associated tumor on chromosome: 22q
|
Tumor suppressor gene NF2: Neurofibromatosis type 2
|
|
|
Gene and matching chromosome associated with: Retinoblastoma
|
Tumor suppressor gene Rb on chromosome 13q
|
|
|
Gene and matching chromosome associated with: Osteosarcoma
|
Tumor suppressor gene Rb on chromosome 13q
|
|
|
Gene and matching chromosome associated with: Breast cancer
|
Tumor suppressor genes BRCA1 (17q) and BRCA2 (13q)
|
|
|
Gene and matching chromosome associated with: Ovarian cancer
|
Tumor suppressor genes BRCA1 (17q) and BRCA2 (13q)
|
|
|
Gene and matching chromosome associated with: Most human cancers
|
Tumor suppressor gene p53 on chromosome 17p
|
|
|
Gene and matching chromosome associated with: Li-Fraumeni syndrome
|
Tumor suppressor gene p53 on chromosome 17p
|
|
|
Gene and matching chromosome associated with: Melanoma
|
Tumor suppressor gene p16 on chromosome 9p
|
|
|
Gene and matching chromosome associated with: Colorectal cancer
|
Tumor suppressor gene APC on chromosome 5q
|
|
|
Gene and matching chromosome associated with: Wilms' tumor
|
Tumor suppressor gene WT1 on chromosome 11q
|
|
|
Gene and matching chromosome associated with: Neurofibromatosis type 1
|
Tumor suppressor gene NF1 on chromosome 17q
|
|
|
Gene and matching chromosome associated with: Neurofibromatosis type 2
|
Tumor suppressor gene NF2 on chromosome 22q
|
|
|
Gene and matching chromosome associated with: Pancreatic cancer
|
Tumor suppressor gene DPC on chromosome 18q
|
|
|
Gene and matching chromosome associated with: Colon cancer
|
Tumor suppressor gene DCC on chromosome 18q
|
|
|
Oncogenes: gain or loss of function QUICK
|
onco: gain
|
|
|
tumor suppressor genes: gain or loss of function QUICK
|
tumor suppressor: loss
|
|
|
Oncogenes: one or two alleles need to be damaged QUICK
|
One (gain of function)
|
|
|
Tumor suppressor genes: one or two alleles need to be damaged QUICK
|
Two (loss of function)
|
|
|
Association for tumor marker: PSA
|
Screening for Prostatic Carcinoma
|
|
|
Association for tumor marker: CEA
|
-Carcinoembryonic antigen.
-In ~70% of colorrectal and pancreatic cancers -Also produced by gastric and breast carcinomas -Very nonspecific |
|
|
Association for tumor marker: alpha-fetoprotein
|
-Hepatocellular carcinomas
-Nonseminomatous germ cell tumors of the testis (eg yolk sac tumor) |
|
|
Association for tumor marker: beta-hCG
|
-Hydatidiform moles
-Choriocarcinomas -Gestational trophoblastic tumors |
|
|
Association for tumor marker: CA-125
|
-Ovarian malignant epithelial tumors
|
|
|
Association for tumor marker: S-100
|
-Melanoma
-Neural tumors -Astrocytomas |
|
|
Association for tumor marker: Alkaline phosphatase
|
-Metastases to bone
-Obstructive biliary disease -Paget's disease of bone |
|
|
Association for tumor marker: Bombesin
|
-Neuroblastoma
-Lung cancer -Gastric cancer |
|
|
Association for tumor marker: TRAP
|
-Tartrate-resistance acid phosphatase
-Found in hairy cell leukemia |
|
|
What type of cell is found in hairy cell leukemia?
