![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
76 Cards in this Set
- Front
- Back
|
What are the 2 forms that a single dimorphic Fungi can live in? What is the major difference between these?
|

Yeast - unicellular (smooth individual colony)
Molds - multicellular (entangled filamentous) |
|
|
What are some gen characteristics of fungi?
|
Rigid cell wall (glucan and chitin)
Haploid No chlorophyll |
|
|
How do yeast reproduce?
|
through budding
|
|
|
What are pseudohyphae?
|

These are long chains of cells formed from yeast that bud but remained attached. the cytoplasma are NOT connected. This is different from septated hyphae.
|
|
|
What are the 2 types of molds?
|
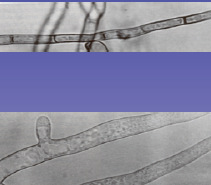
Septated hyphae
and Non septated hyphae *typical of zygomycetes" |
|
|
What differentiates the 2 types of molds?
|
septated hyphae - have membranes that separate each cell
& non septated - lack the dividing membranes and thus are multinucleated cells |
|
|
What does a dimporhic mold refer to?
|
Its ability to live in 2 different forms.
- Often they are temperature dependent |
|
|
What are unique substances in fungi walls?
|
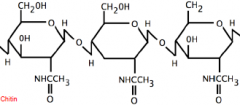
ergosterol and chitin
|
|
|
How are the cell wall properties effect the ability of antibiotics to work on fungi?
|
Antibiotics are often not functional against fungi
- No peptidoglycans (chitin instead) & Antifungals target -Ergosterol ect |
|
|
What are mechanisms of antifungals?
|
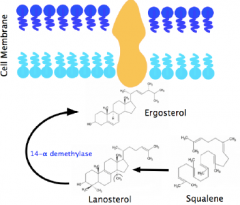
They target ergosterol
- Ketaconazole = inhibit ergosterol synthesis - Amphoteracin B = pore forming at site of ergosterol - Nystatin = pore forming at site of ergosterol (topical including GI topical) |
|
|
How can fungal infections be categorized?
|
Based on how they infect and where
|
|
|
What are the fungal categories? (4)
|
Cutaneous
Subcutaneous Systemic Oppurtunistic |
|
|
Major function Fungi in nature and how relate to metabolism?
|
NO chloroplasts
Decomposers as carbon source + Nitrate/NH3 as Nitrogen source |
|
|
What type of patients typically get mycoses?
|
immunocompromised
|
|
|
What type of infections are typically caused by fungi
|
mycoses vary greatly in their manifestations but tend to be subacute to chronic with indolent, relapsing features.
- acute diseasae is rare |
|
|
What is organization of fungi?
|
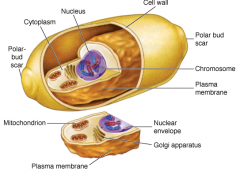
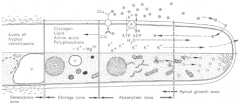
A yeast cell showing the cell wall and internal structures of the fungal eukaryotic cell plan
- The rigid cell wall external to cytoplasmic membrane has a different composition |
|
|
What are the differences in membrane sterol compositions between fungi and humans?
|
Fungi - ergosterol
Humans - cholesterol |
|
|
What is the significance of fungi having eukaryotic organization?
|
More of the structures are similar to human cells and HARDER to differentiate from non pathogenic, self cells
|
|
|
What is the composition of fungal cell walls?
|
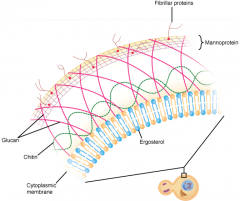
Mannan, glucan, & chitin
-------------------- The fungal cell wall. The overlapping mannan, glucan, chitin, and protein elements are shown. Proteins complexed with the mannan (mannoproteins) extend beyond the cell wall. |
|
|
What bactrerial structures are fungi missing that are found in bacteria?
|
Different in that bacterial cells in that it does not contain peptidoglycan, glycerol or ribitol teichoic acids, or lipopolysaccharide
|
|
|
Gram-positive envelope.
|
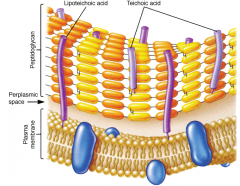
Major components of Gram-positive walls are peptidoglycan and teichoic acid
-- Peptidoglycan comprises glycan chains cross-linked by peptide chains |
|
|
Gram-negative envelope.
