![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
121 Cards in this Set
- Front
- Back
|
What are the two types of hyperkaratosis?
|
Ortho and parakeratosis
|
|
|
What are the main categories (think layers) of skin that can react to injury?
|
Epidermis
Dermis Subcutis Adnexa |
|
|
T or F:
Nuclei are present in the keratinocytes with orthokeratosis. |
False! This describes parakaratosis!
|
|
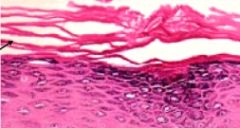
Does this image depict ortho or parakaratosis?
|
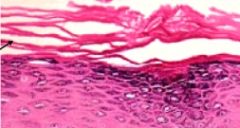
Orthokaratosis (note the anuclear keratinocytes)
|
|
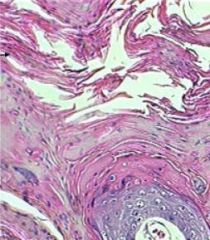
Does this image depict ortho or parakaratosis?
|
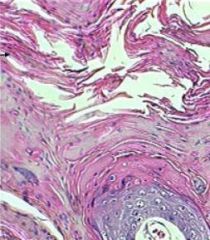
Parakaratosis (note the nucleated keratinocytes)
|
|
|
T or F:
Hypergranulosis is a characteristic of orthokeratosis. |
False! HYPOgranulosis (anuclear) is a characteristic of parakaratosis.
|
|
|
What is the most important piece of information to determine if a sample is normal skin or shows epidermal hyperplasia?
|
Need location of biopsy
|
|
|
Premature keratinization is also known as...
|
...DYSKERATOSIS
|
|
|
Abnormal development or abnormal maturation describes which process?
|
Dysplasia
|
|
|
What are some histologic hallmarks of apoptosis?
|
Condensed nucleus
Hypereosinophilic cytoplasm |
|
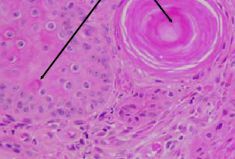
What process do the structures indicated by the arrows depict?
|
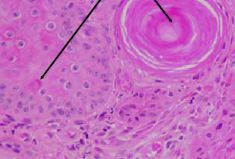
Dyskeratosis (dysplasia of keratin)
|
|
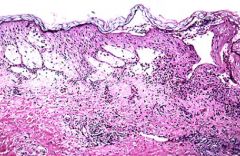
Is the edema in this image intracellular or intercellular? What is the specific name for this condition?
|
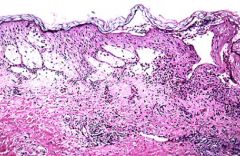
Intercellular edema = spongiosis
|
|
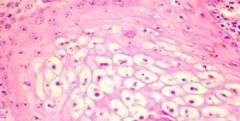
Does this image depict intracellular or intercellular fluid accumulation? What is the term for this process?
|
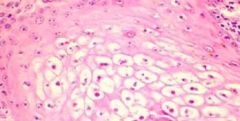
Intercellular fluid accumulation
Degeneration (in this case both ballooning and vacuolar degenaration) |
|
|
Let's play ballooning or vacuolar degeneration...
...occurs basally. |
Vacuolar
|
|
|
Let's play ballooning or vacuolar degeneration...
...occurs superficially. |
Ballooning
|
|
|
Let's play ballooning or vacuolar degeneration...
...associated with autoimmune disorders. |
Vacuolar
|
|
|
Let's play ballooning or vacuolar degeneration...
...associated with viral or metabolic disease. |
Ballooning
|
|
|
Disruption of intercellular connections is known as...
|
...acantholysis
|
|
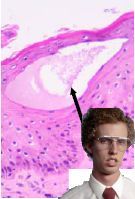
This is a flippin' sweet example of what type of lesion?
|
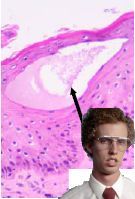
Vesicle
|
|
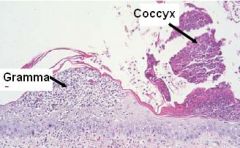
What type of lesion does "Gramma" depict? How about her "coccyx"?
|
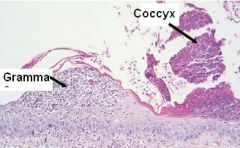
Gramma = pustule
Coccyx = crust |
|
|
What is the main difference between a vesicle and a pustule?
