![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
44 Cards in this Set
- Front
- Back
|
what are the major functions of the female reproductive system |
produce sex hormones produce functioning gametes (ova) support and protect developing embryo |
|
|
what are the organs of the female reproductive system |
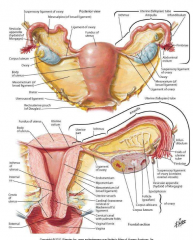
uterus uterine tube/fallopian tube ovaries vagina external genitalia |
|
|
generally describe the ovary |
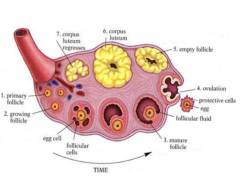
size and shape of almond tend to shrink after menopause produce eggs (ova) every female is born with lifetime supply (~2-400,000 in each) produce hormones: estrogen, progesterone, testosterone |
|
|
describe the process of oogenesis |
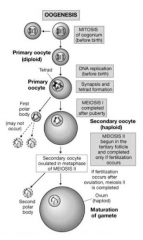
primary oocytes formed before birth at puberty, primary oocytes in metaphase I recommence development, few at a time, once a month completes meiosis I, forms large secondary oocyte and small polar body proceeds to metaphase of meiosis II and stops restarts with sperm entry |
|
|
describe the 4 layers of the ovary
|
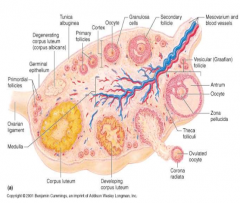
epithelium (covering) tunica albuginea cortex: germ cellls (ovum) in follicles medulla: supporting tissues |
|
|
describe the cortex of the ovary |
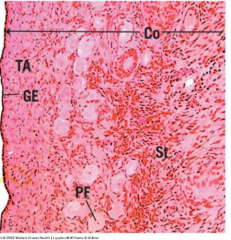
contains ovarian follicles covered by simple cuboidal epithelium (germinal epithelium) just under that is tunica albuginea- fibrous connective tissue |
|
|
describe the medulla of the ovary |
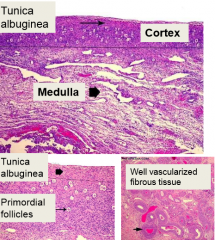
well-vascularized fibrous tissue help contractile function during extrusion of egg at ovulation |
|
|
describe the follicle |
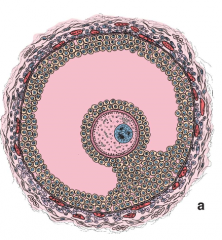
develops and grows around oocyte to support oogenesis contains single oocyte and supporting cells and fluid filled space in layers granulosa cells antrum theca cells (interna/externa) cumulus oophorious with egg surrounded by corona radiata |
|
|
describe the zona pellucida |
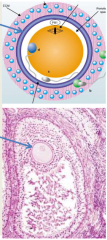
glycoprotein membrane surrounding oocyte first appears in unilaminar primary oocytes secreted by oocyte and follicular cells binds to spermatozoa and initiates acrosome reaction and fertilization |
|
|
describe granulosa cells |
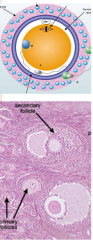
proliferates with oocyte within developing follicles form stratum granulosum antral follical mural granulosa cells- endocrine, produce steroid hormones and other ligands cumulus cells- support oocyte development androgens--> estradiol following ovulation, granulosa lutein cells produce progesterone |
|
|
describe the antrum |
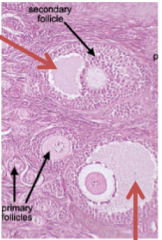
follicular fluid space in secondary follicle fluid is released with oocyte at ovulation 'carries' oocyte out of follicle helps enter into fallopian tube |
|
|
describe theca interna and externa |
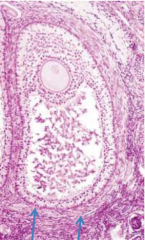
interna: inner epithelium layer surrounding developing follicle in ovary responds to leutenizing hormone to synthesize/secrete androgens transported to glomerulosa cells which process it to estrogen externa: outer layer surrounding developing follicle connective tissue cells, smooth muscle, collagen |
|
|
describe the process of folliculogenesis |
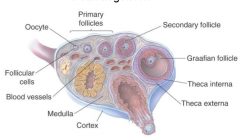
at birth, lots of primary oocytes with 1 layer of flat, squamous epithelium (no zona pellucida) epithelium becomes cuboid-- primary follicle become stratified, columnar cavities appear-- secondary follicle become fully mature, Graafian follicle fuse with membrane and release oocyte |