|
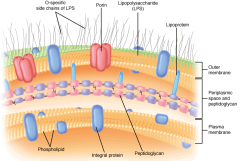
Gram-negative outer membrane is phospholipoprotein bilayer, of which the outer leaflet is LPS endotoxin
|
|
|
What are the major determinants of serological specificty in fungi?
|
Mannoproteins are mannose-based polymers (mannan) found on the surface and in the structural matrix of the cell wall, where they are linked to protein.
|
|
|
Chitin function in yeast v. mold
|
In filamentous mold - form the wall that is insulble, rigid, and inert
- In yeast - forms cross septa & channels so nuclei can pass to progeny |
|
|
What is the difference in function betw/ Glucans and mannans?
|
Glucans - w/ chitin give rigidity to cell wall
- mannan is on surface and gives serological differences |
|
|
Are fungi aerobeic or anaerobic?
|
All that cause disease in humans are strict aerobes.
|
|
|
What are conidia? What methods are they produced by?
|
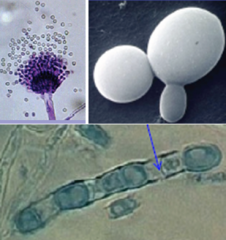
These are the reproductive elements in asexual (anamorphs). Haploid under go mitosis
- Produced by budding, fragmentation, or sporulation. (iamge) |
|
|
What are spores? Haploid or diploid?
|
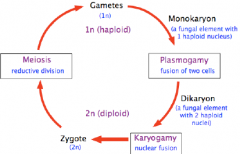
These are reproductive structures in the sexual (telomorph)
Haploid combine to become diploid and divide by meosis |
|
|
What are the mechanisms in asexual and sexual reproduction? What are the products?
|
Asexual reproduction forms conidia by mitosis
- Meiosis forms sexual spores in specialized structures |
|
|
What are Blastoconidia and conidophores?
|
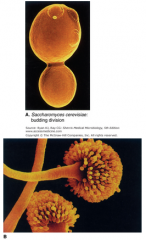
Yeast and mold forms of fungal growth. A. This oval yeast cell is budding to form a blastoconidium. Scars from the separation of other blastoconidia can be seen on other parts of the cell. B. The mold form is highly variable. Here tubular stalks called condiophores arising from hyphae (not seen) bear a "Medusa head" crop of reproductive conidia
|
|
|
Describe the structure of septated/nonseptated hyphae & pores that join these structures
|
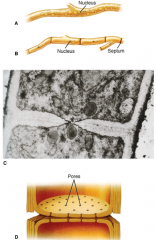
Hyphae. A. Nonseptate hyphae with multiple nuclei. B. Septate hyphae divide nuclei into separate cells. C. Electron micrograph of septum with a single pore. D. Multipore septum structure.
|
|
|
What is the fluffy portion of mold? How else may they grow?
|
The more visible surface growth may assume a fluffy character as the mycelium becomes aerial.
Hypahe may grow along, into or above the substrate |
|
|
What is the function of the fluffy component of mold?
|
The aerial hyphae bear the reproductive structures of this class of fungi.
|
|
|
What is the importance of conidia?
|
Morphology of reproductive conidia and spores used for identification
|
|
|
What are the different conidia and what defines them?
|
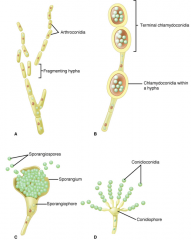
(CASS)
------------------------------- Asexual mold forms. A. Arthroconidia develop within the hyphae and eventually break off. B. Chlamydoconidia are larger than the hyphae and develop with the cell or terminally. C. Sporangiocondia are borne terminally in a sporangium sac. D. Simple conidia arise directly from a conidiophore |
|
|
What stages are typical in a temperature dimorphic fungi?
|
Yeast phase growth requires conditions similar to those of the physiologic in vivo environment, such as 35° to 37°C incubation and enriched medium. Mold growth requires minimal nutrients and ambient temperatures.
|
|
|
Do we typically see molds in humans? Why and give example?
|
No, due to the host temperature that promotes yeast
---------------- Histoplasma capsulatum. They are understandably complex, given the dramatic change of milieu encountered by the fungus when its mold conidia float from their soil habitat to the pulmonary alveoli. Conversion to the yeast phase is then triggered by the host temperature (37°C) and possibly by other aspects of the new environment. |
|
|
Is dimorphism reversible?