|
A pustule contains cells (neutrophils)
|
|
|
Dried exudate is also known as...
|
...crust
|
|
|
The transmigration of leukocytes through the epidermis is also known as...
|
...exocytosis
|
|
|
What are three reactions to skin injury that involve pigmentation?
|
hyperpigmentation
hypopigmentation pigmentary incontinence |
|
|
Melanophages in the superficial dermis describes which process?
|
Pigmentary incontinence
|
|
|
Which layer must be damaged in order for there to be pigmentary incontinence?
|
Stratum basale and basement membrane (allows melanocytes through to be phagocytosed)
|
|
|
T or F:
Pigmentary incontinence is usually a chronic process. |
True! Due to chronic irritation or inflammation
|
|
|
T or F:
Hypopigmentation can be genetic OR acquired. |
True
|
|
|
What are four reactions to injury that involve dermal collagen? Which is chiefly a genetic defect?
|
Hyalinization
Lysis Atrophy Dysplasia (genetic) |
|
|
What is the chain of events leading to pachyderma or elephantiasis in the dermis?
|
Fibroplasia > fibrosis > sclerosis > pachyderma/elephantiasis
|
|
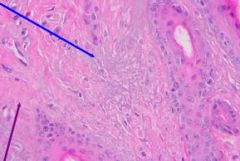
What does the blue arrow depict? The purple arrow? What tissue does each involve?
|
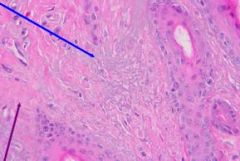
Blue = Solar elastosis (elastic fibers)
Purple = fibrosis (collagen) |
|
|
What are some abnormal dermal deposits that can occur?
|
Amyloid
Lipids Mineralization (Calcium) Mucin |
|
|
An acquired mucinous dermal deposit is known as...
|
...myxedema
|
|
|
What exudates are possible in dermal inflammation? (hint - there are 6)
|
histiocytic/granulomatous
suppurative eosinophilic lymphoplasmacytic necrotizing fibrosing |
|
|
What are the four causes of disease in dermatopathology? Which is most important?
|
(in order of most to least important)
a. Bacterial b. Fungal c. Parasitic d. Viral infxn |
|
|
There are three portals of entry for skin infections. What are they?
|
Follicular
Hematogenous Direct (penetration) |
|
|
How are pyodermas classified?
|
By depth of infection
|
|
|
What is the most common type of pyoderma?
|
Superficial pyoderma
|
|
|
Puppy pyoderma is better known as..
|
...superficial staphylococcal pyoderma
|
|
|
A flat or level color change within the skin is also known as a(n)...
|
...macule
|
|
|
A solid dermal or epidermal elevation that is <1cm is also known as a(n)...
|
...papule
|
|
|
A solid dermal or epidermal elevation that is >1cm is also known as a(n)...
|
...nodule
|
|
|
An elevation due to dermal edema is also known as a(n)...
|
...wheal
|
|
|
In which layer does edema form causing a wheal?
|
In stratum papillare of dermis
|
|
|
A fluid-filled elevation that is <1cm is known as a(n)...
|
...vesicle
|
|
|
A fluid-filled elevation that is >1cm is known as a(n)...
|
Bulla
|
|
|
A cell-filled elevation is known as a(n)...
|
pustule
|
|
|
What cell type usually fills a pustule?
|
Granulocytes (neutrophils mostly)
|
|
|
What is a multichambered pustule called?
|
A pock
|
|
|
Tightly clustured pustules is known as...
|
...impetigo
|
|
|
T or F:
Crust is a secondary lesion. |
True
|
|
|
What are some common secondary skin lesions?
|
Crust
Scale Erosion Ulcer Fissure |
|
|
What are some follicular responses to injury? (hint; there are 6)
|
Hyperkaratosis
Atrophy Arrest in phase of cycle Dysplasia Folliculitis Furunculosis |
|
|
What are the three types of folliculitis?
|
Luminal
Mural Perifollicular |
|
|
Follicular destruction due to inflammation is known as...
|
...furunculosis
|
|
|
What are some common bacterial pathogens causing superficial pyoderma?
|
Staphlyococci
Streptococci Corynebacterium Actinomyces Dermatophilus |
|
|
What mediates type I hypersensitivity?