|
B-cells
|
|
|
Association for tumor marker: CA-19-9
|
Pancreatic adenocarcinoma
|
|
|
Tumor marker for: Prostatic carcinoma
|
-PSA
-Prostatic acid phosphatase |
|
|
Tumor marker for: Colorectal cancer
|
CEA - Carcinoembryonic antigen
-Produced by 70% of colorectal cancers |
|
|
Tumor marker for: Pancreatic cancer
|
CEA - Carcinoembryonic antigen
-Produced by 70% of pancreatic cancers CA-19-9 -Produced in pancreatic adenocarcinoma |
|
|
Tumor marker for: Gastric carcinoma
|
-CEA - Carcinoembryonic antigen
-Bombesin |
|
|
Tumor marker for: Breast carcinoma
|
CEA - Carcinoembryonic antigen
|
|
|
Tumor marker for: Hepatocellular carcinoma
|
alpha-fetoprotein
|
|
|
Tumor marker for: Nonseminomatous germ cell tumors of the testis
|
alpha-fetoprotein
|
|
|
Tumor marker for: Hydatidiform moles
|
beta-hCG
|
|
|
Tumor marker for: Choriocarcinoma
|
beta-hCG
|
|
|
Tumor marker for: Gestational Trophoblastic tumors
|
beta-hCG
|
|
|
Tumor marker for: Malignant ovarian epithelial tumors
|
CA-125
|
|
|
Tumor marker for: Melanoma
|
S-100
|
|
|
Tumor marker for: Neural tumors
|
General: S-100
Neuroblastoma: Bombesin |
|
|
Tumor marker for: Astrocytomas
|
S-100
|
|
|
Tumor marker for: Metastases to bone
|
Alkaline phosphatase
|
|
|
Tumor marker for: Obstructive biliary disease
|
Alkaline phosphatase
|
|
|
Tumor marker for: Paget's disease of bone
|
Alkaline phosphatase
|
|
|
Tumor marker for: Neuroblastoma
|
Bombesin
|
|
|
Tumor marker for: Lung cancer
|
Bombesin
|
|
|
Tumor marker for: Hairy cell leukemia
|
TRAP (Tartrate-resistant acid phosphatase)
|
|
|
Tumor marker for: Pancreatic adenocarcinoma
|
CA-19-9
|
|
|
Cancer associated with: HTLV-1
|
HTLV=Human T-Lymphotropic Virus
Adult T-cell leukemia |
|
|
Cancer associated with: HBV
|
Hepatocellular carcinoma
|
|
|
Cancer associated with: HCV
|
Hepatocellular carcinoma
|
|
|
Cancer associated with: EBV
|
-Burkitt's lymphoma
-Nasopharyngeal carcinoma |
|
|
Cancer associated with: HPV
|
-Cervical carcinoma (with HPV 16,18)
-Penile/anal carcinoma |
|
|
Cancer associated with: HHV-8
|
HHV-8 = Kaposi's sarcoma-associated herpes virus
-Kaposi's sarcoma -body cavity fluid B-cell lymphoma |
|
|
Oncogenic virus associated with: Adult T-cell leukemia
|
HTLV-1 (HTLV=Human T-Lymphotropic Virus)
|
|
|
Oncogenic virus associated with: Hepatocellular carcinoma
|
-HBV
-HCV |
|
|
Oncogenic virus associated with: Burkitt's lymphoma
|
EBV
|
|
|
Oncogenic virus associated with: Nasopharyngeal carcinoma
|
EBV
|
|
|
Oncogenic virus associated with: Cervical carcinoma
|
HPV 16 and 18
|
|
|
Oncogenic virus associated with: Penile carcinoma
|
HPV
|
|
|
Oncogenic virus associated with: Anal carcinoma
|
HPV
|
|
|
Oncogenic virus associated with: Kaposi's sarcoma
|
HHV-8 (aka Kaposi's sarcoma-associated herpesvirus)
|
|
|
Oncogenic virus associated with: body cavity fluid B-cell lymphoma
|
HHV-8 (Human Herpesvirus 8)
|
|
|
Organ affected by: Aflatoxins
|
Liver (hepatocellular carcinoma)
|
|
|
Organ affected by: Vinyl chloride
|
Liver (angiosarcoma)
|
|
|
Organ affected by and effects of: CCl4
|
Liver
-centrilobular necrosis -fatty change |
|
|
Organ affected by: Nitrosamines
|
-Esophagus
-Stomach |
|
|
Organ affected by: Cigarette smoke
|
-Larynx
-Lung |
|
|
Organ affected by: Asbestos
|
Lung
-Mesothelioma -Bronchogenic carcinoma |
|
|
Organ affected by: Arsenic
|
Skin (squamous cell carcinoma)
|
|
|
Organ affected by: Naphthalene (aniline) dyes
|
Bladder (transitional cell carcinoma)
|
|
|
Organ affected by: Alkylating agents
|
Blood (leukemia)
|
|
|
Carcinogen associated with: Hepatocellular carcinoma
|
Aflatoxins
|
|
|
Carcinogen associated with: Angiosarcoma
|
Vinyl chloride
|
|
|
Carcinogen associated with: Centrilobular necrosis of liver
|
CCl4
|
|
|
Carcinogen associated with: Fatty change of liver
|
CCl4
|
|
|
Carcinogen associated with: Liver
|
-Aflatoxins
-Vinyl chloride -CCl4 |
|
|
Carcinogen associated with: Esophagus
|
Nitrosamines
|
|
|
Carcinogen associated with: Stomach
|
Nitrosamines
|
|
|
Carcinogen associated with: Larynx
|
Cigarette smoke
|
|
|
Carcinogen associated with: Lung
|
-Cigarette smoke
-Asbestos |
|
|
Carcinogen associated with: Mesothelioma of lung
|
Asbestos
|
|
|
Carcinogen associated with: Bronchogenic carcinoma of lung
|
Asbestos
|
|
|
Carcinogen associated with: Skin
|
Arsenic (squamous cell carcinoma)
|
|
|
Carcinogen associated with: Bladder
