![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
110 Cards in this Set
- Front
- Back
|
What is the bradycardia protocol for?
|
Slow heartbeat with negative signs and/or symptoms that are caused by the bradycardia?
|
|
|
What is bradycardia?
|
A heartbeat slower than 60 BPM
|
|
|
What does bradycardia look like?
|
It depends on what kind it is
|
|
|
What are the different kinds of bradycardia?
|
Sinus Bradycardia
??? |
|
|
What does sinus bradycardia look like?
|
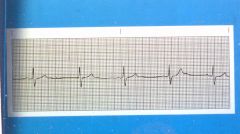
|
|
|
What is the first step in the bradycardia algorithm?
|
BSI
Scene Safe Additional Resources Check LOC Look, listen, and feel... If no breathing, reposition airway... Look, listen, and feel again... If still no breath, begin rescue breathing? Check pulse... If no pulse, begin CPR... Hook up ECG, and figure out what the rhythm is??? (These are your basic/primary ABCD's?) Then start Advanced/Secondary ABCD's? |
|
|
What is the mnemonic for the bradycardia algorithm?
|
Pacing
Always Ends Danger |
|
|
What does "Pacing Always Ends Danger" stand for?
|
Pacing
Atropine Epinephrine Dopamine |
|
|
If there is a high degree block, when do you pace?
|
Immediately
|
|
|
What is a high degree block?
|
Third Degree/Complete Block
Second Degree Type II (Mobitz Type II) |
|
|
What does a third degree/complete block look like?
|
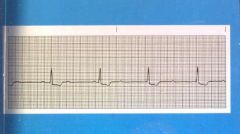
|
|
|
What does a Second Degree Type II/Mobitz Type II look like?
|

|
|
|
If you need to pace, what should you think about doing while you are getting ready?
|
Atropine
Epinephrine (If necessary) Dopamine (If necessary) |
|
|
When do you use atropine for bradycardia?
|
When there is symptomatic bradycardia caused by the slow rate...can use either while you are getting ready to pace, or if pacing doesn't work
|
|
|
If you give atropine for bradycardia, how much should you give?
|
0.5mg IV or IO push every 3-5 minutes
|
|
|
If you give atropine for bradycardia, what is the most you should give?
|
3mg
|
|
|
What is the first drug you should give for symptomatic bradycardia?
|
Atropine
|
|
|
What are other drugs can you use for symptomatic bradycardia after you Atropine?
|
Epinephrine
Dopamine |
|
|
When should you use epinephrine or dopamine for bradycardia?
|
Either while you are getting ready to pace AFTER you use Atropine, or AFTER pacing doesn't work AND you use Atropine
|
|
|
If you give epinephrine for symptomatic bradycardia, how much should you give?
|
2-10 ug/minute
|
|
|
If you give dopamine for bradycardia, how much should you give?
|
2-10 ug/kg/minute
|
|
|
How should you use epinephrine and dopamine in a patient with symptomatic bradycardia?
|
Very carefully
|
|
|
If the bradycardia protocol doesn't work, what may that mean?
|
That it is a sign and/or symptom of another problem, and that may be what you need to focus on?
|
|
|
If the bradycardia algorithm doesn't work, what do you do?
|
Problem Search/Differential Diagnosis
|
|
|
If TCP doesn't work, what can be done?
|
Transvenous pacing by an expert
|
|
|
What is a high degree block?
|
Type II Second Degree Block
Third Degree/Complete AV Block? |
|
|
When should you pace and/or give drugs for bradycardia?
|
ONLY IF THERE ARE SIGNS AND/OR SYMPTOMS
|
|
|
What is the drug of choice for symptomatic bradycardia?
|
Atropine
|
|
|
If a person has a high degree block, you should immediately give atropine and then pace, true or false?
|
False...you should pace immediately!
|
|
|
Are blocks considered bradycardia?
|
???
|
|
|
What is bradycardia?
|
A heartbeat <60 BPM
|
|
|
If a patient has symptomatic bradycardia, what do you do?
|
Open the person's airway, and make sure it stays open
Help them breath if necessary Give oxygen Hook up ECG, try to figure out what the heartbeat rhythm is, and watch Check blood pressure, pulse ox, et cetera At least establish and INT, if not a complete IV |
|
|
After checking the airway, breathing, et cetera, what do you do?
|
You see if the person has signs and/or symptoms of shock/inadequate perfusion caused by the slow heart beat?
|
|
|
What are some examples of signs and/or symptoms of shock caused by bradycardia?
|
Sudden Altered Mental Status
Chest pain that doesn't stop (Angina) Hypotension Other signs and/or symptoms of shock |
|
|
If there is adequate perfusion and/or the patient appears stable what do you do?
|
Watch the person closely, and transport?
|
|
|
If the patient is in shock (= Unstable) what do you do?
|
PACE IMMEDIATELY?
|
|
|
What do you do if there is a high degree block?