|
IgE
|
|
|
What mediates type II hypersensitivity?
|
IgG or IgM
|
|
|
What mediates type III hypersensitivity?
|
immune complex + IgG or IgM
|
|
|
What mediates type IV hypersensitivity?
|
Cell-mediated (CD4+ or CD8+ lymphocytes)
|
|
|
Anaphylaxis is another name for which type of hypersensitivty? What cell type is primarily mobilized?
|
Type I
Mast Cells |
|
|
What event causes the massive degranulation of mast cells in type I hypersensitivity?
|
Antibody bridging
|
|
|
What are some common type I hypersensitivity syndromes?
|
Urticaria (hives)
atopic dermatitis food + parasite hypersensitivity anaphylaxis |
|
|
What type of hypersensitivity features direct cytotoxicity via complement activation?
|
Type II (autoimmune diseases)
|
|
|
What are some autoimmune skin diseases involving type II hypersensitivity?
|
Pemphigus complex
Bullous pemphigoid |
|
|
What are some examples of type III hypersensitivity?
|
Systemic Lupus Erythematous (SLE)
Hemorrhagic Purpura (Strept. equi) |
|
|
What are some examples of type IV hypersensitivity reactions?
|
Fungal dermatitis + Tbc reaction
Atopic dermatitis Contact hypersensitivity, Graft-versus-host |
|
|
What type(s) of hypersensitivity does urticaria usually involve?
|
Type I and III
|
|
|
T or F:
Acute urticaria involves wheals while chronic urticaria involves papules. |
True!
|
|
|
The increased vascular permeability shown in cutaneous hypersensitivity is called __________ when dermal and _________when subcutaneous.
|
urticaria (dermal)
angioedema (subcutaneous) |
|
|
Which species are commonly afflicted with urticaria/angioedema?
|
horse and dog
|
|
|
What will be seen histologically with urticaria/angioedema?
|
mast cells
eosinophils subepidermal edema |
|
|
How is the antigen introduced into the body in atopic dermatitis?
|
inhaled or percutaneously absorbed
|
|
|
What type of hypersensitivity is involved in atopic dermatitis? In which animals is this commonly seen?
|
Mostly type I (maybe type IV)
dogs, cats, horses |
|
|
What is the primary clinical sign of atopic dermatitis (grossly)?
|
pruritis and self trauma from scratching
alopecia |
|
|
What are common allergens involved in atopic dermitis?
|
dust mites
pollen bacteria |
|
|
What are histopathologic features of acute atopic dermatitis? chronic?
|
eosiniphilic dermatitis (acute)
hyperplastic epidermis (chronic) |
|
|
A food allergy is an example of which type of hypersensitivity? In which domestic species is this common?
|
Type I
kats and dawgs |
|
|
What is the macroscopic presentation of a food allergy?
|
pruritis of the ventral abdomen and thorax
cats often involve the head |
|
|
What is the histopathologic presentation of a food allergy?
|
Perivascular dermatitis with large numbers of eosinophils and neutrophils, mast cells
|
|
|
What type of hypersensitivity is associated with an insect bite?
|
Type I and IV
|
|
|
There are multiple factors (7) that cause pathological changes in the skin. What are they?
|
1. Congenital/heriditary dz
2. Reactions to injury 3. Environmentally-related dz 4. metabolic/nutritional dz 5. hypersensitivity/autoimmune 6. infectious dz 7. neoplasms |
|
|
What are three major differentials when dealing with bacterial skin diseases?
|
Pyoderma
Bacterial granulomas Toxin producing bacteria (systemic or localized) |
|
|
Which species are commonly afflicted with dermatophilosis? What is a major sign grossly?
|
Horses, sheep and cattle
WET hair coat |
|
|
What are some differentials to keep in mind for greasy pig disease?
|
Exudative dermatitis caused by S. hyicus
Parakeratosis diatatica (Zn deficiency) Epidermitis exsudativa Cutaneous strongyloidosis Scabies |
|
|
What are two major categories of deep pyoderma?
|
Folliculitis/furunculosis
Abscesses |
|
|
What is the major pathogenic factor involved in furunculosis?
|
Rupture of follicle causes release of keratin which serves as a nidus for an extraordinary inflammatory response
|
|
|
What is the major pathogenic genus in bacterial granulomatous dermatitis? What species does it commonly affect? Is there zoonotic potential?