|
yes, this is why it is not considered a embryogenesis type proceess
|
|
|
What is unique about the medically releavnt fungi? How does this effect classification? (NEED TO SHORTEN ANS)
|
A major issue in classifying the medically important fungi using these groups is that for most species, no teleomorph form has been demonstrated. It may be that because of an advantage for pathogenicity, persistently anamorph clones were selected during evolution, or that the conditions for natural production of spores are just yet to be met.
|
|
|
What do we do about the difficulty in classifying fungi? So then what do we do about it?
|
we make up artificial groups
- types of tissues they parasitize and the diseases they produce, rather than on the principles of basic mycologic taxonomy. |
|
|
What about Superficial fungi?
-Name? -Common examples? |
superficial fungi, such as the dermatophytes, cause indolent lesions of the skin and its appendages, commonly known as ringworm and athlete's foot.
|
|
|
What about subcutaneous fungi?
-Where do these typically spread to? |
subcutaneous pathogens characteristically cause infection through the skin, followed by subcutaneous spread, lymphatic spread, or both.
|
|
|
What about opportunistic fungi?
-where do these reside? -type of host? |
The opportunistic fungi are those found in the environment or in the normal flora that produce disease under certain circumstances and in the compromised host.
|
|
|
What about systemic fungi?
-comparative virulence? -type of host? |
The systemic pathogens are the most virulent fungi and may cause serious progressive systemic disease in previously healthy persons. They are not found in the normal human flora.
|
|
|
Why is KOH used in fungal preps?
|
KOH digests tissue, but not fungal wall
|
|
|
Describe how and what ringworm could be diagnosed?
|
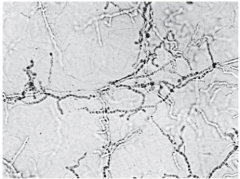
--------------------
KOH (potassium hydroxide) preparation. Scalp scrapings from a suspected ringworm lesion have been mixed with 10% KOH and viewed under low power. The skin has been dissolved, revealing tubular branching hyphae.` |
|
|
How are fungi visualized?
|
fungi can be observed under the light microscope with or without staining
|
|
|
How are fungi cultured?
|
They grow slowly
Grow under normal condition but bacteria outpace the Selective media make use of antimicrobics Typically grow @ 30c |
|
|
What are hyphae?
|
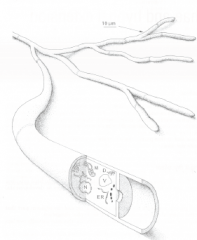
Each of the branching filaments that make up the mycelium of a fungus. May be septated or not. Growth occurs at the tip
|
|
|
What are mycelium?
|
Sun of the hyphae. The vegetative part of a fungus, consisting of a network of fine filaments (hyphae)
|
|
|
(Bactrerial) What is the difference betw/ lipotechoic acid and techoic acid?
|
lipotechoic acid has lipid that allows it to associate with the inner cell membrane. Techoic acid does not have the ability to associate w/ lipid bilaye
|
|
|
Are fungi in flora?
|
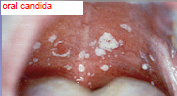
yes, these might be the opportunistic classified fungi
Primarily thing Candida Albicans. Candida is indigenous to GI tract |
|
|
What type of pathogenesis (general) that fungi cause?
|
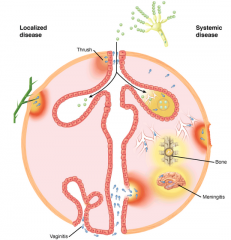
----------------------
Fungi system view. Localized disease (left) is produced by local trauma or the superficial invasion of flora resident on the oropharyngeal (thrush), gastrointestinal, or vaginal mucosa. Systemic disease (right) begins with inhalation of conidia followed by dissemination to other sites. |
|
|
What is the immunological response to Fungi?
|
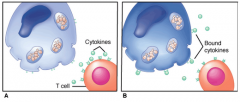
--------------------------
Immunity to fungal infections. A. Pathogenic fungi are able to survive and multiply slowly in non-activated macrophages. B. When macrophages are activated by cytokines from T-cells the growth is restricted and the fungi digested. |
|
|
What are the majority of pathogenic fungi? What are some examples?
|
Oppurtunistic
Examples - Aspergillus, Zygomycetes, Pneumocystis |
|
|
What is the ability to adhere associated with in fungi?
|
Virulence
|
|
|
How do fungi adhere?
|
Adherence usually requires a surface adhesin (mannoprotein) on the microbe and a receptor on the epithelial cell. (fibronectin)
I.e. Candida Albicans - mannoprotein (common in many) |
|
|
What is a virulence factor in fungi that infect lungs?
|
Small so they are suspended in air and reach terminal bronchioles
|
|
|
What is invasion by fungi associated with?
|
It is associated with enzymes secrete from tip of hyphae.
