![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
54 Cards in this Set
- Front
- Back
|
patient is hooked up to a monitor. You see V-fib. What should you do |
Immediate shock
Biphasic: 200 Monophasic: 360 |
|
|
How often can epinephrine be given? |
Every 3-5 minutes
dose: 1mg 40 units of Vasopressin can replace the first or second dose of epi |
|
|
you have shouted for help and have started the emergency response. What are the first three things you should do when a patient goes down |
Start CPR
Give O2 Attach monitor/defib |
|
|
To ensure proper CPR quality, how deep should you push? |
>2 inches [5cm]
>100/min allow complete chest recoil |
|
|
How often should you rotate the compressor?
|
every 2 minutes
|
|
|
If no advanced airway is available, what should your compression-ventilation ratio be? |
30:2
|
|
|
a patient is receiving CPR. An advanced airway is placed and quantitative waveform capnography is in place. What PETCO2 suggests that CPR quality is INADEQUATE
|
<10mmHg
|
|
|
a patient is receiving CPR. An advanced airway is placed and and intra-arterial pressure is available. If relation phase (diastolic) pressure is <__mmHg, you should attempt to improve CPR quality |
<20mmHg
|
|
|
At what PETCO2 can you see ROSC? |
>40mmHg
also look for return of pulse and BP |
|
|
What is the proper initial dose of Amiodarone? |
initial: 300mg bolus
Second: 150 |
|
|
if an advanced airway is in place, how many breaths/min should be given with continuous chest compression?
|
8-10
|
|
|
List the 5 H's that can be reversible causes of irregular rhythm
|
Hypovolemia
Hypoxia Hydrogen ion (acidosis) Hypo/hyperkalemia Hypothermia |
|
|
List the 5 T's that can be reversible causes of irregular rhythm
|
Tension pneumonthorax
Tamponade Toxins Thrombosis, pulmonary Thrombosis, coronary |
|
|
What drug is recommended for the initial treatment of stable monomorphic wide-complex tachycardia?
|
Adenosine
|
|
|
What drug SHOULD NOT be used for IRREGULAR wide-complex tachy?
Why? |
Adenosine
may cause degeneration of the rhythm to VF |
|
|
After obtaining ROSC, what oxyhemoglobin saturation do you want?
|
>94%
the fraction of inspired oxygen (FIO2) should be adjusted to the minimum concentration needed to achieve arterial oxyhemoglobin saturation ≥94%, with the goal of avoiding hyperoxia while ensuring adequate oxygen delivery. |
|
|
With renewed focus on improving functional outcome, neurologic evaluation is a key component in the routine assessment of survivors. Early recognition of potentially treatable neurologic disorders, such as ________, is important. The diagnosis of these
may be challenging, especially in the setting of hypothermia and neuromuscular blockade, and electroencephalographic monitoring has become an important diagnostic tool in this patient population. Prognostic assessment in the setting of hypothermia is changing, and experts qualified in neurologic assessment |
Seizures
|
|
|
in general, what should be performed after cardiac arrest
|
PCI
even if not clearly a STEMI |
|
|
When should morphine be given in a STEMI situation
|
if a pt has chest pain unresponsive to nitrates
|
|
|
in unstable angina/NSTEMI, _______ should be avoided because it was associated with increased mortality
|
Morphine
|
|
|
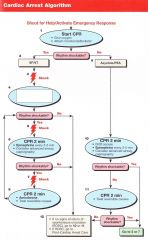
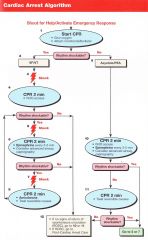
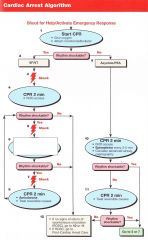
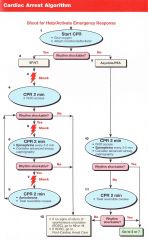
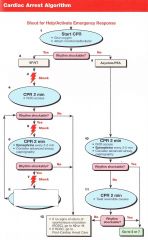
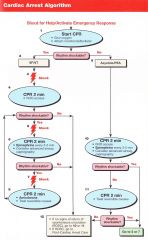
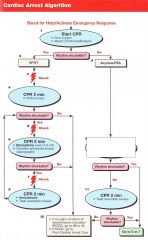
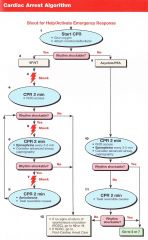
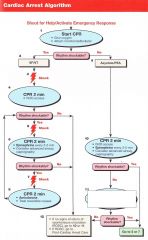
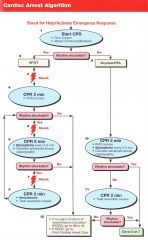
Patient presents in VT/VF. what is the first thing you do?
|
Shock 200J (biphasic)
|
|
|
Pt has VT/VF, you have given the first shock. What do you next?
|
CPR for 2 minutes/5 Cycles
Obtain IV/IO access recheck rhythm |
|
|
Pt has VT/VF, you have given the first shock. 5 cycles of CPR are done and IV access is obtained. VT/VF remains. What do you do?