|
Mycobacterium spp. affects cats; can be zoonotic
|
|
|
What causes pigeon fever in horses?
|
Corynebacterium pseudotuberculosis
|
|
|
What is a major cause of diamond skin disease in pigs? Is this zoonotic?
|
Erysipelothrix rhusiopathiae; zoonotic potential!
|
|
|
What are some major genera causing systemic infections involving the skin?
|
Streptococcus
Staphylococcus Erysipelothrix Clostridium |
|
|
What is the most common fungal pathogen causing cutaneous mycoses?
|
Microsporum spp. (Ringworm)
|
|
|
Name three genera of fungi causing superficial dermatitis?
|
Candida
Malassezia Microsporum |
|
|
Why are subcutaneous mycoses difficult to treat? What is an example of an agent causing subcutaneous mycosis?
|
very destructive!
Sporothrix schenckii |
|
|
What viral disease strikes rabbits? What are the signs?
|
Myxomatosis presents with bletheral and genital myxedema and appendicitis
|
|
|
What condition does parapoxvirus cause in animals? In humans? When is it fatal?
|
Ecthyma contagiosum (fatal when interferes with suckling feeding)
Orf in humans |
|
|
T or F:
Beak and feather disease is caused by the avian pox virus. |
False!
By the beak and feather disease virus! |
|
|
What are some signs of canine distemper infection?
|
Demyelinating encephalitis
Interstitial pneumonia Necrotizing enteritis Impetigo (secondary) Hyperkeratosis of foot pads and planum nasale |
|
|
What is another name for vesicular dermatitis? What is it caused by?
|
Foot and Mouth Disease;
Caused by a picornavirus (FMDV) |
|
|
What does ovine herpesvirus 2 cause?
|
Malignant catarrhal fever
|
|
|
What should a major differential be for deep suppurative dermatitis and panniculitis?
|
Bacterial (S. aureus)
|
|
|
What should a major differential be for deep eosinophilic dermatitis and panniculitis?
|
Parasitic (Habronema spp. larvae)
|
|
|
What should a major differential be for deep granulomatous dermatitis and panniculitis?
|
Fungal infection
|
|
|
What genus of parasitic mite has zoonotic potential?
|
Sarcoptidae
|
|
|
T or F:
Discoid lupus erythematous affects only the skin. |
True!
|
|
|
What are the possible epithelial tumors of the skin?
|
Papilloma
Trichoblastoma Squamous cell carcinoma Apocrine gland tumor Hair follicle tumor cyst |
|
|
What skin tumor is common in young dogs? What is the prognosis?
|
Cutaneous histiocytoma; might spontaneously regress
|
|
|
Boxers are prone to which tumor type?
|
Mast cell tumor
|
|
|
Cats are prone to which iatrogenically-induced tumor? What is the prognosis?
|
Vaccine-associated sarcoma
Pretty bad prognosis... |
|
|
What is a common dermal to subcutaneous neoplasm in all dogs? What is the prognosis?
|
Hemangioma; good prognosis with complete excision
|
|
|
What is a common tumor in glabrous skin of dogs? What is the prognosis?
|
Cutaneous hemangiosarcoma; good prognosis after removal
|
|
|
Where are common regions to find visceral hemangiosarcomas in dogs? What is the prognosis?
|
Heart (R. auricle), spleen, liver
Poor prognosis |
|
|
T or F:
Oral melanomas are almost always malignant. |
True!
|
|
|
What neoplasms are common in white horses?
|
Melanomas
|
|
|
What is the most common tumor in the horse? What is the cause of this tumor?
|
Equine sarcoid; associated with bovine papillomavirus
|
|
|
What are two common tumors of the nail bed in dogs?
|
Squamous cell carcinoma
Melanoma |
|
|
T or F:
Equine sarcoids do not metastasize. |
True
|
|
|
What is a common neoplasm of all young animals?
|
Papilloma
|
|
|
What is remarkable about feline squamous cell carcinoma of the toe?
|
Usually metastasized from a bronchocarcinoma
|
|
|
Where are common regions to find squamous cell carcinoma in the horse?
|
3rd eyelid, penis, vulva, udder
|
|
|
Where are common regions to find squamous cell carcinoma in the sheep and cattle?
|
eyelid (cancer eye)
|