|
Pace IMMEDIATELY!
|
|
|
While you are getting ready to pace or if pacing doesn't work, what do you do?
|
Think about using Atropine
|
|
|
If you choose to use atropine, how much do you give?
|
0.5mg IV or IO push
|
|
|
If you give 0.5 mg Atropine IV or IO push, how many doses can you give?
|
Up to six
|
|
|
If you choose to give atropine for symptomatic bradycardia, what is the most you can give?
|
3mg
|
|
|
If Atropine doesn't work, what do you do?
|
Pace or epinephrine?
|
|
|
As a second choice after Atropine, what else can you do while you get ready to pace and/or if pacing doesn't work?
|
Give epinephrine or dopamine
|
|
|
If you choose to give epinephrine, how much do you give?
|
2-10 ug/min?
|
|
|
What is the drug of choice for bradycardia?
|
Atropine?
|
|
|
If you choose to use dopamine, how much do you use?
|
2-10 ug/kg/min
|
|
|
If pacing, atropine, epinephrine, and dopamine don't work, what do you do?
|
Get ready for transvenous pacing by an expert, and only if allowed by policy
Try to figure out if anything is helping cause the bradycardia, and treat that if possible Contact the supervising doctor |
|
|
What do you do if pulseless arrest happens?
|
Use the pulseless arrest algorithm
|
|
|
What are some of the things that might help cause bradycardia?
|
Hypovolemia
Hypoxia Acidosis Hypokalemia Hyperkalemia Hypoglycemia Hypothermia Poisons Cardiac Tamponade Tension Pneumothorax Clot (Thrombosis) in the heart Clot (Thrombosis) in the lungs Trauma (Which can cause hypovolemia, higher ICP, et cetera) |
|
|
What is the bradycardia algorithm used for?
|
Bradycardia with circulatory compromise that is caused by the slow heart beat
|
|
|
What are the signs and/or symptoms of circulatory compromise?
|
Mild hypotension
Pulmonary congestion CHF Hypotensive shock |
|
|
What are the signs and/or symptoms of circulatory compromise?
|
Shortness of breath
Chest pain Altered LOC |
|
|
When might you find symptomatic bradycardia?
|
During the Basic/Primary ABCDs?
|
|
|
What is the bradycardia algorithm part of?
|
Advanced/Secondary ABCDs?
|
|
|
What are the Advanced/Secondary ABCDs?
|
Airway
Breathing Circulation Differential Diagnosis |
|
|
What is the difference between the Basic/Primary ABCDs and the Advanced/Secondary ABCDs?
|
The primary is a basic assessment, and the secondary is an advanced assessment. Also, the "D" in the primary stands for "Defibrillation", and the "D" in the secondary stands for "Differential Diagnosis".
|
|
|
What is the order of events?
|
Discover problem during "Primary C-ABCDs"
Begin "Secondary C-ABCDs", and if problem not solved by the end of it then use transcutaneous pacing, atropine, epinephrine, and dopamine if necessary |
|
|
If there is serious circulatory compromise caused by the slow heart beat (Especially high degree blocks), what is the first thing you do?
|
Get ready to pace!!!
|
|
|
When is it very important to get ready to pace?
|
When there is a high degree block
|
|
|
What is a high degree block?
|
Second Degree AV Block Type II?
Third Degree Block? |
|
|
What do you do while you are getting ready to pace using electricity?
|
Depending on the situation, use drugs to pace?
|
|
|
What does it mean to "Pace" the heart?
|
To see how fast it is going (This is wrong?)?
|
|
|
What drugs do you use?
|
Atropine, epinephrine, and/or dopamine
|
|
|
Which drug do you use first?
|
Atropine
|
|
|
What is atropine considered?
|
The drug of choice for unhealthy slow heart beat
|
|
|
How much atropine do you give?
|
0.5 mg IV or IO Every 3-5 minutes (max. 3mg)
|
|
|
How often should you give atropine?
|
Every 3-5 minutes
|
|
|
What is the most atropine you should give?
|
3mg
|
|
|
If atropine doesn't work, what do you do?
|
Give epinephrine
|
|
|
How much epinephrine should you give?
|
2-10 µg/min
|
|
|
If epinephrine doesn't work, what should you do?
|
Give dopamine
|
|
|
How much dopamine should you give?
|
2-10 µg/kg/min
|
|
|
If dopamine doesn't work, what should you do?
|
Use transcutaneous pacing
|
|
|
What is transcutaneous pacing?
|
Pacing through the skin?
|
|
|
What do you do if TCP doesn't work?
|
Have an expert do transvenous pacing
|
|
|
What is transvenous pacing?
|
Pacing in the veins
|
|
|
What do you do if TCP and the drugs don't work?
|
It may be caused by some other condition, so use "Differential Diagnosis" to try to figure it out
|
|
|
What is primary drug for slow heart beat?