|
|
describe the primordial follicle |
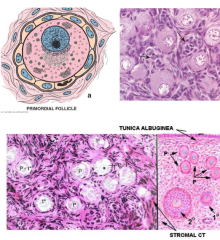
primary oocyte surrounded by single layer of follicular cells simple squamous epithelium resting in prophase of meiosis I about 20 start maturing with each menstrual cycle, only one succeeds from either ovary, others become atretic |
|
|
describe early primary follicles |
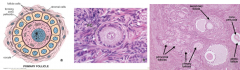
first stage of oogenesis contain primary oocyte when follicular cels become cuboidal granulosa cells divide producing multilaminar primary follical theca layer forms around no antrum |
|
|
describe late primary follicles |
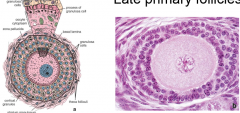
multilayered mass of granulosa cells surround oocyte
theca cells around primary follicle basal lamina between granulosa and theca interna no antrum |
|
|
describe secondary follicles |
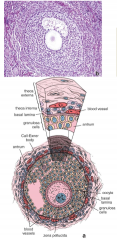
still contain primary oocyte clear theca interna and externa (interna is thick and defined, produces hormones. externa is thinner, indistinguishable from surrounding CT) zona pellucida developed antrum vavuoles appear granulosa cells on one side of follical form cumulus oophorus |
|
|
describe Graafian/mature follicles |
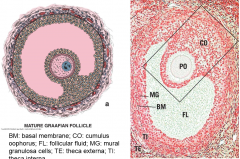
primary oocyte undergoes meiosis I, forms large secondary oocyte and small polar body theca interna and externa are thicker crescent shaped antrum corona radiata granular cells protrude into cavity to form cumulus oophorus |
|
|
describe the process of fertilization |
sperm first penetrates corona radiata contacts zona pellucida, acrosome reaction triggered penetrates zona pellucida, enters perivitelline space. attaches/enters plasma membrane of egg sperm-egg fusion triggers meiosis |
|
|
describe the corpus luteum |
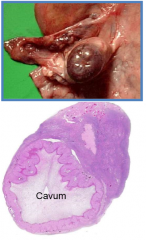
collapse of mature follicle after ovulation corpus hemorrhagicum-- hemorrhage into follicle, develops into corpus luteum if fertilized, corpus luteum persists and secretes progesterone and estrogen if not, produces progesterone but within 12 days becomes corpus albicans |
|
|
describe fallopian tubes |
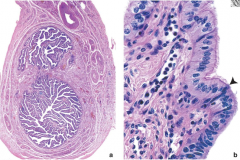
pathway for ovum to uterus site of fertilization 'oviducts' or 'uterine tubes' takes approximately 6-10 days to travel through tube to implant in uterine lining mucosa: simple columnar epithelium, ciliated cells, secretory cells |
|
|
describe fimbriae |
fringe of tissue near ovary leading to fallopian tube near ovulation, sex hormones activate fimbria so it hits ovary in gentle, sweeping motion sometimes eff is in abdominal cavity for a bit |
|
|
describe the uterus |
womb pear shaped organ, size of fist endometrium, myometrium and serosa blood enriched tissue that sloughs off each month powerful muscles can expand for birth |
|
|
describe the layers of the uterus |
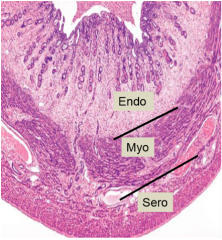
endometrium (tunica mucosa): simple columnar epithelium (stratum functionale-- shed, stratum basale-- retained) myometrium (tunica muscularis): smooth muscle serosa (tunica serosa or perimetrium) |
|
|
describe the hormones of the menstrual cycle |
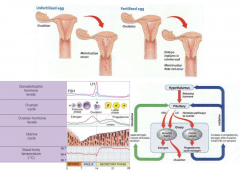
Follicle stimulating hormone (FSH)- follicle growth, estrogen production lutenizing hormone (LH)- signals ovulation estrogen- produced throughout by granuolsa and theca, build up uterine endometrium progesterone- produced in second half of cycle by corpus luteum to prepare endometrium for implantation |
|
|