|
Naphthalene dyes (transitional cell carcinoma)
|
|
|
Carcinogen associated with: Blood
|
Alkylating agents (leukemia)
|
|
|
Paraneoplastic effects: definition
|
Symptoms not directly related to tumor or hormones of tumor tissue
|
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Small cell lung carcinoma
|
(with intracranial neoplasms)
-Cause: ADH -Effect: SIADH (without intracranial neoplasms) -Cause:ACTH/ACTH-like peptide -Effect: Cushing's -Cause:Antibodies against presynaptic Ca2+ channels at neuromuscular junction -Effect: Lambert-Eaton Syndrome (muscle weakness) |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Squamous cell lung carcinoma
|
Causes:
-PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Effect: Hypercalcemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Renal cell carcinoma
|
Cause: Erythropoietin
Effect: Polycythemia Causes: -PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Effect: Hypercalcemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Breast carcinoma
|
Causes:
-PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Effect: Hypercalcemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Multiple myeloma
|
Causes:
-PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Effect: Hypercalcemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Bone metastasis (lysed bone)
|
(Though technically not a paraneoplastic syndrome)
Causes: -PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Effect: Hypercalcemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Hemangioblastoma
|
Cause: Erythropoietin
Effect: Polycythemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Hepatocellular carcinoma
|
Cause: Erythropoietin
Effect: Polycythemia |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Thymoma
|
-Cause:Antibodies against presynaptic Ca2+ channels at neuromuscular junction
-Effect: Lambert-Eaton Syndrome (muscle weakness) |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Leukemia
|
Cause: Hypercalcemia due to excess nucleic acid turnover (ie, cytotoxic therapy)
Effects: -Gout -Urate nephropathy |
|
|
Name/effect and cause of paraneoplastic syndrome associated with: Lymphoma
|
Cause: Hypercalcemia due to excess nucleic acid turnover (ie, cytotoxic therapy)
Effects: -Gout -Urate nephropathy |
|
|
Paraneoplastic syndrome and neoplasm associated with: ACTH
|
Paraneoplastic syndrome: Cushing's syndrome
Neoplasm: Small cell lung carcinoma |
|
|
Paraneoplastic syndrome and neoplasm associated with: ACTH-like peptide
|
Paraneoplastic syndrome: Cushing's syndrome
Neoplasm: Small cell lung carcinoma |
|
|
Paraneoplastic syndrome and neoplasm associated with: ADH
|
Paraneoplastic syndrome: SIADH
Neoplasm: Small cell lung carcinoma with intracranial neoplasms |
|
|
Paraneoplastic syndrome and neoplasm associated with: PTH-related peptide
|
Paraneoplastic syndrome: Hypercalcemia
Neoplasms: -Squamous cell lung carcinoma -Renal cell carcinoma -Breast carcinoma -Multiple myeloma -Bone metastasis (lysed bone) (not really a paraneoplastic syndrome for this one) |
|
|
Paraneoplastic syndrome and neoplasm associated with: TGF-beta
|
Paraneoplastic syndrome: Hypercalcemia
Neoplasms: -Squamous cell lung carcinoma -Renal cell carcinoma -Breast carcinoma -Multiple myeloma -Bone metastasis (lysed bone) (not really a paraneoplastic syndrome for this one) |
|
|
Paraneoplastic syndrome and neoplasm associated with: TNF-alpha
|
Paraneoplastic syndrome: Hypercalcemia
Neoplasms: -Squamous cell lung carcinoma -Renal cell carcinoma -Breast carcinoma -Multiple myeloma -Bone metastasis (lysed bone) (not really a paraneoplastic syndrome for this one) |
|
|
Paraneoplastic syndrome and neoplasm associated with: IL-1
|
Paraneoplastic syndrome: Hypercalcemia
Neoplasms: -Squamous cell lung carcinoma -Renal cell carcinoma -Breast carcinoma -Multiple myeloma -Bone metastasis (lysed bone) (not really a paraneoplastic syndrome for this one) |
|
|
Paraneoplastic syndrome and neoplasm associated with: Erythropoietin
|
Paraneoplastic syndrome: Polycythemia
Neoplasms: -Renal cell carcinoma -hemangioblastoma -hepatocellular carcinoma |
|
|
Paraneoplastic syndrome and neoplasm associated with: Antibodies against Ca2+ channels
|
Paraneoplastic syndrome: Lambert-Eaton syndrome (muscle weakness due to presynaptic channels being destroyed)
Neoplasms: -Thymoma -Small-cell lung cancer |