|
Atropine
|
|
|
What are the secondary drugs for slow heart beat?
|
Epinephrine
and Dopamine |
|
|
When should you use epimephrine and/or dopamine?
|
If atropine and/or TCP doesn't work
|
|
|
How should you use epinephrine and dopamine?
|
Very carefully!
|
|
|
What is pacing?
|
The heart's natural pacemaker is the sinoatrial node, but if that is not working correctly then an internal or external artificial "pacemaker" can be used to attempt to set the speed of the heart, or pace, to normal
|
|
|
What are the modes of transcutaneous pacing?
|
Nondemand (Asynchronous)
Demand |
|
|
What does etiology mean?
|
The cause (s) of a disease
|
|
|
What is pathophysiology?
|
A change in the body that is connected to and/or caused by a sickness, disease, and/or injury
|
|
|
What is bradycardia?
|
A heartbeat < 60 BPM...
|
|
|
What is tachycardia?
|
A heartbeat >100 BPM?
|
|
|
What are some of the first things you do to treat bradycardia?
|
Make sure the airway is open and stays that way.
Help them breathe if necessary. Give oxygen. Hook up ECG Figure out what heart rhythm the patient has. Get blood pressure. Get pulse ox. Establish an I.V. (At least a port?). |
|
|
What are some signs and/or symptoms of not enough nutrient/gas exchange (Perfusion) that can be caused by bradycardia that you need to be looking for?
|
Sudden altered mental status.
Chest pain that doesn't stop. Low blood pressure. Other signs of shock, et cetera. |
|
|
After your first treatments, what do you do?
|
Figure out if there are any signs and/or symptoms of not enough nutrient/gas exchange (Perfusion), and then figure out if they could be caused by bradycardia?
|
|
|
If there IS enough nutrient/gas exchange (Perfusion), what do you do?
|
Watch the patient closely, keep re-checking them, and transport?
|
|
|
After your initial interventions, if there is not enough nutrient/gas exchange (Perfusion), what do you do?
|
Get ready for transcutaneous pacing.
Think about giving atropine while waiting for the pacer. Think about giving epinephrine or dopamine while waiting for pacer, or if pacer doesn't fix the problem. |
|
|
If a person has a high degree block, you should wait five minutes before pacing, true or false?
|
False, you need to do it ASAP.
|
|
|
While you are waiting on the pacer, if you decide to give atropine how much should you give?
|
0.5mg via I.V.
|
|
|
If you decide to give atropine via I.V., what is the most you should give?
|
3 mg in 0.5mg doses
|
|
|
If you give atropine and it doesn't work, what do you do?
|
Begin pacing.
|
|
|
If you decide to give epinephrine while waiting on the pacer, how much should you give?
|
2-10 ug/minute (Via infusion)
|
|
|
If you decide to give dopamine while waiting on the pacer, how much should you give?
|
2-10 ug/kg/minute (Via infusion)
|
|
|
If a patient doesn't have enough nutrient/gas exchange (Perfusion), what drug(s) can you give as an alternative while you are waiting on the pacer?
|
Atropine, epinephrine, or dopamine.
|
|
|
If transcutaneous pacing doesn't work, what drug(s) can you give?
|
Give epinephrine or dopamine.
|
|
|
If transcutaneous pacing and/or giving atropine, epinephrine, or dopamine doesn't fix the problem, what do you do?
|
Use transvenous pacing.
Treat causes. Call medical direction. |
|
|
When should you use transcutaneous pacing to treat bradycardia?
|
When it causes signs and symptoms of shock.
|
|
|
All bradycardia is abnormal, true or false?
|
False, some athletes have slower heart beats.
|
|
|
What is transcutaneous pacing?
|
A temporary way of pacing a patient's heart in an emergency. Is done by giving electricity through the patient's chest from the outside in. This stimulates the heart, and causes it to contract.
|
|
|
What is another name for transcutaneous pacing?
|
External Pacing
|
|
|
What is transvenous pacing?
|
A form of pacing used to treat bradycardia, and is done by threading a pacing electrode through a vein into the right atrium, right ventricle, or both.
|
|
|
What is another name for transvenous pacing?
|
Endocardial Pacing
|
|
|
When can you use transvenous pacing?
|
When a patient has a slow heartbeat, and by subcutaneous pacing and/or drugs don't work.
|
|
|
What do you do if pulseless arrest develops?
|
Use the "Pulseless Arrest Formula".
|
|
|
What are some things that can cause bradycardia?
|
Not enough fluid in the body (Hypovolemia).
Not enough oxygen (Hypoxia). Too many charged hydrogen particles (Acidosis). Too much or too little potassium (Hyperkalemia or Hypokalemia) Not enough sugar (Hypoglycemia) Not enough heat (Hypothermia) Poisons Fluid in the sac that lines the heart (Cardiac Tamponade) Tension Pneumothorax Blood Clot in heart or lungs (Thrombosis). Trauma |

