![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
21 Cards in this Set
- Front
- Back
|
5 broad categories of chest pain:
|
Cardiac causes, gastrointestinal disorders, pulmonary disorders, musculoskeletal causes, and psychogenic causes
|
|
|
Cardiac causes of chest pain differential:
|
-Stable angina
-Unstable angina -Acute MI -Atypical or variant angina (coronary vasospasm, Prinzmetal's angina) -Cocaine-induced chest pain -Pericarditis -Aortic dissection: tearing chest pain radiating to back -Valvular heart disease, i.e., critical aortic stenosis -Cardiac arrhythmia |
|
|
Gastrointestinal disorders causes of chest pain:
|
-Esophageal disease (GERD, esophagitis, esophageal dysmotility)
-Biliary disease (cholecystitis, cholangitis): typically RUQ with radiation to shoulder, may be referred to chest -Peptic ulcer disease -Pancreatitis |
|
|
Pulmonary disorders causing chest pain:
|
-Pneumonia
-Spontaneous pneumothorax -Pleurisy -Pulmonary embolism -Pulmonary hypertension/cor pulmonale -Pleural effusion |
|
|
Musculoskeletal causes causing chest pain:
|
-Costochondritis
-Rib fracture -Myofascial pain syndromes -Muscular strain -Herpes zoster |
|
|
Psychogenic causes of chest pain:
|
-Panic disorders
-Hyperventilation -Somatoform disorders |
|
|
Cardiac risk factors
|
smoking, hypertension, dyslipidemia, diabetes, family history of CAD, or previously documented CAD, peripheral arterial disease, or stroke
|
|
|
Ischemic vs. Non-ischemic pain
|
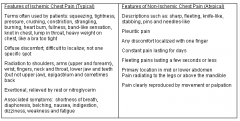
|
|
|
Atypical symptoms of a cardiac event
|
dyspnea, fatigue, nausea, abdominal discomfort, or syncope
|
|
|
Classic angina
|
is retrosternal chest pain that comes on with exertion and is relieved with rest or nitroglycerin - stable angina describes symptoms that have been occurring chronically and are predictable with exertion.caused by a stable atherosclerotic plaque
|
|
|
Unstable angina
|
is when the chest pain occurs at rest, is new, is increasing in frequency, or when its onset is triggered with a lower level of exertion caused by an unstable plaque that has ruptured and caused a non-occlusive thrombus
|
|
|
Diagnosis of acute MI
|
the typical rise and fall of troponin or creatine kinase myocardial band (CK-MB) plus ONE of the following:
- Symptoms consistent with myocardial ischemia - Electrocardiogram changes indicating myocardial ischemia (ST-segment elevation or depression) - New pathologic Q waves - Findings on percutaneous coronary intervention (PCI). |
|
|
What's the difference clinically btwn acute NSTEMI and unstable angini
|
No troponin increase = No MI
|
|
|
Treatments for unstable angina
|
sublingual nitroglycerin, beta blockers, heparin, aspirin, statin, PCI
|
|
|
The (thrombolysis in myocardial infarction)TIMI risk score includes the following items
|
If present, the item is scored is +1, if absent, the score is 0.
Age ≥65 years Presence of at least three risk factors for CHD (hypertension, diabetes, dyslipidemia, smoking, or positive family history of early MI) Prior coronary stenosis of ≥50 percent Presence of ST-segment deviation on admission ECG At least two anginal episodes in prior 24 hours Elevated serum cardiac biomarkers Use of aspirin in prior seven days (which is probably a marker for more severe coronary disease) Patients are considered to be at low risk with a score of 0 to 2; intermediate risk with a score of 3 to 4; and high risk with a score of 5 to 7. |
|
|
Rough ECG anatomy
|
V1-V4 reflect the anterior wall; leads II, III and AVF reflect the inferior portion of the heart; and leads I, AVL, V5 and V6 correspond to the lateral myocardial wall.
|
|
|
Left Bundle Branch Block diagnosis criteria:
|
The criteria to diagnose a left bundle branch block on the electrocardiogram:
The heart rhythm must be supraventricular in origin. The QRS duration must be = or > 120 ms. There should be a QS or rS complex in lead V1. There should be a monophasic R wave in leads I and V6. The T wave should be deflected opposite the terminal deflection of the QRS complex |
|
|
absolute contraindications for thrombolytic therapy include:
|
Strong suspicion of dissection of the aorta
Pericardial effusion Active gastrointestinal or other internal bleeding Brain tumor, arteriovenous malformation, or aneurysm Ischemic stroke in preceding 6 months (a verified transient ischemic attack (TIA) is an exception) Previous intracerebral hemorrhage or subarachnoid hemorrhage Intracranial procedure or recent head trauma Severe known bleeding disorder: coagulation abnormality, thrombocytopenia, etc. |
|
|
a GP IIb/IIIa inhibitor such as abciximab or eptifibatide
|
inhibits platelet aggregation and may prevent platelet adhesion to the vessel wall. While these medications increase the risk of bleeding (especially when used in combination with fibrinolytics) and can cause thrombocytopenia within 24 hours of initiation, they improve outcomes in patients with STEMI.
|
|
|
when do you prefer CABG vs. PCI
|
CABG may be preferred in left main lesions or in complex proximal LAD disease with other unfavorable lesions (three-vessel disease) or in patients with left ventricular dysfunction or diabetes mellitus.
|
|
|
acute complications of acute MI
|
include arrhythmias (bradyarrhythmias and tachyarrhythmias), reduced ventricular function, cardiogenic shock, papillary muscle dysfunction with acute valvular dysfunction, ventricular free wall rupture, and recurrent thrombosis.
|