describe the menstrual phase |
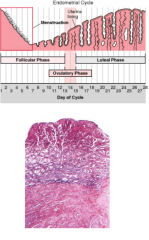
days 1-4 menstrual flow corpus luteum degenerates drop in progesterone/estrogen coiled arteries constrict and then relax ischemia and necrosis of zona functionalis (stratum functionale) shed |
|
|
describe the blood supply of the endometrium of the uterus |
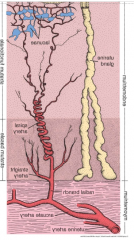
spiral arteries between stratum functionale and basale degenerate and regenerate with menstrual cycle (estrogen/progesterone) vasoconstriction followed vasodilation prior to menstruation results in necrosis of endometrium |
|
|
describe the proliferative phase |
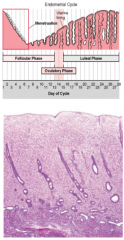
days 5-14 development of ovarian follicles epithelial cells develop microvilli and cilia with estrogen regenerate: surface epithelium, lamina propria, uterine glands, coiled arteries |
|
|
describe the secretory phase |
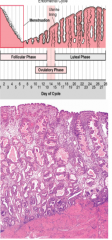
luteal phase days 15-28 after ovulation depends on corpus luteum secretion of progesterone glands become coiled and distended glands secrete glycogen and glycoprotein rich mucus enometrial lining= thickest myometrium is same prepared to receive zygote for implant |
|
|
define pseudo-decidual cells |
implantation occurs, zygote grows, lamina propria becomes decidua psuedo before implantation in preparation produce lots of glycogen |
|
|
describe implantation |
corpus luteum produces progesterone and estrogen until placenta takes over this ceases menses |
|
|
describe the cervix |
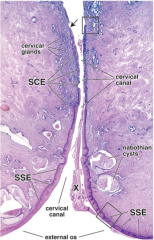
lower portion/neck of uterus endometrium contains large branched glands with low estrogen, thick and sparse mucus-- hinders sperm when egg is ready, estrogen is high, mucus becomes thin and slippery-- sperm friendly mucus forms cervical plug no spiral arteries no cilia cervical canal: simple columnar cervix: stratified squamous epithelium lots of collagen-- expands during labor smooth muscle-- contraction after labor |
|
|
describe the cervical transformation zone |
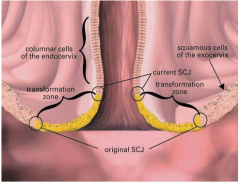
immature metaplasia between original and current squamo-columnar juctions spot of 99% of HPV related cancer pap test obtains cells from cervix (primarily transformation zone) for cytology screening |
|
|
describe the vagina |
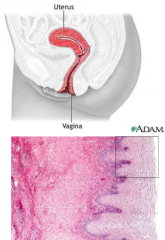
elastic, muscular canal with soft, flexible lining for lubrication and sensation connects uterus to world vulva and labia form entrance cervix protrudes in receives penis and expels menstrual flow birth canal no glands but bacteria produce lactic acid |
|
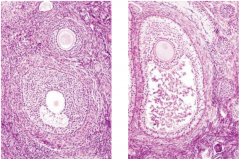
describe these cells |
secondary follicles |
|
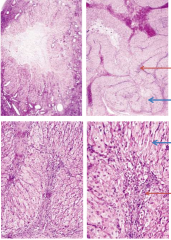
describe these cells |
corpus luteum |
|
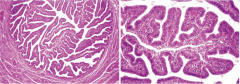
describe these cells |
fallopian tube low mag |
|
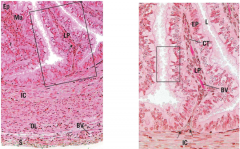
describe these cells |
fallopian tube
|
|
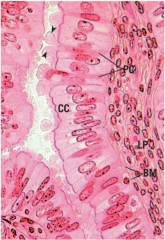
describe these cells |
fallopina tube high mag |
|
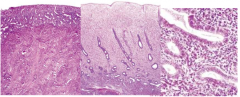
describe these cells |
uterus in proliferative stage different magnifications |
|
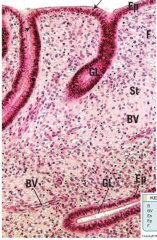
describe these cells |
uterus in proliferative stage |
|
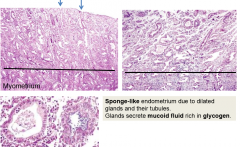
describe these cells |
uterus in secretory phase |
|
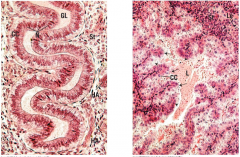
describe these cells |
uterus in secretory phase high mag pseudo-decidua cells |
|
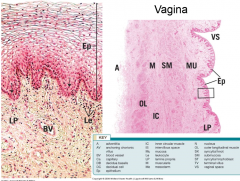
describe these cells |
vagina |