|
|
Paraneoplastic syndrome and neoplasm associated with: Hyperuricemia due to excess nucleic acid turnover (ie cytotoxic therapy)
|
Paraneoplastic syndromes:
-Gout -Urate nephropathy Neoplasms: -Leukemia -Lymphoma |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Cushing's syndrome
|
Cause: ACTH or ACTH-like peptide
Neoplasm: Small cell lung carcinoma |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: SIADH
|
Cause: ADH
Neoplasms: Small cell lung carcinoma with intracranial neoplasms |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Hypercalcemia
|
Causes:
-PTH-related peptide -TGF-beta -TNF-alpha -IL-1 Neoplasms: -Squamous cell lung carcinoma -Renal cell carcinoma -Breast carcinoma -Multiple myeloma -Bone metastasis (lysed bone: technically not a paraneoplastic cause) |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Polycythemia
|
Cause: Erythropoietin
Neoplasms: -Renal cell carcinoma -Hemangioblastoma -Hepatocellular carcinoma |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Lambert-Eaton syndrome (muscle weakness)
|
Cause: Antibodies against presynaptic Ca2+ channels at neuromuscular junction
Neoplasms: -Thymoma -Small cell lung carcinoma |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Gout
|
Cause: Hyperuricemia due to excess nucleic acid turnover (ie cytotoxic therapy)
Neoplasms: -Leukemias -Lymphomas |
|
|
For the following paraneoplastic syndrome, give the causes and associated neoplasms: Urate nephropathy
|
Cause: Hyperuricemia due to excess nucleic acid turnover (ie cytotoxic therapy)
Neoplasms: -Leukemias -Lymphomas |
|
|
Primary tumors that metastasize to the brain
|
Lots of Bad Stuff Kills Glia
-Lung -Breast -Skin (melanoma) -Kidney (renal cell carcinoma) -GI |
|
|
Primary tumors that metastasize to the liver
|
Cancer Sometimes Penetrates Benign Liver
By decreasing frequency: -Colon -Stomach -Pancreas -Breast -Lung |
|
|
Primary tumors that metastasize to bone
|
Primary Tumors Like Killing Bone
-Prostate (blastic) -Thyroid/Testes -Lung (Lytic) -Kidney -Breast (Both lytic and blastic) Prostate and bone are most common |
|
|
% of brain tumors from metastases
|
50%
|
|
|
% of liver tumors from metastases
|
Unspecified, but there are many more metastases than primary liver tumors
|
|
|
% of bone tumors from metastases
|
Unspecified, but there are many more metastases than primary bone tumors
|
|
|
Brain metastasis: Morphology
|
-Multiple
-Well circumscribed -At gray/white border |
|
|
Incidence and mortality in men of the following cancer: Prostate
|
Incidence: 32%
Mortality: 13% |
|
|
Incidence in men of the following cancer: Lung
|
Incidence: 16%
Mortality: 33% |
|
|
Incidence in men of the following cancer: Colon and rectum
|
Incidence: 12%
Mortality: Unspecified |
|
|
Incidence and mortality in women of the following cancer: Breast
|
Incidence: 32%
Mortality: 18% |
|
|
Incidence and mortality in women of the following cancer: Lung
|
Incidence: 13%
Mortality: 23% |
|
|
Incidence and mortality in women of the following cancer: Colon and Rectum
|
Incidence: 13%
Mortality: Unspecified |
|
|
Karyolysis (seen as nuclear fading indicating chromatin dissolution caused by action of DNAses and RNAses)
|
What process does the following cell demonstrate?
|
|
|
Pyknosis (nuclear shrinkage when DNA condenses into shrunken basophilic mass)
|

What process does the following cell demonstrate?
|
|
|
Karyorrhexis (nuclear fragmentation due to rupture of pyknotic nucleic membranes)
|

What process does the following cell demonstrate?
|
|
|
Normal cells, no hyperplasia or dysplasia
|

Stage of cancer progression
|
|
|
Hyperplasia, no dysplasia
|

Stage of cancer progression
|
|
|
Hyperplasia with mild dysplasia
|
Stage of cancer progression
|
|
|
Severe dysplasia AKA carcinoma in situ
|

Stage of cancer progression
|
|
|
Cancer, invasive
|

Stage of cancer progression
|
|
|
Type of necrosis found in: Heart
|
Coagulative
|
|
|
Type of necrosis found in: Liver
|
Coagulative
|
|
|
Type of necrosis found in: Kidney
|
Coagulative
|
|
|
Type of necrosis found in: Brain
|
Liquefactive
|
|
|
Type of necrosis found in: Tuberculosis
|
Caseous
|
|
|
Type of necrosis found in: Pancreas
|
Fat
|
|
|
Type of necrosis found in: Blood vessels
|
Fibrinoid
|
|
|
Type of necrosis found in: Limbs
|
Gangrenous
|
|
|
Type of necrosis found in: GI tract
|
Gangrenous
|