|
Shock
Followed by 2 min/5 cycles of CPR Epi 1 mg given every 3-5 minutes consider advanced airway/capnography |
|
|
Pt has VT/VF, you have given the first shock. 5 cycles of CPR are done and IV access is obtained. VT/VF remains. You shock again and begin CPR. What is the next step? |
1 mg Epinephrine every 3-5 minutes
check the rhythm |
|
|
Pt has VT/VF, you have given the first shock. 5 cycles of CPR are done and IV access is obtained. VT/VF remains. You shock again and begin CPR. 1 mg of Epi is given. Rhythm is still shockable. What are the next 2 steps? |
CPR 2 minutes/5 cycles |
|
|
VT->Shock->CPR->VF->Shock->CPR->1mg epi->VF->Shock->Amiodarone 300mg-->VT->Shock->CPR-->1mg epi-->VT-->Shock-->??
|
Amiodarone 150mg
|
|
|
VT->Shock->CPR->VF->Shock->CPR->1mg epi->VF->Shock->??
|
Amiodarone 300mg
|
|
|
VT->Shock->CPR->VF->Shock->CPR->?
|
1mg Epi
|
|
|
VT->Shock->CPR->VF->Shock->CPR->1mg epi->VF->Shock->Amiodarone 300mg-->VT->Shock->CPR-->??
|
1mg epi
|
|
|
Pt arrives in PEA/Asystole. What do you do first?
|
CPR 2 minutes/ 5 Cycles
Obtain IV/IO access Epi 1 mg every 3-5 minutes Consider advanced Airway |
|
|
PEA-> CPR->Epi 1 mg-> VT ->?
|
Shock
|
|
|
PEA-> CPR->Epi 1 mg-> VT ->Shock->?
|
CPR
|
|
|
PEA-> CPR->Epi 1 mg-> VT ->Shock->CPR->
|
Epi 1 mg
|
|
|
VT->CPR->PEA->?
|
CPR
|
|
|
VT->CPR->VT->CPR->Epi->ROSC->?
|
CPR 2 minutes/5 cycles
|
|
|
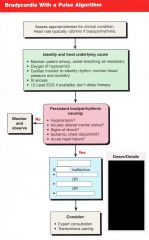
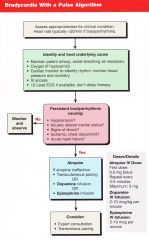
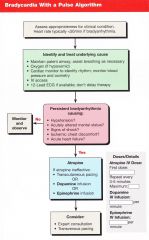
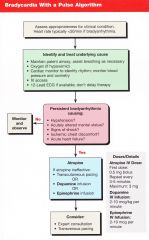
Patient presents with bradycardia (typically <50 if bradyarrhythmia) with a pulse. You have lookded for underlying cause (maintain airway, O2, monitor, BP, IV access).
The brady persists causing any of the following: Hypotension, AMS, Shock, Ischemia, heart failure. What is the first step? |
Atropine 0.5mg bolus
repeat every 3-5 min max dose is 3mg |
|
|
Patient presents with bradycardia (typically <50 if bradyarrhythmia) with a pulse. You have lookded for underlying cause (maintain airway, O2, monitor, BP, IV access).
The brady persists causing any of the following: Hypotension, AMS, Shock, Ischemia, heart failure. You give Atropine (what dose again?). How long do you wait and what is the next step? |
initial dose 0.5mg bolus
wait 3-5 min give 0.5mg again max dose 3mg |
|
|
when considering bradycardia with a pulse what is the max amount of atropine you can give?
|
3mg
it is given in 0.5mg doses so 6 doses |
|
|
Instead of atropine, what can be given for bradycardia? Consider doses
|
Dopamine IV infusion (2-10mcg/kg/min)
Epinephrine IV infusion (2-10mcg/min) |
|
|
Patient presents with bradycardia (typically <50 if bradyarrhythmia) with a pulse. You have lookded for underlying cause (maintain airway, O2, monitor, BP, IV access).
The brady persists causing any of the following: Hypotension, AMS, Shock, Ischemia, heart failure. You have now given 3mg of Atropine pt is still unstable. Next step? |
Transvenous pacing
|
|
|
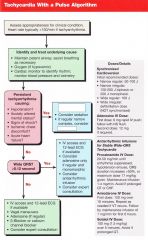
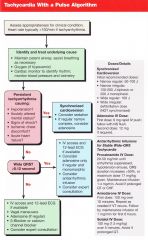
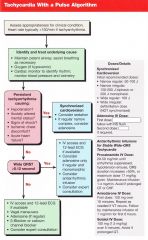
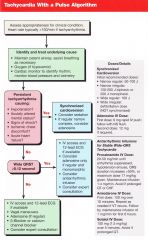
Pt has persistent tachy arrhythmia (HR usually>150) causing any of the following: Hypotension, AMS, Shock, Ischemic chest discomfort, acute heart failure.
What are your two options? |
Synchronized cardioversion
Adenosine (6mg rapid IV push, follow NS, 2nd dose 12 if needed) |
|
|
Give the doses of synchronized cardioversion considering the following rhythms:
Narrow regular: Narrow irregular: Wide regular: Wide irregular: |
Narrow regular: 50-100J
Narrow irregular: 120-200J biphasic or 200J mono Wide regular: 100J Wide irregular: DEFIBRILLATION (not synchronized) |
|
|
Pt has wide complex (QRS >0.12) stable tachycardia >150. What should be considered as tx?
|
IV access and 12 lead
Consider Adenosine only if regular and monomorphic Consider antiarrhythmic infusion (procainamide, amiodarone, sotalol) |
|
|
Pt has narrow complex (QRS <0.12) stable tachycardia >150. What should be considered as tx?
|
IV access and 12 lead
Vagal maneuvers Adenosine (if regular) B-blocker or CCB |
|
|
when can vagal maneuvers be tried to stabilize a pt?
|
Stable narrow complex tachycardia
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Adenosine Dose?
|
|