----------------- Extracellular enzymes (eg, proteases, elastases) are associated with the advancing edge of the hyphal form of Candida and with the invasive forms of many of the dimorphic and other pathogenic fungi. Although these enzymes must contribute to some aspect of invasion or spread, |
|
|
Do fungi have exotoxins? Then what causes necrosis and infarction?
|
No, it has not been oberved in vivo
---------- presence of necrosis and infarction in the tissues of patients with invasion by fungi such as Aspergillus suggests a toxic effect, direct evidence is lacking. |
|
|
What causes most of the injury in fungal infections?
|
The injury caused by fungal infections seems to be due primarily to the destructive aspects of delayed-type hypersensitivity (DTH) responses as a result of the inability of the immune system to clear the fungus. >
|
|
|
What type of infection do fungal parralel
|
In this respect, fungal infections resemble tuberculosis more than any other disease
|
|
|
What is the role of innate immunity to fungi?
|
High level, which is why most fungi are oppurtunistic
|
|
|
What innate immune mechanisms are antifungal?
|
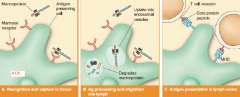
1. professional phagocytes (neutrophils, macrophages, and dendritic cells)
2. complement system 3. pattern recognition receptors - lectin like (binds glucan) |
|
|
What mediates the the resolution of fungal infection?
|
In most instances in which it has been investigated, the actions of neutrophils and TH1-mediated immune responses have been found to be of primary importance in this resolution. (T cell mediated response)
|
|
|
What is the role of adaptive humoral immunity to fungal infections?
|
Most fungal infections will have some Ab formation but response is dominated by CMI
-Cryptococcous neoformans = Ab help -Coccidioidomycosis Imitus = Ab bad (dissemination/worsening) |
|
|
What type of pts get severe systemic fungal infections?
|
Systemic neutropenia or depressed Th1 (T cell) repsonses
|
|
|
How do some fungi escape PMNs?
|
Fungi that escape neutrophils grow slowly in macrophages
|
|
|
What are the steps of cellular response to fungi and what effect do they have?
|
Fungi
Interaction DC & macrophages favors production IL4 & IFNgamma -> CD4 become Th2 cells -> activate B cells to secrete neutralizing Ab (killing) [extracellular microbes] ***Turning point when host fight fungal infection*** Th1 response - T cells activate macrophages via IFNgamma & . Now macrophages are able to restrict intracellular growth of fungi. Any secreted Ab are for opsonizing pathogens |
|
|
What is the important mechanism to attack fungi?
|
The CMI or Th1 response that is depndent on macrophages and their activation
|
|
|
What are the sexual fruiting bodies?
|
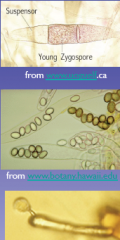
Top - zygospore (yoke)
Mid - Ascospore (sac) Bot - basidiospore (club) |
|
|
How are glucans used by medical personelle?
|
Measure circulating levels Beta glucan to detect invasive systemic fungi
Glucan Synthetase inhibitors - antifungals |
|
|
Summary medical fungi
|
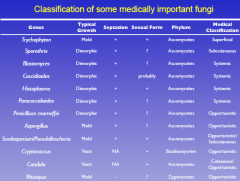
|
|
|
What are the endemic fungi?
|
Blastomycetes
Coccidioides Cryptococcus Histoplasma |
|
|
What are the targets for antifungals? (7)
|
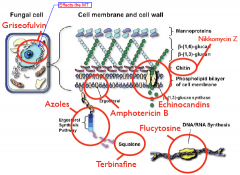
|
|
|
What are the 7 antifungal classes?
|
Flucytosine
Terbinafine Azoles Amphoteracin B Echinocandins Nikkomycin Z Griseofulvin |

